Eczema is a skin disorder which results in extreme dryness and itching. Also known as Atopic Dermatitis, it has been seen in babies from the age of two months onwards to before the age of five years. The skin disorder tends to run in families but is not contagious and cannot be passed on to others.
Cause and triggers of eczema
There is no single known cause for the skin disorder. Both genetic and environmental triggers tend to play a role in perpetuating the disease. Some children diagnosed with Atopic Dermatitis when they are less than five years old, may grow up and not suffer from the problem at all; for others it may become a lifelong affliction.
Some triggers in the environment that tend to set off an Eczema flare up are:
- Extremely dry skin which is brittle or scaly
- Harsh chemicals found in commonly used products like soaps, shampoos, body washes or even laundry detergents
- Fluctuations in temperature extremes
- Extra emotional stress
- Allergies to pollen, pets, dust, mold, etc.
- Certain foods which may cause an allergic reaction
- Hormones rising and dropping suddenly, especially in women
Symptoms
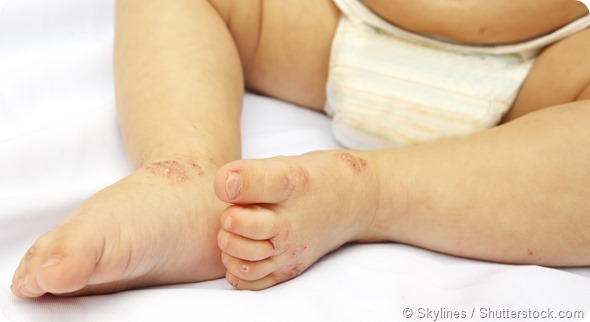
There are no typical symptoms for Eczema. In some babies the rash may be dry, red and itchy, whilst in others it may ooze fluid. Irrespective of these details, the rash most commonly appears on the face or scalp of the baby. In slightly older babies, the rash can be on the cheeks, bottom, hands, feet, elbow creases or behind the knees.
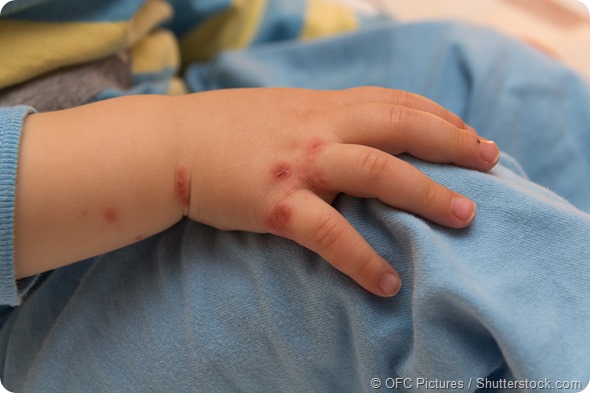
There can be multiple rashes on the body of the baby. The more these are scratched, the worse they become. As it progresses, the rash will develop a crust and begin to form dry scales which may continue to itch. The skin will become thick in the area the rash occupies.
Treatment options
The skin should be moisturised regularly and kept clean and dry using gentle skin cleaning products. If stress is a trigger, one must try and keep the baby calm and happy. While over-the-counter creams and ointments are easily available, a doctor should still be consulted before anything is used on the afflicted area of the skin.
Since Eczema causes irritation of the skin, there is an urge to scratch the area. It is important not to allow the baby to indulge this urge as scratching can cause the skin to break, and open wounds on the skin leave it vulnerable to more infections i.e., secondary infections.
If the symptoms begin to worsen, the doctor should be visited to get medication prescribed. They may provide topical immunomodulators or steroids to apply to the skin, in conjunction with antihistamine pills. These are generally prescribed when the baby has established food allergies.
Antihistamine ointments may also be used on the skin directly to counter allergy reactions. Oral antibiotics may be prescribed in cases where a secondary skin infection is flaring up. Doctors usually avoid giving babies oral medication if the ointments are able to control the Eczema.
Living with eczema
Eczema is an unpredictable skin disorder - it may simply disappear after a period of time, or crop up repeatedly for years. The best way to manage Eczema is to control exposure to triggers that may cause a flare up.
A daily skin care routine should be designed for the baby so that the skin is clean and moisturised. Ensure that you use a gentle skin cleaner and a perfume free moisturiser. The moisturiser should be applied all over the body after drying the skin post a bath. This ensures deep pore moisturising.
A baby’s delicate skin can be easily irritated by the harsh chemicals in most soaps and detergents. Try to wash their clothes in gentle cleaners. Don’t use fabric softeners or perfumed detergents that have more chemicals in them and may trigger the Eczema.
The biggest challenge is to ensure that the baby does not scratch the rashes. Since the urge can be quite strong, one must ensure that the fingernails of the baby are cut short and there are no jagged edges on the fingernails that may break the skin, causing an infection. Diverting the baby’s attention or using cloth mittens on the baby’s hands may prevent them from scratching.
Further Reading
Last Updated: Feb 26, 2019