Developing novel medications has many challenges: evading the immune system, minimizing the danger of cytotoxicity, and obtaining FDA approval. Overcoming these issues requires proven developmental and analytical approaches, procedures to avoid patient harm, and techniques to increase blood circulation time.
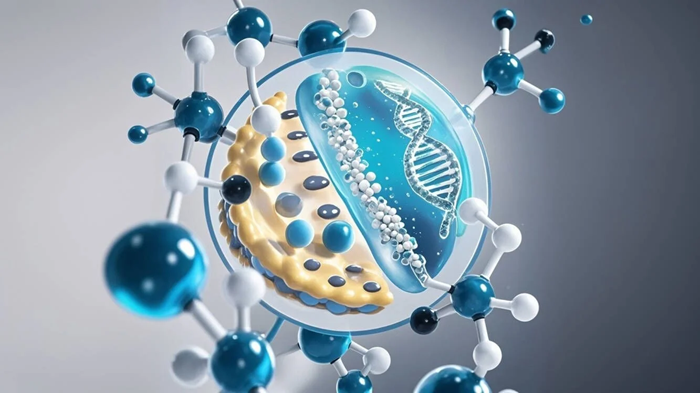
Image Credit: Genizer
Encapsulating an active substance in a liposome or lipid nanoparticle can minimize cytotoxicity and increase blood circulation by bypassing the immune system.
Several techniques can improve a drug's efficacy, including increased permeability and retention, targeted external stimuli, and active targeting. These strategies function by focusing on a certain location. Liposomes have been approved and used as medications for decades in Europe and the United States.
Liposomes and lipid nanoparticles were the first nanomedicines, and they remain significant today. The use of liposomes in clinical trials has risen in recent years; for example, the crucial Moderna mRNA COVID-19 vaccine is a lipid nanoparticle.1,2
Image Credit: Genizer
Liposomes
Human cell membranes are composed of phospholipid bilayers. These membranes have hydrophilic ends on the inside and outside, and hydrophobic tails in the center.3
The phospholipid bilayer is semipermeable. The hydrophilic core prevents the entry of hydrophobic molecules into the cell, though some hydrophilic molecules can still pass through it.4

Image Credit: Genizer
Liposomes are synthetic cell membranes made of cholesterol and phospholipids. They are used in a variety of applications, including pharmaceuticals, agriculture, and cosmetics.3 Liposomes are biodegradable and inert, much like human cell membranes.5
The combination of hydrophilic and hydrophobic sections can cause spherical liposomes to form naturally: the hydrophilic ends attract each other, as do the hydrophobic heads.5,6 Researchers can also resize the generated liposomes to meet their specifications.
Liposomes can range in size from 0.025–2.5 μm, but biomedical researchers typically use liposomes sized 50–450 nm.7 The characteristics of liposomes vary depending on their formulation, making them incredibly adaptable.3
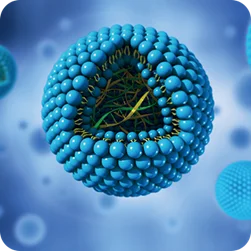
Image Credit: Genizer
Liposomes were one of the first types of lipid nanoparticles,8 and researchers are still working on developing the next generation, including solid lipid nanoparticles such as cationic lipid-nucleic acid complexes, which are currently used in the delivery of nucleic acid therapeutics. These complexes enhance drug delivery by reducing degradation.8
Reduced cytotoxicity is one of the key advantages of encapsulating an active substance in a liposome or other lipid nanoparticle.
Biocompatibility
Cytotoxicity harms patient cells, which in turn exacerbates any side effects and limits patient compliance. Encapsulating active ingredients in liposomes can reduce cytotoxicity while increasing active ingredient efficacy.
Cancer drugs can be exceedingly cytotoxic, making it critical to limit cytotoxicity in cancer treatments.9 Cytarabine, for example, is an anti-tumor medication with a short bioavailability and blood circulation period.
Severe side effects have been associated with the drug's standalone use, forcing Depocyt® to combine DepoFoam and liposome technology to reduce the required injection frequency while enhancing patient compliance.9
Amphotericin B, an antibiotic used to treat fungal infections, is also cytotoxic. When administered alone, Amphotericin B has low absorption and can impair renal function.
Amphotericin B was more effectively absorbed by macrophages when it was encapsulated in a liposome. The macrophages delivered the liposomes to the infection site, where they gradually released Amphotericin B. Removing the liposomes from the plasma improved absorption while reducing adverse effects.
Versatility
Liposomes can carry a variety of active substances, including enzymes, vaccines, and medicines.10 Liposomes' phospholipid structure enables them to transport hydrophilic and hydrophobic nanoparticles. Hydrophilic components are integrated into the hydrophobic tails, and hydrophobic components are kept in the liposome's center.5,11
Liposomes are nanocarriers with customizable properties, including their size. Researchers can use sonication, extrusion, and homogenization to alter liposome size. Larger particles require larger liposomes, but smaller liposomes can better elude the immune system.8
Nanomedicine performance can be improved by adjusting lipid content, using nanoparticle liposome hybrids, and making surface alterations.3,11 For example, cholesterol is a key component of phospholipid bilayers and can influence permeability.5
Liposome characteristics can be altered by adjusting formulation parameters such as cholesterol content. The phosphates in the liposome can have a negative, positive, or neutral charge, which affects cytotoxicity and drug delivery.2
Liposomes can also be customized to control the rate of release of the active ingredient; for example, by adding more lipid bilayers to slow it down.12
Stealth liposome technology involves attaching polymers to liposomes to better protect them from the immune system. The most commonly used polymer is polyethylene glycol (PEG), which is frequently used in pharmacology to prolong the circulation time of an active substance by minimizing the risk of liposome fusion. This approach improves the distribution of the active substance.2,9,11
The liposome nanomedicine Doxil® contains doxorubicin. PEG is attached to the liposomes in this medicine, improving its anti-tumor activity while allowing it to remain in the body longer. This gives the drug more time to reach its destination.
PEG alterations are an effective technique, but they have some limits. Patients taking large doses of medications such as Doxil®, for example, may develop skin problems not associated with non-PEG liposome nanomedicine.2
Specificity
A key advantage of liposome nanocarriers is their ability to target disease. They can also be beneficial in imaging applications such as ultrasounds and MRIs.11
The enhanced permeability and retention (EPR) effect is a widely used passive targeting approach for cancer nanomedicines. Tumors have increased permeability due to abnormal blood vessels that create holes in capillaries. As a result, tumors have limited fluid circulation and accumulate macromolecules.
Macromolecules, such as liposomes, accumulate more in tumor tissue than in non-tumor tissue, but a variety of challenges, including limited understanding of tumor microenvironments, impede the successful use of EPR in nanomedicine.13 As a result, EPR alone is often insufficient for proper targeting.1
Using external stimuli is another common targeting method. For example, thermosensitive liposomes can be used with radiofrequency ablation to raise the temperature in the target area.9 Liposomes have also been created to use sound as a targeting mechanism, making them suitable for use in ultrasound contrast agents.8
External stimuli can also be used to alter medication release time,8 with pH- and temperature-sensitive liposomes showing promise for use in phase transitions to control drug delivery time.10
Some molecules can bind to liposomes and actively target liposome nanomedicines. Such molecules, known as ligands, may contain proteins, antibodies, or sugars.13 Combining EPR and actively targeted liposomes can boost medication efficacy.
Proven
Liposomal drugs have been FDA- and European Medicines Agency (EMA)-approved for decades.2,14 For example, in 1990, the FDA approved AmBisome for the treatment of fungal infections.2
Liposome pharmaceuticals are licensed for several uses, including vaccinations, cancer therapy, anesthesia, pain management, and the treatment of age-related macular degeneration.2,14
Doxorubicin liposomes are a well-studied example. Despite its extensive usage in cancer treatments, doxorubicin is extremely cytotoxic when used on its own. Encapsulating it in a liposome decreases toxicity, facilitating the safe delivery of larger therapeutic doses.
Doxil®, the doxorubicin liposome nanomedicine, was approved by the FDA in 1995 and the EMA as Caelyx® in 1996 before being listed in China in 2003.2
Liposomes have been proven useful and safe for a variety of medications, but their safety is continually reassessed as researchers investigate new possibilities.
This is particularly beneficial as lipid nanoparticles incorporate new components. Liposome nanomedicines can also benefit from important qualities that have already been defined for approval,1 such as the Moderna mRNA vaccine, which the FDA authorized in 2021.2
Future
Future researchers face a hurdle in administering lipid nanoparticles. Most FDA-approved liposome medications are administered intravenously or intrathecally. However, Arikayce®, a drug inhaled to treat the lung illness caused by Mycobacterium avium complex, illustrates the potential for alternative delivery methods.15
Continued challenges in lipid nanoparticle medicine offer opportunities for researchers to investigate and improve. One major problem is the effective targeting of nanomedicines, as current liposome nanomedicines rely on the EPR effect for active targeting.
Researchers could explore ligand attachments and environmental cues to better target nanomedicines.1 A nanomedicine must be near the target location in order to be effective, which is a significant difficulty in present research.
If the nanomedicine moves too quickly through the bloodstream, the ligand will not reach its location, rendering the targeting mechanism ineffective.13 More research is needed to improve blood circulation and create targeting approaches to increase effectiveness while reducing cytotoxicity.
Lipid nanoparticles could also be tailored to individual patients’ needs as part of a personalized therapeutic approach. Personalized medicine recognizes each patient's unique characteristics and seeks to account for them throughout therapy.
Nanomedicines’ ability to better target specific illnesses or locations may allow patients to receive higher doses tailored to their condition, opening new possibilities in diagnostics.
Personalized treatment also requires consideration of the precise tumor microenvironment when treating cancer, addressing a fundamental challenge in nanomedicine targeting. For example, a specific receptor could be added to a liposome to target a patient's disease-presenting location.16
Combining individual diagnostics and treatment provides an additional chance to tailor liposomes. The same liposome might be used for both imaging and drug administration, allowing clinicians to know when to discontinue a certain treatment.1
Lipid nanoparticles can transport active proteins and gene therapies, reducing the risk of denaturation and facilitating easier cell delivery.2 Researchers face additional hurdles in such cases, since the nanoparticles could be more harmful than a liposome.8
The future holds great promise for personalizing, enhancing, and adapting liposomal nanomedicines to meet these problems. The appropriate combination of bioavailability, adaptability, specificity, and demonstrated success will be critical to reaching this vision.
References and further reading
- Giordani, S., et al. (2023). Liposomes characterization for market approval as pharmaceutical products: Analytical methods, guidelines and standardized protocols. Journal of Pharmaceutical and Biomedical Analysis, 236, pp.115751–115751. DOI: 10.1016/j.jpba.2023.115751. https://www.sciencedirect.com/science/article/pii/S0731708523005204?via%3Dihub.
- He, Y., et al. (2022). Liposomes and liposome-like nanoparticles: From anti-fungal infection to the COVID-19 pandemic treatment. Asian Journal of Pharmaceutical Sciences, (online) 17(6), pp.817–837. DOI: 10.1016/j.ajps.2022.11.002. https://www.sciencedirect.com/science/article/pii/S1818087622001040?via%3Dihub.
- Akbarzadeh, A., et al. (2013). Liposome: classification, preparation, and applications. Nanoscale Research Letters, (online) 8(1). DOI: 10.1186/1556-276x-8-102. https://link.springer.com/article/10.1186/1556-276X-8-102.
- Nasr, G., et al. (2020). Liposomal membrane permeability assessment by fluorescence techniques: Main permeabilizing agents, applications and challenges. International Journal of Pharmaceutics, 580, p.119198. DOI: 10.1016/j.ijpharm.2020.119198. https://www.sciencedirect.com/science/article/abs/pii/S0378517320301824?via%3Dihub.
- Cuffari, B. (2010). What is a Liposome? (online) News-Medical.net. Available at: https://www.news-medical.net/life-sciences/What-is-a-Liposome.aspx.
- Deamer, D.W. (2010). From ‘Banghasomes’ to liposomes: A memoir of Alec Bangham, 1921–2010. The FASEB Journal, 24(5), pp.1308–1310. DOI: 10.1096/fj.10-0503. https://faseb.onlinelibrary.wiley.com/doi/10.1096/fj.10-0503.
- Sharma, P., et al. (2023). Introductory Chapter: Liposome - A Versatile Tool for Drug Delivery in Nanobiomedicine. IntechOpen eBooks. DOI: 10.5772/intechopen.109426. https://www.intechopen.com/chapters/85407.
- Tenchov, R., et al. (2021). Lipid Nanoparticles - From Liposomes to mRNA Vaccine Delivery, a Landscape of Research Diversity and Advancement. ACS Nano, (online) 15(11). DOI: 10.1021/acsnano.1c04996. https://pubs.acs.org/doi/10.1021/acsnano.1c04996.
- Bulbake, U., et al. (2017). Liposomal Formulations in Clinical Use: An Updated Review. Pharmaceutics, (online) 9(4), p.12. DOI: 10.3390/pharmaceutics9020012. https://www.mdpi.com/1999-4923/9/2/12.
- Pande, S. (2023). Liposomes for drug delivery: review of vesicular composition, factors affecting drug release and drug loading in liposomes. Artificial Cells Nanomedicine and Biotechnology, 51(1), pp.428–440. DOI: 10.1080/21691401.2023.2247036. https://www.tandfonline.com/doi/full/10.1080/21691401.2023.2247036.
- Xing, H., Hwang, K. and Lu, Y. (2016). Recent Developments of Liposomes as Nanocarriers for Theranostic Applications. Theranostics, (online) 6(9), pp.1336–1352. DOI: 10.7150/thno.15464. https://www.thno.org/v06p1336.htm.
- Yamauchi, M., et al. (2007). Release of drugs from liposomes varies with particle size. Biological & Pharmaceutical Bulletin, (online) 30(5), pp.963–966. DOI: 10.1248/bpb.30.963. https://www.jstage.jst.go.jp/article/bpb/30/5/30_5_963/_article.
- Bertrand, N., et al. (2014). Cancer nanotechnology: The impact of passive and active targeting in the era of modern cancer biology. Advanced Drug Delivery Reviews, 66, pp.2–25. DOI: 10.1016/j.addr.2013.11.009. https://www.sciencedirect.com/science/article/abs/pii/S0169409X13002688?via%3Dihub.
- Giordani, S., et al. (2023). Liposomes characterization for market approval as pharmaceutical products: Analytical methods, guidelines and standardized protocols. Journal of Pharmaceutical and Biomedical Analysis, 236, pp.115751–115751. DOI: 10.1016/j.jpba.2023.115751. https://www.sciencedirect.com/science/article/pii/S0731708523005204?via%3Dihub.
- Giordani, S., et al. (2023). Liposomes characterization for market approval as pharmaceutical products: Analytical methods, guidelines and standardized protocols. Journal of Pharmaceutical and Biomedical Analysis, 236, pp.115751–115751. DOI: 10.1016/j.jpba.2023.115751. https://www.sciencedirect.com/science/article/pii/S0731708523005204?via%3Dihub.
- Alghamdi, M.A., et al. (2022). The Promise of Nanotechnology in Personalized Medicine. Journal of Personalized Medicine, 12(5), p.673. DOI: 10.3390/jpm12050673. https://www.mdpi.com/2075-4426/12/5/673.
Acknowledgments
Produced from materials originally authored by Kristi Hetchler from Genizer.
About Genizer
Genizer™, located in Technology Link in Greater Los Angeles, is dedicated to advancing homogenizer nanotechnology.
The company provides high-pressure homogenizers, liposome extruders, sanitary heat exchangers, diamond interaction chambers, and high-pressure gauges compatible with other brands of high-pressure homogenizers, pumps, and microfluidizers.
Sponsored Content Policy: News-Medical.net publishes articles and related content that may be derived from sources where we have existing commercial relationships, provided such content adds value to the core editorial ethos of News-Medical.net, which is to educate and inform site visitors interested in medical research, science, medical devices, and treatments.