Hidradenitis supurativa, also known as acne inversa, is a chronic skin condition involving the inflammation of the apocrine sweat glands, forming pimple-like bumps known as abscesses. These tend to recur in specific regions of the body, can be very painful, and often leave behind deep scar tissue when they heal.
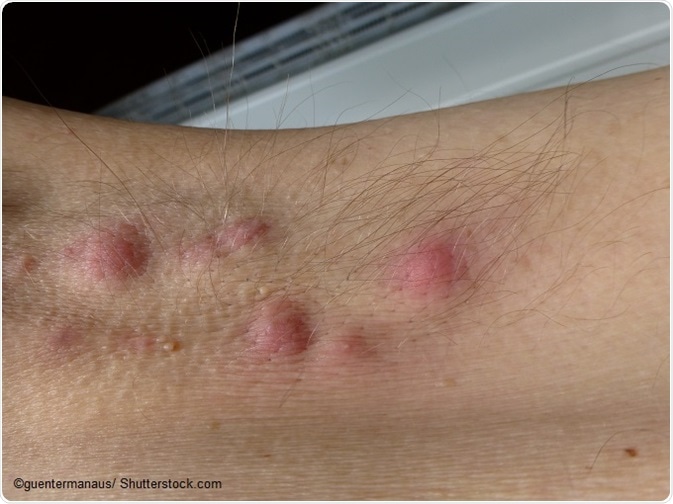
Image Credit: guentermanaus / Shutterstock.com
Cause
The cause of hidradenitis supurativa is not known, although there are several factors that are thought to be involved in the pathophysiology of the condition. These include:
- Genetics
- Hormonal imbalances
- Obesity
- Smoking
There are also some other health conditions that are linked to hidradenitis supurativa and individuals that suffer from these are more likely to be affected by the skin disease. Crohn’s disease, in particular, is associated with a higher risk and is thought to stimulate the progression of hidradenitis supurativa.
Symptoms
The hallmark sign of hidradenitis supurativa is the formation of abscesses that can be very painful and ooze pus when ruptured. These absecesses typically appear in specific areas of the body such as the groin, armpits, or underneath the breasts.
Initially, a single lesion in one region will appear, which may spontaneously resolve within 15-30 days or rupture and leak pus on their own. It is common for scar tissue to form when the lesion clears. More abscesses will likely recur in the same region and sinus tracts may form as the disease progresses, which are narrow channels of pus underneath the skin.
In some cases, bacteria can colonize the lesions and lead to an infection of the area, increasing the production of pus and symptoms of pain.
Stages of progression
Hidradenitis supurativa can be classified according to the stage of progression of the disease, as follows:
- Hurley stage 1: Single or a few lesions with no evidence of scarring or sinus tracts.
- Hurley stage 2: Recurrent abscesses in several areas of the body and initial formation of sinus tracts.
- Hurley stage 3: Many abscesses throughout the body with evidence of scarring and pus, as well as a network of sinus tracts under the skin.
These stages help to understand the severity of the condition and guide the treatment decisions to manage the symptoms.
Treatment
There are many different treatments that may be used in the management of hidradenitis supurativa with varied success. Most patients find they need to trial several options before ultimately finding the most effective solution to prevent their symptoms.
Initial treatment usually begins with simple lifestyle changes to help reduce the number of lesions and the severity of symptoms. This may include weight loss, cessation of smoking, eating well, avoiding irritants, and wearing loose-fitting clothing.
There is also a wide range of pharmaceutical options available for the treatment of hidradentis superativa, such as:
- Acne washes (e.g. benzoyl peroxide)
- Bleach baths to eradicate colonizing bacteria
- Antibiotics to manage inflammation and bacterial infections
- Hormonal therapy to regulate hormones and reduce breakouts
- Retinoid medications (e.g. acitretin) to reduce sebum secretion
- Metformin to manage patients with metabolic syndrome
- Corticosteroids (e.g. prednisolone) to relieve pain and inflammation, as well as prevent new breakouts
- Biologic medications (e.g. adalimumab) to reduce symptoms of patients with severe forms of the disease
- Methotrexate to regulate the immune system and manage symptoms
Additionally, some patients may require surgery to treat severe cases of hidradenitis supurativa. Depending on the individual circumstances, the procedure may involve laser surgery, cytotherapy, deroofing, drainage, incision or excision.
The ideal treatment is highly variable and most patients will need to trial several different options before finding the best solution to help control outbreaks and improve their quality of life.
References
Further Reading
Last Updated: Mar 3, 2021