If pericarditis persists for more than three months, then it is called chronic pericarditis. Constrictive pericarditis (CP) (hardness of the pericardium tissue through scarring) and chronic effusive pericarditis (CEP) (accumulation of excessive fluid in the space inside the pericardium - pericardial cavity) are the two major complications of chronic pericarditis.
 Image Credit: BlurryMe/Shutterstock.com
Image Credit: BlurryMe/Shutterstock.com
Chronic effusive pericarditis
It is difficult to exactly measure the span of chronic effusive pericarditis spread since the symptoms are not clear in most cases; however, some of the symptoms are chest pain, lightheadedness, hiccups, and shortness of breath. A research carried out among 20 people, especially older adults, has concluded that they have some degrees of fluid build-up in their pericardium. Similar to symptoms, the exact causes for this condition also remain unknown; however, the possible causes of CEP are:
- Hepatitis or tuberculosis
- Spread of cancer from other parts of the body to the pericardium
- Injury or damage which occurs during surgery
Chronic effusive pericarditis can be treated using medications or surgical techniques. The medication tried initially to treat this disease is non-steroidal anti-inflammatory drugs (NSAIDs). When it does not help, the physician will recommend surgery. The most frequent surgical method used for treating this disease is pericardiocentesis.
In this surgery, a catheter (thin plastic tube) is passed into the pericardium via the chest, and the excessive fluid in the pericardium is drained out. Before passing the catheter, the patient is given a local anesthetic to desensitize the skin, so that they would not experience any pain during the surgery.
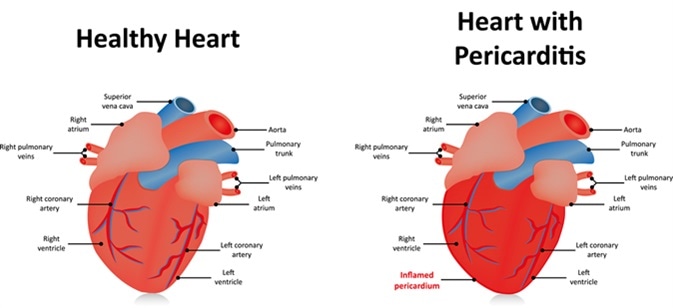
Pericarditis. Image Credit: Joshya/Shutterstock.com
Constrictive pericarditis
It is an uncommon disease, which develops over a period of time. Patients with pericarditis, especially those with long-term inflammation, can expect to develop scarring, elasticity, and contraction of the pericardium. The scarred tissue tightens the heart and obstructs the proper functioning of the heart. This condition is known as constrictive pericarditis (CP).
The common symptoms of constrictive pericarditis are:
- Swelling in the legs and abdomen
- Shortness of breath
- Nausea and vomiting
- Fatigue
- Abdominal pain
In a survey of 10 people with a history of acute pericarditis, it was reported that only one person among them developed constrictive pericarditis. The inducing factors or causes of CP are bacterial infections and complications of radiotherapy.
Constrictive pericarditis can be treated by removing the pericardium through surgery, since it may not respond well to medications; however, this type of surgery carries a higher risk (1 of 20) of death. Due to this, it is performed only if the symptoms of the patient have noteworthy side effects on the quality of life.
Other complications
Cardiac tamponade
If too much fluid collects in the pericardium, then it leads to a deadly condition called cardiac tamponade (CT). This excessive fluid creates pressure around the heart and mitigates the proper filling of blood in the heart, thus creating a drastic drop in blood pressure.
This is a definite complication in all cases of pericarditis, which is generally caused by cancer or tuberculosis. The drop in blood pressure can cause blurred vision, nausea, confusion, and weakness. These indications can establish CT rapidly, and sometimes, even within a minute.
Since it is a life-threatening condition, it requires immediate treatment. Pericardiocentesis is normally used to treat CT. If left untreated, it can be fatal. It occurs in very few cases.
Bacterial complications
Bacteria also play a vital role in complicating pericarditis. In many cases of bacterial pericarditis, the infection is triggered from any of the body parts. For instance, a patient with tuberculosis (infection in the lungs) is prone to bacterial pericarditis if the pericardium is directly accessed by the bacteria or through the bloodstream. Sometimes, these infections build up pus in the heart or pericardium, which is called an abscess.
Chronic heart failure
Another expected serious condition is myopericarditis, which is caused by an inflammation in the myocardium or damage to the cardiac tissue due to a heart attack. It is also called post-myocardial infarction (MI) pericarditis or post-heart attack pericarditis.
Sudden death is a serious complication of this condition, whereas chronic heart failure comes as a long-term complication.
Recurrent Pericarditis
The most problematic complication of acute pericarditis is recurrent or relapsing pericarditis. A pericardial pain recurs when a pericarditis patient shows a relapse of the condition after disruption of the treatment or after recovery from an initial attack. There are two types of recurrent pericarditis, namely, the incessant type and the intermittent type.
Early diagnosis and treatment of any disease, for instance, pericarditis, normally mitigate the risk of long-term complications.
Pericarditis and pericardial effusions - causes, symptoms, diagnosis, treatment, pathology
References
Further Reading
Last Updated: Dec 9, 2022