Cutaneous T-cell lymphomas are a group of T-cell related cancers that mainly affect the skin. There are many different treatment options available for Cutaneous T-cell lymphomas with varying degrees of success.
Skip to
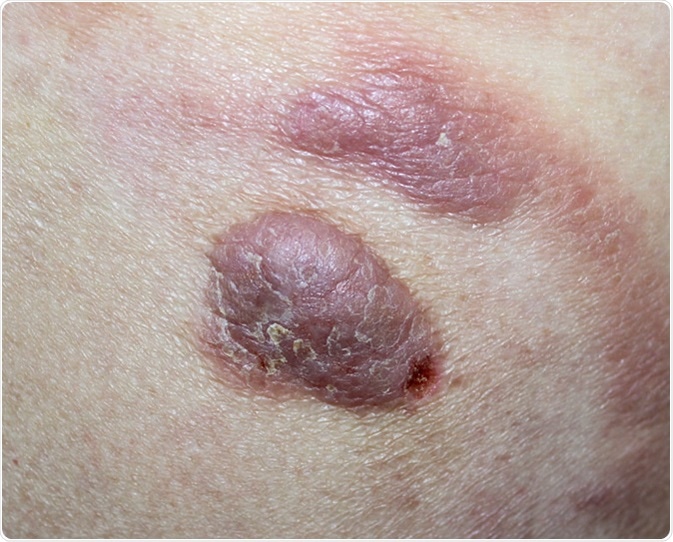
Cutaneous T-cell lymphoma. Image Credit: Dermatology11 / Shutterstock
Cutaneous T-cell lymphoma
Cutaneous T-cell lymphomas (CTCLs) are a group of T-cell proliferation that mainly affects the skin. The most common CTCLs are mycosis fungoides (MF), Sezary Syndrome (SS), and a number of CD30 positive lymphoproliferative disorders such as primary cutaneous anaplastic large cell lymphoma (pcALCL).
MF and SS have similar symptoms but can be distinguished from each other with a clinical pathology evaluation. MF is the proliferation of skin-homing T-cells and mainly occurs in patients over 60. SS is a leukemic variation of CTCL which is characterized by malignant Sezary cells (T-cell lymphoma with a CD4+ T cell phenotype) present in the blood, lymph nodes, and skin.
Mycosis Fungoides and Cutaneous Lymphomas
Pathogenesis and pathophysiology of cutaneous T-cell lymphoma
Unregulated activation and build-up of T-cells can lead to the development of CTCL. Certain human leukocyte antigen (HLA) class II alleles have been associated with CTCL development. Viral and bacterial pathogens (human t-lymphotropic virus, herpes simplex virus, Staphylococcus aureus, and Chlamydia pneumoniae) are environmental factors that can affect tumor suppressor or pro-oncogenic pathways, which can lead to the development of CTCL.
The different types of CTCL have varied developments. MF starts with scattered lymphocytic infiltrates that show as a few patches favoring the epidermis. This develops and affects more of the epidermis which results in patches, plaques, or erythroderma (widespread abnormal redness of the skin). Some patients experience the growth of lymphoid tumors which can metastasis to distant lymph nodes, bone marrow, and other organs. As MF progresses, the effectiveness of the patient’s immune system also decreases, making them far more susceptible to widespread infections. SS is also characterized by erythroderma, itching, and enlargement of lymph nodes. SS is more aggressive, and the 5-year survival rate is only 28%.
Screening and diagnosis for cutaneous T-cell lymphoma
There are many methods that can be used to diagnose CTCL. Dermoscopy is a noninvasive screening method that allows for the in vivo evaluation of microstructures of the epidermis. It is mainly used to diagnose MF. Reflectance confocal microscopy (RCM) could be used to select biopsy sites for MF, which will help reduce false negative test results. RCM can detect atypical lymphocytes in the epidermis and other cutaneous cell types. Other screening methods that can be used to evaluate CTCLs include immunohistochemistry and flow cytometry.
A definitive diagnosis of MF is challenging due to its non-specific clinical and pathologic features. The varied symptoms of MF can lead to the symptoms being diagnosed as eczema or parapsoriasis before being definitively diagnosed as MF.
The detection of Sezary cells in peripheral blood is not specific to CTCL, as Sezary cells can also be found in peripheral blood from normal donors. Histological analysis of SS gives similar findings seen with the analysis of MF but with less prominent epidermotropism (migration of T cells into the epidermis). To effectively diagnose SS the integration of clinical analysis, histologic analysis, immunophenotyping, and molecular studies are performed.
Treatments for cutaneous T-cell lymphoma
Currently, there is no cure for CTCL, so the treatment is mainly used to improve the symptoms and quality of life of a patient. Because of this, therapies are patient-specific based on age, the severity of the disease, rate of disease progression, and prior treatments. This makes it difficult to successfully treat all patients.
During the initial stages of CTCL, effective immune control can slow down the progression of the disease. Skin-specific treatment is preferred, as chemotherapy is associated with toxicity but little disease improvement.
IFN-α and IFN-γ have cytotoxic and immunological effects on tumor-associated T-cells, therefore they can be used for clinical treatments of CTCLs. With all stages of MF, IFN-α achieves better results compared to the use of chemotherapy. IFN-γ shifts the tumor supportive Th-2 dominant microenvironment to a more tumor suppressive Th-1 microenvironment.
Toll-like receptor (TLR) agonists stimulate the immune system which induces anticancer effects. The activation of TLR7 on plasmacytoid dendritic cells stimulate Th-1 immune responses, which leads to the production of IFN.
Further Reading
Last Updated: May 9, 2019