Thyroid cancer is a type of cancer involving unregulated cell growth in the thyroid gland, located at the base of the neck. It is a rare type of cancer, accounting for approximately 1% of all people diagnosed with cancer.
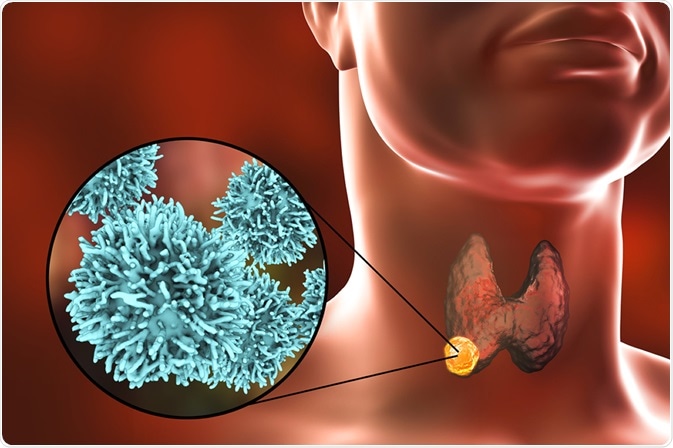
3D illustration showing thyroid gland with a tumor inside the human body and closeup view of thyroid cancer cells. Image Credit: Kateryna Kon / Shutterstock
Risk Factors
Certain populations are at an increased risk of thyroid cancer and should, therefore, be advised to check for thyroid cancer symptoms.
Risk factors include:
- Females
- Asian ethnicity
- Aged between 25 and 65
- Family history of thyroid disease
- Previous radiation treatment to head or neck
Symptoms
The most common thyroid cancer symptom is a lump or swelling in the throat, which is often painless. Any patient with a lump in the throat should be investigated for possible thyroid cancer, although only about 5% of lumps examined are found to be cancerous.
Symptoms of thyroid cancer may include:
- Lump or swelling in the throat
- Dyspnea and difficulty breathing
- Dysphagia and difficulty swallowing
- Persistent cough and hoarse voice
- Enlarged lymph nodes in the neck
Frequently Searched Questions | Thyroid Cancer
Diagnosis
The symptoms of thyroid cancer are not specific to the disease, and specific tests are required to confirm the diagnosis.
A blood sample is usually needed after a physical examination, and a thorough medical and family history has been taken. Additionally, imaging techniques are usually used to examine the thyroid gland, such as ultrasound, computed tomography (CT) scan, or magnetic resonance imaging (MRI). A laryngoscope can also be useful in the internal examination of the voice box.
A biopsy can be taken from the thyroid gland for microscopic examination in a laboratory to confirm a diagnosis.
Types
There are four primary types of thyroid cancer including:
- Papillary carcinoma usually affects young women under the age of 40 and is the most common type.
- Follicular carcinoma often affects elderly populations.
- Medullary thyroid carcinoma has hereditary characteristics and may run in families.
- Anaplastic thyroid carcinoma is the rarest and most aggressive type, usually affecting older adults over 60.
According to individual characteristics, papillary and follicular carcinoma are often treated similarly, whereas medullary and anaplastic thyroid carcinoma warrants specific management plans.
Treatment
In most thyroid cancer cases, surgical removal of the entire thyroid gland is usually the first step in the treatment plan. If the neck's lymph nodes are also suspected to be affected by cancerous cells, these are also removed surgically.
Radiation therapy plays an important role in treating thyroid cancer and may be used as the sole treatment or as adjuvant therapy following surgery. The radiation can be administered by way of an external X-ray beam aimed at the thyroid gland or by taking radioactive iodine orally.
Chemotherapy may also be used but is generally reserved as a second-line option after surgery, and radiotherapy has not been successful. This is because it is a more general treatment that carries severe side effects for the entire body, whereas surgery and radiotherapy can easily be localized to the thyroid gland.
As thyroid cancer treatment renders the function of the thyroid gland insufficient, the normal actions of the thyroid gland are interrupted post-therapy. This predominantly affects the hormones produced by the thyroid gland – triiodothyronine (T3), thyroxine (T4), and calcitonin – which need to be administered pharmacologically on a lifelong basis.
References
Further Reading
Last Updated: Jan 20, 2021