Cervical cancer is cancer of the cervix or the entrance to the womb from the vagina. The cervix is sometimes called the uterine cervix.
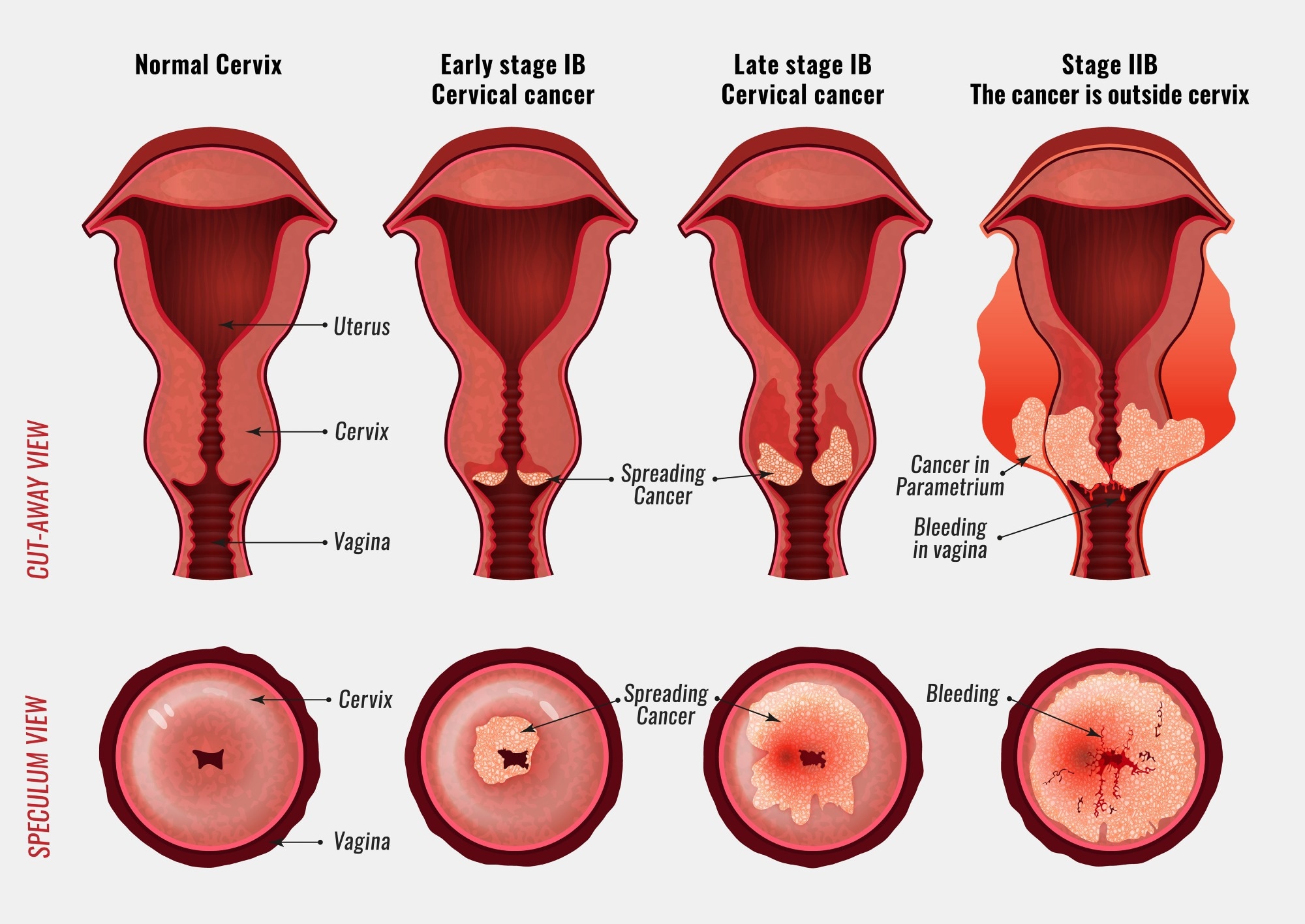 Cervical cancer development image. Image Credit: Double Brain / Shutterstock
Cervical cancer development image. Image Credit: Double Brain / ShutterstockWhat is the cervix?
The body of the uterus or the womb is like a pouch that grows to accommodate the growing baby. The cervix connects the body of the uterus to the vagina (birth canal). The part of the cervix closest to the uterus is called the endocervix. The part next to the vagina is the exocervix (or ectocervix).
Two main types of cells line the cervix. These are squamous cells (on the exocervix) and glandular cells (on the endocervix). The endocervical lining, thus, is capable of secretions. The place where these two cell types meet is called the transformation zone.
How does cancer occur?
The body is built up of trillions of cells. Each of these cells has a tightly regulated system within its DNA that controls its growth, maturity, division, and death. When this DNA undergoes damage or changes, the cells turn rogue and abnormal and grow uncontrollably, giving rise to cancers.
Most cervical cancers start in the transformation zone. The cancers usually begin in the cells lining the cervix. The normal cells first gradually develop precancerous changes that turn into cancer. These precancerous changes are called cervical intraepithelial neoplasia (CIN), squamous intraepithelial lesion (SIL), and dysplasia. These changes can be detected by the Pap test and treated to prevent the development of cervical cancer.
Screening for and symptoms of cervical cancer
Cervical cancer often has no symptoms in its early stages. This is the reason why screening for cervical cancer can help detect early cases and save thousands of lives. The cells lining the cervix undergo several changes over the years. In rare cases, these changed cells can become cancerous.
Screening tests for cervical tests are offered by the NHS to all women over 24 years old. All women between 25 and 49 must be screened every three years, and women between 50 and 64 should be screened every five years.
During screening, a small sample of cells is taken from the cervix and checked under a microscope for abnormalities. This test is commonly referred to as a cervical smear test.
The most common early symptoms include vaginal bleeding. This can occur during or after sexual intercourse or after the menopause. Although this is abnormal, bleeding may not always mean cervical cancer.
Treatment of cervical cancer
When diagnosed at an early stage, surgery is a possible method of treating cervical cancer successfully. Sometimes, just the cervix is removed, and in many cases, the complete womb is removed. This is called hysterectomy. Hysterectomy is usually opted for by women who have completed childbirth and who have attained menopause.
Radiotherapy is an alternative to surgery for some women with early-stage cervical cancer. Those with advanced cancer need chemotherapy with anticancer drugs as well as radiotherapy.
Causes of cervical cancer
Most types of cervical cancers are caused by the human papillomavirus (HPV). HPV is a very common virus that's spread during sex. There are more than 100 different types of HPV, many of which are harmless. It may lead to an asymptomatic infection or genital warts.
Two distinct strains of the HPV virus are known to be responsible for 70% of all cases of cervical cancer. They are HPV 16 and HPV 18. These HPV strains can disrupt the normal functioning of the cells of the cervix, making them dysplastic and eventually cancerous.
Most women who are infected with these two types of HPV may not get cervical cancer. This means other factors may be responsible for cervical cancer causation.
Risk factors for cervical cancer
Some of the risk factors associated with cervical cancer include:
- Sexual active heterosexual women
- Women with multiple sexual partners
- Women who are partners of promiscuous males
- Infection with human papillomavirus (HPV), predominantly types 16 and 18
- Smokers
- Lower social class
- Those with impaired immunity with HIV and those after an organ transplant
- Non-attendance at screening for cervical screening
Prevention of cervical cancer
Prevention of cervical cancer can thus be achieved by anti-HPV vaccine. The vaccine used is Gardasil or Cervarix - which provides protection against cervical cancer and genital warts. This is usually administered a few years before a girl becomes sexually active. The usual recommended age is 9 to 11 years. The vaccine protects against the two strains of HPV responsible for more than 70% of cervical cancers in the U.K.
Cervical Cancer: Causes, Symptoms, Treatment, and HPV Prevention | Mass General Brigham
Sources
- “Cervical Cancer.” Nhs.uk, 20 Oct. 2017, www.nhs.uk/conditions/cancer-of-the-cervix/Pages/introduction.aspx?WT.mc_id=61001. www.nhs.uk/.../introduction.aspx?WT.mc_id=61001
- Centers for Disease Control and Preventions, and Inside Knowledge campaign. Inside Knowledge 2016 Cervical Cancer Factsheet. 2016. http://www.cdc.gov/cancer/cervical/pdf/cervical_facts.pdf
- World Health Organization. “Cervical Cancer.” World Health Organization, 2019, www.who.int/health-topics/cervical-cancer#tab=tab_1, https://www.who.int/health-topics/cervical-cancer#tab=tab_1
Further Reading
Last Updated: Feb 19, 2024