Granuloma inguinale (also known as donovanosis) is a sexually-transmitted clinical entity that presents with readily bleeding genital ulcerations. This condition is encountered in diverse regions of the world, most of which have scanty medical research capabilities.
The causative microorganism is generally reported as Calymmatobacterium granulomatis, which is a Gram-negative, encapsulated pleomorphic bacterial pathogen. However, due to close phylogenetic resemblance with certain representatives of the genus Klebsiella, in recent years the organism was reclassified as Klebsiella granulomatis comb. nov.
A Variety of Clinical Forms
After an average incubation period of 17 days, this condition starts to become clinically apparent. Although the initial sign of infection is usually a firm papule or a nodule under skin that has the propensity to ulcerate, there are four principal types of granuloma inguinale:
- Ulcerograulomatous type – the most common type of disease that is characterized by single or multiple fleshy, non-tender, exuberant ulcers which may bleed upon touching
- Verrucous (or hypertrophic) type – in this type the ulcer is characterized raised, irregular edges, often presenting with a dry, walnut-like appearance
- Necrotic type – the ulcer is deep and foul-smelling with concomitant tissue destruction
- Sclerotic (or cicatricial) type – substantial formation of fibrous and scar tissue is seen in this type, but histopathological examination is warranted for disease confirmation
The main predilection spot are genitals which are involved in 90% of all cases, while the inguinal region is affected in 10% of cases. In women, the labia minora and the posterior margin of the vulva are most often affected; in men, usual sites of infection are prepuce, frenulum, coronal sulcus and glans penis (hence uncircumcised men are at greater risk of acquiring this condition).
Extragenital lesions are observed in 6% of cases and may present on the lips, cheeks, nose, neck, throat and chest. They are usually linked to primary genital disease, thus in primary extragenital lesions one should always consider a possibility of rhinoscleroma (a chronic, granulomatous infection of the nose caused by a similar pathogen).
Donovanosis does not involve lymph nodes, which is a feature that discriminates this condition from chancroid and lymphogranuloma venereum. Disseminated form of the disease is quite rare, albeit secondary spread to bone and liver may occur (usually in association with pregnancy).
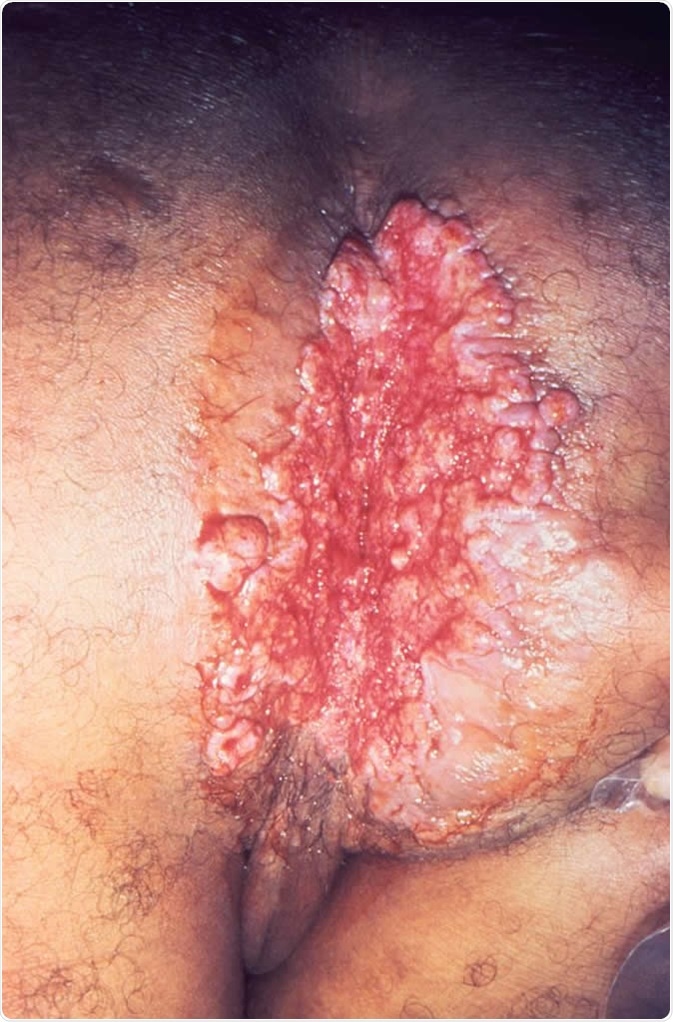
A very large erosive cutaneous lesion in the perineal region of this patient, which had been diagnosed as Donovanosis, otherwise known as granuloma inguinale, a genital ulcerative disease caused by the Gram-negative bacterium, Klebsiella granulomatis, formerly known as Calymmatobacterium granulomatis, and even earlier Donovania granulomatis. The causative organism is difficult to culture, and diagnosis requires visualization of dark-staining Donovan bodies on tissue crush preparation from a biopsy. Image Credit: CDC/ Joe Miller
Complications and Consequences
The most frequent complication in modern era is pseudoelephantiasis (in up to 5% of all the affected individuals), which is more commonly observed in women. In the cicatricial type of donovanosis there is a possibility of urethral, vaginal or anal stenosis.
Luckily, carcinomas are rarely reported nowadays, but they are still a dreaded complication of this condition. One study found cancer as a sequel of donovanosis in only 0.25% of positive cases, while a study from Jamaica found that Klebsiella granulomatis comb. nov. antigens were reactive in 14.5% of penile carcinoma.
Ulcers in granuloma inguinale can be co-infected with other sexually-transmitted diseases – most notably syphilis. Such cases should be managed by employing a ‘syndromic approach’ (i.e. clinical decision-making based on symptoms and signs, and not primarily on precise diagnosis).
Also, donovanosis increases the risk of HIV infection, which results in protracted lesion presence. Furthermore, HIV-positive individuals experience increased tissue damage and require more time for scars to develop. There is also a report of co-existent squamous cell carcinoma in HIV-positive patient.
Further Reading
Last Updated: Jan 25, 2019