Stress is actually a bit of a buzzword. The initial definition was “the reaction to changes”, which is why you get stressed also when good things happen, hence the distinction between good stress, eustress, and bad stress, distress.
Since the 90’s, stress has become a synonym of the everyday hustling, describing a life style. We focus on the original definition, evaluating the user autonomic balance that can be estimated from heart rate variability (HRV).
Can you please outline the physiological response to stress in terms of the sympathetic and parasympathetic nervous systems?
The autonomic nervous system (the sympathetic and parasympathetic systems) has a direct influence over most of our internal organs.
The sympathetic system is called “fight or flight” because it takes over whenever you have to perform quickly, answering to a challenge. When you are under stress, the sympathetic system help you perform, the heart rate accelerates, adrenaline flows. But this also means that you are consuming your body to face a challenge.
The parasympathetic system is called “rest and digest”, and basically takes over when you are relaxed, and helps your body fortify. After a period of stress, it’s important for you to relax, so the parasympathetic system can take over and you can recover.
We usually think that stress is always bad. This is not true, stress is basically whatever happens whenever you have to adapt to a change, and the physiological reaction helps you cope with this challenge. An autonomic imbalance towards the sympathetic system becomes dangerous only if you never recover after a prolonged period of high activation. In that case stress becomes harmful, and it has shown to be correlated with dangerous conditions.
How does deep breathing work from a physiological perspective?
Luckily for us, there is a quite simple trick that has an immediate and beneficial effect on the autonomic system.
The diaphragm is linked to the vagus nerve, which interfaces with parasympathetic control of the heart rate. If you perform diaphragmatic, slow, deep breathing, you will literally pull your vagus nerve, forcing your heart rate to raise during inhalation (a momentary suspension of parasympathetic activity), and fall during exhalation (parasympathetic system kicks back in).
Slow diaphragmatic breathing has been proven to relax patients. It’s commonly used to calm down patients with panic attacks. You can find scientific papers back from the 60’s proving its efficacy, but it’s a technique that was already used in China thousands of years ago.

What effect does deep breathing have on the heart rate?
The stimulation of the vagus nerve, if done correctly by breathing using the diaphragm, will force the heart rate to raise and fall in synch with the breathing. This phenomenon is called Respiratory Sinus Arrhythmia (RSA).
However, if you breathe forcing expansion of your chest instead of your diaphragm, you won’t see anything interesting on your heart rate, nor will your autonomic activity be affected.
Babies spontaneously know how to correctly breathe (using the diaphragm). Sadly, adults tend to forget, and usually breathe forcing expansion of the chest. Chest breathing will not have the same effect on your autonomic system.
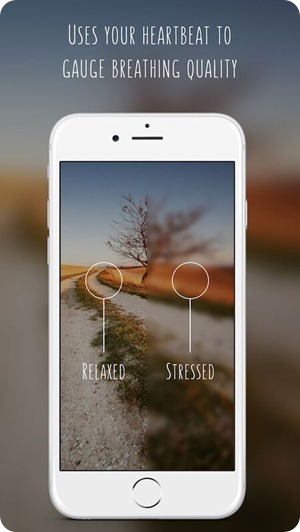
Can you please outline the app Biobeats developed to teach users to deep breathe?
We developed an app, Hear and Now (https://biobeats.com/ ), that guides the user through breathing exercises. Using music and visual cues, we teach the correct breathing pattern. In the meantime we measure the users heart rate using the smartphone camera as a PPG device, or using a connected wearable heart rate device.
Measuring the response of the users heart rate to the exercise, we give immediate feedback about the effectiveness of the exercise. This will let the user know if they performed chest or diaphragmatic breathing, and will let them track their progress over time.
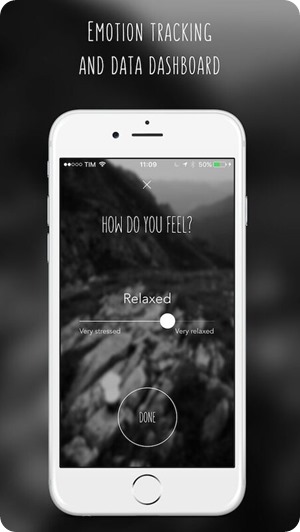
How does the app work and in what ways does it use artificial intelligence?
The app leverages on Respiratory Sinus Arrhythmia to measure the users breathing quality.
We are currently piloting a new version of the app that uses artificial intelligence to estimate the level of stress of the users, and suggests the best moment to perform a breathing exercise.
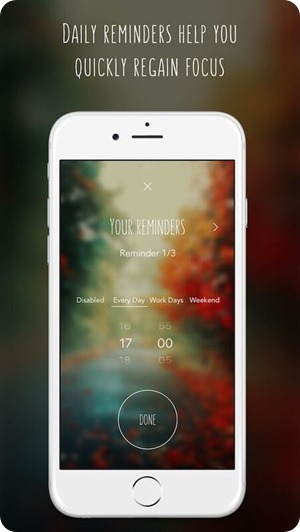
What were the main aims behind developing the ‘Hear and Now’ app?
We believe that technology can help people track their wellbeing. With wearable devices, this can happen passively. We think that the Quantified Self movement should progress from giving data about physical activity back to users, to giving insights about what causes stress, and a concrete help in managing stress.
How do you plan to use the data from the app?
We are training our stress detection algorithms using the data we collect from internal pilots. Once the algorithms are ready, we will apply the same technology to the B2C market, and offer stress coaching programs to users.
What does the future hold for Biobeats?
We are currently building stress reduction programs for medium to large sized corporate clients and will be launching a B2C product with breathing and stress coaching programs.
How important do you think artificial intelligence will be in combating medical issues such as stress going forwards?
At the moment, we are focusing on wellbeing, trying to help people detect stress before they burn out. However, the same Artificial Intelligence approach could be used to detect the onset of conditions, and implement early interventions.
After years of stagnation, deep learning has shown how effective it can be in solving tasks that can’t be easily solved by traditional computer science. However, it’s a young discipline, and there is still much to be done, and the intersection with the medical field is still largely to be explored.
Where can readers find more information?
The effectiveness of breathing techniques has been largely explored and many interesting scientific papers can be found on Google Scholar. The “Benson Relaxation Response” is certainly a good starting point.
About breathing and asthma:
- Holloway, Elizabeth A., and Robert J. West. “Integrated Breathing and Relaxation Training (the Papworth Method) for Adults with Asthma in Primary Care: A Randomized Controlled Trial.” Thorax 62, no. 12 (2007): 1039–42.
- Holloway, E., and F. S. Ram. “Breathing Exercises for Asthma.” Cochrane Database Syst Rev 1 (2004). http://onlinelibrary.wiley.com/doi/10.1002/14651858.CD001277.pub2/pdf/.
- Opat, A. J., M. M. Cohen, M. J. Bailey, and M. J. Abramson. “A Clinical Trial of the Buteyko Breathing Technique in Asthma as Taught by a Video.” Journal of Asthma 37, no. 7 (2000): 557–64.
- Thomas, M., R. K. McKinley, E. Freeman, C. Foy, P. Prodger, and D. Price. “Breathing Retraining for Dysfunctional Breathing in Asthma: A Randomized Controlled Trial.” Thorax 58, no. 2 (2003): 110–15.
- About breathing and hypertension:
- Brook, Robert D., Lawrence J. Appel, Melvyn Rubenfire, Gbenga Ogedegbe, John D. Bisognano, William J. Elliott, Flavio D. Fuchs, et al. “Beyond Medications and Diet: Alternative Approaches to Lowering Blood Pressure a Scientific Statement from the American Heart Association.” Hypertension 61, no. 6 (2013): 1360–83.
- Grossman, E., A. Grossman, M. H. Schein, R. Zimlichman, and B. Gavish. “Breathing-Control Lowers Blood Pressure.” Journal of Human Hypertension 15, no. 4 (2001): 263–69.
- Holloway, Elizabeth A., and Robert J. West. “Integrated Breathing and Relaxation Training (the Papworth Method) for Adults with Asthma in Primary Care: A Randomised Controlled Trial.” Thorax 62, no. 12 (2007): 1039–42.
- Joseph, Chacko N., Cesare Porta, Gaia Casucci, Nadia Casiraghi, Mara Maffeis, Marco Rossi, and Luciano Bernardi. “Slow Breathing Improves Arterial Baroreflex Sensitivity and Decreases Blood Pressure in Essential Hypertension.” Hypertension 46, no. 4 (2005): 714–18.
- Schein, M. H., B. Gavish, M. Herz, D. Rosner-Kahana, P. Naveh, B. Knishkowy, E. Zlotnikov, N. Ben-Zvi, and R. N. Melmed. “Treating Hypertension with a Device That Slows and Regularises Breathing: A Randomised, Double-Blind Controlled Study.” Journal of Human Hypertension 15, no. 4 (2001): 271–78.
- Viskoper, Reuven, Irena Shapira, Rita Priluck, Rina Mindlin, Larissa Chornia, Anny Laszt, Dror Dicker, Benjamin Gavish, and Ariela Alter. “Nonpharmacologic Treatment of Resistant Hypertensives by Device-Guided Slow Breathing Exercises*.” American Journal of Hypertension 16, no. 6 (2003): 484–87.
About the relationship between stress and heart rate variability:
- Boonnithi, Sansanee, and Sukanya Phongsuphap. “Comparison of Heart Rate Variability Measures for Mental Stress Detection.” In Computing in Cardiology, 2011, 85–88. IEEE, 2011. http://ieeexplore.ieee.org/xpls/abs_all.jsp?arnumber=6164508.
- Hughes, Joel W., and Catherine M. Stoney. “Depressed Mood Is Related to High-Frequency Heart Rate Variability during Stressors.” Psychosomatic Medicine 62, no. 6 (2000): 796–803.
- Kim, Desok, Yunhwan Seo, Sook-hyun Kim, and Suntae Jung. “Short Term Analysis of Long Term Patterns of Heart Rate Variability in Subjects under Mental Stress.” In BioMedical Engineering and Informatics, 2008. BMEI 2008. International Conference on, 2:487–91. IEEE, 2008. http://ieeexplore.ieee.org/xpls/abs_all.jsp?arnumber=4549221.
- Melillo, Paolo, Marcello Bracale, Leandro Pecchia, and others. “Nonlinear Heart Rate Variability Features for Real-Life Stress Detection. Case Study: Students under Stress due to University Examination.” Biomed Eng Online 10, no. 1 (2011): 96.
- Mezzacappa, Elizabeth Sibolboro, Robert M. Kelsey, Edward S. Katkin, and Richard P. Sloan. “Vagal Rebound and Recovery from Psychological Stress.” Psychosomatic Medicine 63, no. 4 (2001): 650–57.
- Orsila, Reetta, Matti Virtanen, Tiina Luukkaala, Mika Tarvainen, Pasi Karjalainen, Jari Viik, Minna Savinainen, and Clas-H\a akan Nyg\a ard. “Perceived Mental Stress and Reactions in Heart Rate Variability—a Pilot Study among Employees of an Electronics Company.” International Journal of Occupational Safety and Ergonomics 14, no. 3 (2008): 275–83.
- Pecchia, Leandro, Paolo Melillo, and Marcello Bracale. “Remote Health Monitoring of Heart Failure with Data Mining via CART Method on HRV Features.” Biomedical Engineering, IEEE Transactions on 58, no. 3 (2011): 800–804.
- Salahuddin, Lizawati, Jaegeol Cho, Myeong Gi Jeong, and Desok Kim. “Ultra Short Term Analysis of Heart Rate Variability for Monitoring Mental Stress in Mobile Settings.” In Engineering in Medicine and Biology Society, 2007. EMBS 2007. 29th Annual International Conference of the IEEE, 4656–59. IEEE, 2007. http://ieeexplore.ieee.org/xpls/abs_all.jsp?arnumber=4353378.
- Schlotz, Wolff, Ilona S. Yim, Peggy M. Zoccola, Lars Jansen, and Peter Schulz. “The Perceived Stress Reactivity Scale: Measurement Invariance, Stability, and Validity in Three Countries.” Psychological Assessment 23, no. 1 (2011): 80.
- Stalder, Tobias, Phil Evans, Frank Hucklebridge, and Angela Clow. “Associations between the Cortisol Awakening Response and Heart Rate Variability.” Psychoneuroendocrinology 36, no. 4 (2011): 454–62.
About Davide Morelli
Researcher and entrepreneur, I lead BioBeats’ engineering team. I am a specialist in the intersection between Artificial Intelligence and music, I previously ran a successful distributed software consultancy (Parser) for ten years.
I am also an active composer, and my PhD in Computer Science focuses on energy models for algorithms that illuminate correlations.