Female genital mutilation (FGM) refers to the practice of purposefully cutting, injuring, or altering female genitalia. It involves the partial or total removal of the external female genitalia. There is no medical reason to carry out female genital mutilation, and there can be serious, negative health consequences for women who experience FGM.

Image Credit: Mentari Merah Studio/Shutterstock.com
FGM may also be called female circumcision, female cutting, or as sunna, gudniin, halalays, tahur, megrez, or khitan.
Estimates state that over 200 million women and girls have been through FGM in 30 countries in Africa, Asia, and the Middle East, where the practice is most common. 3 million additional women and girls are estimated to go through female genital mutilation every year.
It is illegal in 18 countries in Africa, six states in Australia, and 17 states in the United States.
Other countries where FGM is criminalized include:
- Belgium
- Canada
- Cyprus
- Denmark
- France
- Italy
- New Zealand
- Norway
- Spain
- Sweden
- The United Kingdom.
However, making FGM illegal does not mean that it does not occur in these countries, and new cases of FGM are regularly reported worldwide, meaning FGM is a global health issue.
Why Does Female Genital Mutilation Happen?
It is usually young girls who go through female genital mutilation before puberty starts; it can be done as early as infancy through to the age of 15. However, women in their 30s can also experience FGM.
Although the FGM has no health benefits, it can be common in African countries, Asia, and the Middle East, where it is carried out by traditional circumcisers. These people can be important figures in communities, attending important events such as childbirth. However, healthcare providers also carry out FGM, operating under the belief that FGM is safer if it is done by medical professionals.
Female genital mutilation highlights the inequality between males and females and is widely seen as an act of extreme discrimination against women that violates the rights of women and children in several ways. These human rights violations include a violation of the right to health, sexual control, non-discrimination, bodily integrity, freedom and security, and, if FGM results in death, the right to life.
Several cultural beliefs support female genital mutilation, and many communities believe a woman or girl cannot get married if she has not gone through FGM. Women who have not been through FGM are sometimes thought of as promiscuous, highlighting sexual inequality between men and women in societies.
FGM is believed in some communities to promote marital and pre-marital fidelity and can be used to control a woman’s sexual freedom before marriage. Cultural ideas that support the belief that removing parts of the female genitalia posit that FGM makes a woman more feminine or preserves a woman’s modesty.
Although no religious texts require FGM, some religious leaders support FGM, and other community leaders and medical professionals can also advocate for the practice, which complicates any challenges made against FGM.
FGM can be deeply ingrained into a community and can have occurred across multiple generations of women. As a result, it can be difficult to change these cultural practices when a large number of people in a community believe in the benefits of them, and some people can be nervous about breaking these social norms for fear of discrimination.
Many organizations work to help end the harmful practice of FGM worldwide.
The Types of Female Genital Mutilation
There are four main types of female genital mutilation.
Type 1 - clitoridectomy
Type 1 FGM involves the partial or complete removal of the clitoral glans. This is the visible part of the clitoris, which is a highly sensitive part of the female genitalia located at the top of the inside of the labia majora and labia minora.
The clitoral hood, also called the prepuce, can also be removed in this type of FGM. This is the skin that surrounds the clitoral glans.
Type 2 - excision
Type 2 FGM involves the partial or complete removal of the clitoris glans and the labia minora. The labia majora can also be removed.
Type 3 - infibulation
Type 3 FGM is called infibulation. Infibulation is the practice of narrowing the opening of the vagina by creating a seal with the labia minora and labia majora. This is done by cutting the labia and stitching them to cover the vaginal opening. The clitoral glans and hood can also be removed in this procedure.
Deinfibulation is the term for the process of opening the seal covering the vaginal opening. This is often done to improve a woman’s health or to help with sexual intercourse or childbirth.
Type 4
Type 4 FGM includes all other types of female genital mutilation, covering pricking, piercing, incising, cauterizing, or scraping the female genitals.
Anesthetics are not often used during female genital mutilation, and the traumatic procedure can be carried out with knives, scissors, scalpels, glass, and razor blades. A woman will often go through FGM without her consent and may have to be restrained.
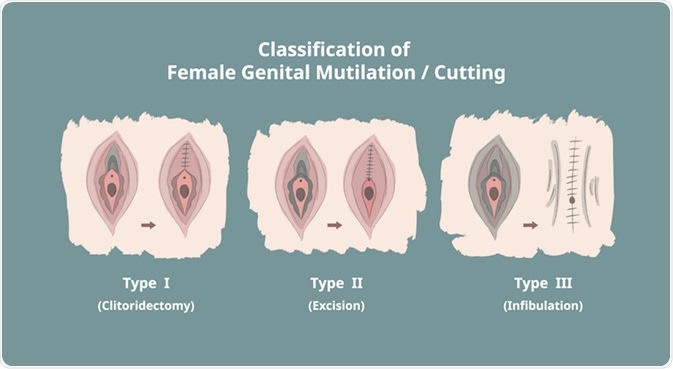
Image Credit: Fang-Chun Liu/Shutterstock.com
Risks of Female Genital Mutilation
There are no health benefits to female genital mutilation and there is no medical reason for the procedure to be carried out. There are serious risks associated with all types of female genital mutilation that include severe physical injury and trauma and long-term mental health problems.
Complications that can occur soon after FGM has been carried out include:
- Extreme pain
- Extreme bleeding (known as hemorrhage)
- Swelling of the genital tissues
- Fever
- Infections (including tetanus, gangrene, and septicemia.)
- Problems urinating
- Complications with wound healing
- Shock
- Death.
Long-term complications of female genital mutilation include:
- Problems with sexual health (including painful intercourse, lowered sexual pleasure and more)
- Problems urinating (including increased urinary tract infections, pain when urinating, and incontinence)
- Problems with the menstrual cycle (painful periods and difficulty passing period blood)
- Decreased vaginal health (discharge, itching, infections including bacterial vaginosis)
- Scarring and the development of keloid scars
- Development of cysts and abscesses
- Complications during childbirth (including prolonged and difficult deliveries, excessive bleeding, stillbirths, need for cesarean sections)
- Infertility
- Later surgeries (vaginal opening seals can be opened to allow for intercourse and childbirth and then reclosed again, increasing the risk of complications)
- Psychological problems (including depression, anxiety, post-traumatic stress disorder, and problems with self-esteem).
Girls can also be forced to leave education early because of female genital mutilation, which impacts their freedom and agency in the future.
Treatment for Female Genital Mutilation
Deinfibulation does not replace any tissue that has been lost through cutting or circumcision, but it can help with some of the problems caused by FGM. It involves reopening the seal over the vagina to help with sexual intercourse, childbirth, and any problems with urination.
This can be done under local anesthetic or general anesthetic. Deinfibulation should be done before a woman becomes pregnant if possible, and before the last two months of pregnancy, although it can be done during labor if necessary.
Summary
Female genital mutilation is a traumatic and extremely dangerous procedure that causes severe injury to a woman’s genitalia. There is no medical benefit to FGM and it is illegal in many countries, but it is widely practiced across certain countries worldwide.
There are long-term health risks for women who go through FGM, including physical injury, sexual health problems, and mental health problems.
There are female genital mutilation support clinics and child protection agencies along with other organizations that can help people who have gone through FGM or who may be at risk of FGM.
Last Updated: Aug 25, 2020