Cutaneous larva migrans is caused by the epidermal migration of the filariform larvae of various hookworm and occasionally, dog tapeworm, species. The most common type is due to the dog/cat hookworm Ancylostoma braziliense. It manifests as a red or vesicular lesion at the site of entry of the larva, usually between the toes of the bare foot. The skin around this papule is usually pruritic.
Symptoms of severe itching start immediately after infestation, and are associated with the appearance of an advancing reddish, serpiginous rash.
This lesion is usually benign, and lasts for weeks to months. Eventually the larvae, having entered an accidental host, die because they are unable to complete their life cycle. The symptoms come to a stop with the decomposition of the larval bodies.
In some patients, especially with a high larval load, the larvae may miss their way and end up in the lungs. As they penetrate the lung alveoli, they may cause pneumonitis, which is called Loeffler’s syndrome.
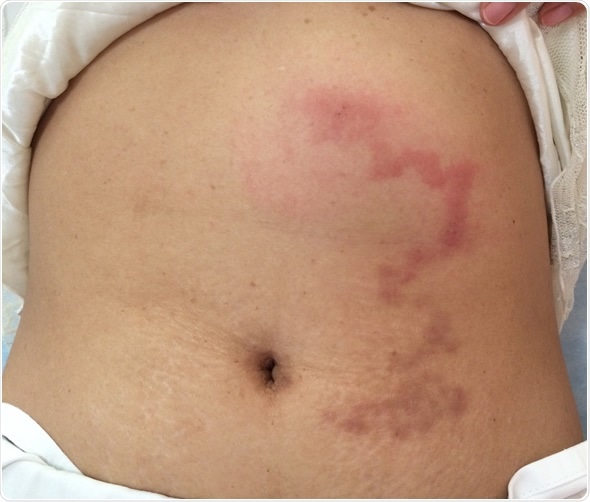
Cutaneous larva migrans at abdominal wall. Image Credit: TisforThan / Shutterstock
Diagnosis
The diagnosis of cutaneous larva migrans is essentially a clinical one. The appearance of the rash is characteristic. It is 2 – 3 mm wide, linear or tortuous, erythematous, and often vesicular, as well as intensely pruritic. This raised tortuous track moves at the rate of 1mm – 2 cm a day. The speed may vary, however, with the species.
The presence of such rashes, along with a history of having been potentially exposed to helminth larva infestation by traveling barefoot in a tropical zone, is diagnostic. The feet and the buttocks are the most commonly affected areas. Other sites include the web spaces between the toes, the anogenital regions, hands and abdomen.
Laboratory tests are used only to confirm the diagnosis in atypical cases. Skin biopsy is not recommended, because it may provoke further inflammation in these areas and does not consistently show the presence of the parasitic larvae. Microscopy may be done to show the presence of hookworm eggs or larvae in the feces.
Management
The larvae enter an accidental host with human infection and cannot penetrate the epithelial basement membrane. As a result they die within weeks or months, and the symptoms vanish. However, the severe itching for several weeks or months may be intolerable. It can lead to scratching with the risk of secondary skin infection. Also, there is a risk of complications, such as impetigo, hyper-eosinophilia and allergic reactions to the presence of the larvae.
Treatment of cutaneous larva migrans may be done with 10 – 15% thiabendazole ointment or solution topically three times a day for 15 days. Within 48 hours the itching stops and the rash ceases to advance. The treatment is difficult if there are multiple rashes or hookworm infestation of the skin follicles.
Oral thiabendazole is less effective than oral albendazole, having a cure rate of 68 – 84%. Albendazole 400 mg may be used as a single dose or repeated for two days, and produces a cure in 46 – 100%.
Another option is ivermectin, which is used off-label for this purpose, a single oral dose of 12 mg being effective in 81 – 100%. Moreover, the relapse rate is very low with this drug.
Antibacterial or antibiotic ointments are used to treat secondary infections of the inflamed skin.
Former treatment options included freezing the leading edge of the rash using cryotherapy. However, since the larva is some distance beyond the frozen part, this is usually unsuccessful. It is also painful, producing ulceration and blister formation in some patients.
References
Further Reading
Last Updated: Feb 26, 2019