Leprosy is a chronic infection caused by the bacillus Mycobacterium leprae. It affects the skin, the peripheral nerves and the upper part of the airway, or the testes. It is transmitted by prolonged contact, usually through aerosols containing the nasal secretions, or droplets from these fluids. However, 95% of people are naturally immune to the infection. It can also be transmitted from mother to child via the placenta.
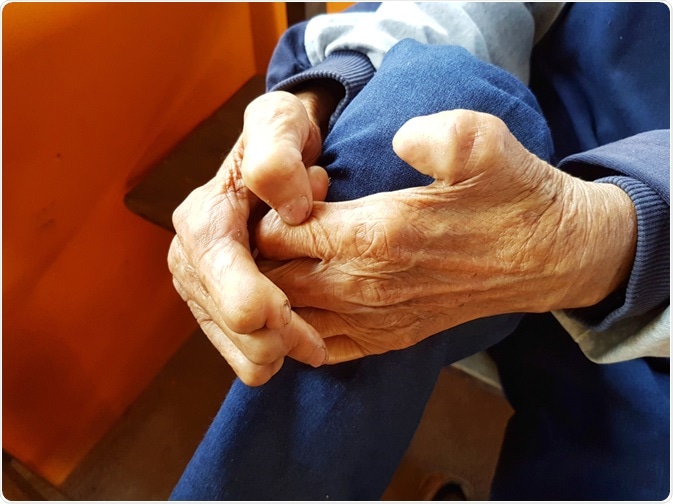 Image Credit: NikomMaelao Production/Shutterstock.com
Image Credit: NikomMaelao Production/Shutterstock.com
Nerve involvement results in sensory loss, motor or muscular weakness, and autonomic nerve damage, depending on the nerves involved.
Sensory loss of the hands and feet makes them vulnerable to burns and injuries. Repetitive damage eventually causes loss of fingers or toes, or the whole hand or foot, which are the classic deformities of leprosy. Loss of eye sensation leads to loss of the normal compensatory reflexes that prevent damage due to the accidental entry of dust or other particles into the eye. The result is loss of vision.
Injury to the motor nerves leads to weakness and paralysis of specific muscles, leading to deformities of the hands and feet. These include wrist drop, claw hand, and foot drop. Lagophthalmos is where the eye cannot close properly because of paralysis of the eye muscles.
Autonomic nerve deficit manifests in the inability to sweat, leading to dry cracked skin and an increased susceptibility to secondary bacterial infections of the skin. Hair loss can lead to lack of eyebrow hair.
In the absence of nerve disease, leprosy is like any other minor infection. It takes 2-10 years to show the first symptoms. The patient rapidly becomes non-infectious following the start of treatment, after the first few doses. There is no need for isolation, therefore, during the course of treatment.
Leprosy, in general, requires a long incubation period. It is more easily caught by children. Other persons at higher risk include those who are in close and prolonged contact with leprosy victims, or who live in regions where leprosy is widespread. This includes several countries in South America, Africa, India, Nepal and Tanzania.
There are two forms of leprosy: tuberculoid and lepromatous. The WHO also classifies it as multibacillary and paucibacillary. The multibacillary type has larger and more numerous skin nodules, and multiple skin patches, which often shows thickening, loss of sensation and lightening of skin coloration. These patches are symmetrically distributed. Nasal congestion or epistaxis are often associated with this type. In contrast, the paucibacillary type has only a few skin lesions, which show a similar loss of sensation. These lesions persist for weeks to months.
Other features include enlargement and nodularity of superficial nerves, which is best felt at the elbow or the knee, corneal drying, ulcers on the soles of the feet and muscle weakness.
Complications of leprosy
- Deformities due to large unsightly nodules, loss of fingers and toes, destruction of the nose and loss of eyebrows
- Permanent sensory loss
- Permanent paralysis of some muscles
- Nerve destruction
Diagnosis of leprosy
Early diagnosis is extremely important, as it prevents deformity, limits the spread of the disease and enables resumption of normal life soon after treatment starts, with no residual stigmata of the disease.
Various diagnostic techniques include:
- Skin scraping test with staining to visualize the bacteria under the microscope
- Skin biopsy
- Lepromin skin test – injecting a minute amount of leprosy bacillary antigen under the skin to test the reaction. Useful in differentiating lepromatous from tuberculoid forms. It is not useful for diagnosis itself, since it is weakly positive or negative in the tuberculoid form.
What is Leprosy? (Chronic Infectious Disease)
Treatment of leprosy
Formerly leprosy could be controlled but not cured due to the non-availability of bactericidal drugs. Nowadays, multiple anti-leprosy drugs are used to cure leprosy with a treatment course that may last from 6 to 24 months. Further treatment may include surgery and physical rehabilitation, depending on the extent of deformity and the stage of the disease.
Drugs useful in leprosy include:
- Dapsone
- Rifampicin
- Clofazimine
- Fluoroquinolones
- Macrolides
- Minocycline
Multi-drug therapy prevents the emergence of drug resistance. It should be continued under regular review, till the specified duration is complete, and the eradication of the infection is confirmed.
Anti-inflammatory drugs like aspirin, or steroids like prednisone, are used to arrest granuloma formation and prevent further nerve damage.
Prevention of leprosy
Avoid long-term contact with infected people till they have received a single monthly dose of multi-drug treatment.
References
Further Reading
Last Updated: Feb 21, 2023