Leprosy is a chronic granulomatous infection. It is caused by the slow-growing organism Mycobacterium leprae, which is an obligate intracellular parasite. It affects chiefly the skin and peripheral nerves.
Leprosy has a wide range of clinical manifestations, which depend upon the host immune response more than the virulence or multiplication rate of the bacillus. It has a long incubation period, from two to seven years, ranging between six months and 20 years. Seropositivity may occur months or years before a clinical diagnosis is made.
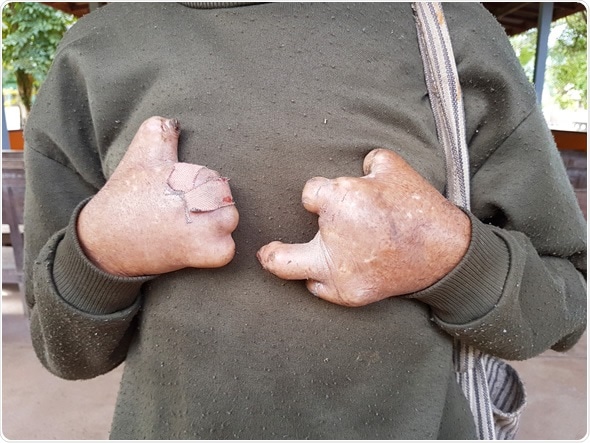
Closeup hands of asian old man suffering from leprosy, Thailand - Image Credit: Bidarat Tiemjai / Shutterstock
The typical manifestations of leprosy include:
- Hypoesthesia of skin lesions with the decrease in sensitivity – this follows the sequence of heat-pain-light touch insensitivity.
- The disease spectrum ranges from tuberculoid to lepromatous, corresponding to a high and low cellular immunity (Th1 and Th2 response) respectively.
- Cytokines released in tuberculoid disease include interferon (IFN)-γ, IL-2 and lymphotoxin-α with high phagocytic activity and granuloma formation due to macrophage and T-cell aggregation. In lepromatous disease, granuloma formation is reduced, and CD8+ cells are predominant. Patients in the borderline forms move between these two ends as the immune status shifts, and leprosy reactions are a characteristic feature of this state.
Clinical Forms
Lepromatous Leprosy
LL patients have the following features:
- Multiple small lesions, hypopigmented in dark-skinned individuals but coppery or reddish in lighter-skinned people
- Macules, papules, or nodules are found (termed lepromas) due to infiltration of skin lesions
- Lesions are shiny, symmetrical and widespread
- Loss of eyebrows and eyelashes (madarosis) and thickened skin over the face, giving rise to the peculiar appearance called “leonine facies”
- Thickening of the ears due to infiltration
- Lesions of the mucous membranes of the upper respiratory tract (including the trachea) and eyes
- Orchitis and bone lesions
- No hypoesthesia or reduced hair growth in early stages
- Edema of the limbs and hypoesthesia in advanced stages
- AFB globi in skin smear and nasal secretion or scraping
- Lepromin negative
Borderline Leprosy
This is the term used to describe unstable forms in which the clinical manifestations vary from time to time.
Borderline Lepromatous (BL)
- Large number of lepromatous lesions but normal skin in between, and somewhat asymmetrical in distribution
- Ring-shaped shiny lesions
- Slight hypoesthesia and reduction in hair growth over lesions
- Nerve thickening may or may not be present
- Many AFB in skin smear
- Lepromin negative
Mid-borderline Leprosy (BB)
- Several lesions
- Lesions are annular, raised and flat, or have a punched out appearance
- Characteristic lesions with erythema, outer borders fading out, inner borders clear, and central hypochromia, called the foveal spot
- Lesions are somewhat shiny
- Some hypoesthesia
- Hair growth over lesion reduced
- Moderate AFB in skin smear
- Lepromin negative
Borderline Tuberculoid (BT)
- One or a few lesions which are on the smaller side
- Lesions tend to be asymmetric, flat and well-defined
- Markedly insensitive
- More nerves thickened but irregularly, and less markedly
- Loss of hair significant
- No or few AFB in skin smear
- Lepromin weakly positive
Tuberculoid Leprosy (TT)
- Lesions are few and well-defined, and may be hypopigmented or reddish
- Asymmetric and localized
- Scaling often present
- Alopecia and anesthesia present due to dermal denervation in the affected area
- Neighboring nerves may be thickened
- Skin in areas of compression shows thickening due to increase in the keratotic areas, and ulceration may set in
- No AFB in skin smear or nasal scraping
- Lepromin strongly positive
- In primary neural leprosy, altered sensitivity may be the only clinical feature, with thickening of the nerve being variable
Indeterminate Leprosy
This refers to a phase in which the disease is not yet in any specific stage or type, such as a single lesion with slight loss of sensitivity and hypopigmentation, but no nerve thickening.
Leprosy Reactions
Leprosy reactions are changes in the leprous status as a result of altered balance between the host and the bacilli. They may occur before, during, or after treatment. They cause significant morbidity and permanent neurological disability.
Type 1 Reaction
This occurs as a delayed hypersensitivity event, usually in borderline forms. It reflects a heightened cellular immune response to the mycobacterial antigens. It may be a reversal reaction with improvement in clinical manifestations, or a degradation reaction with worsening of the disease features.
Treated patients become more tuberculoid in their manifestations, due to reduction in the number of bacilli. However, patients who are not on treatment exhibit increase in bacterial load, and the disease becomes lepromatous in form due to deteriorating cell-mediated immunity. In this case, typically the lesions become tender and erythematous, edema followed by scaling is observed, and ulceration may occur.
The appearance of systemic features depends on whether the individual is at the lepromatous end of the spectrum.
Type 2 Reaction
Also known as erythema nodosum leprosum (ENL), this reaction is the result of the body’s reaction to immune complexes deposited in the body, because of antigenic substances released by killed bacilli. It usually manifests as rapid and sudden deterioration in the clinical status during treatment of an individual with lepromatous leprosy or sometimes borderline lepromatous forms.
It is associated with the occurrence of symmetric nodules or target lesions, with systemic features such as fever, bone and muscle pain, and lymphadenopathy. More serious manifestations may include hepatitis or renal disease, and neural inflammation.
Parameters of inflammation are positive on testing. Necrotic forms of ENL show blocked vessels because of vasculitis following immune complex deposition in the vessel wall.
Lucio’s Phenomenon
This is a classic sign of Lucio’s leprosy and classic lepromatous leprosy. Blood vessels are obliterated by proliferating M. leprae in the capillary endothelium, which promote vascular endothelial overgrowth, clot formation, and finally occlusion of the lumen.
References
Further Reading
Last Updated: Jan 25, 2019