Shaken baby syndrome (SBS) is a condition that is recognized in infants who have been violently shaken. It is the leading cause of death in abused infants. Brain cells are easily destroyed by the forces generated during the shaking.
This sets in motion a series of events, namely hypoxia, edema, increased intracranial pressure, ischemia, and decreased cerebral perfusion pressure, which cause neurological dysfunction and in extreme cases death.
Affected infants may present with mild symptoms that may go unnoticed or be thought to be caused by other etiologies, such as viral illness or colic. Severe symptoms are recognized immediately following the trauma. Retinal and subdural hemorrhages are the clinical hallmarks of SBS.
Other associated symptoms include lethargy, vomiting, poor appetite, unconsciousness, convulsions, and coma. Affected infants may have an increased head circumference and bulging soft spots on the head. In addition to this, they may have bruises, signs of the abuse and thus, a team of various healthcare professionals are needed for definitive diagnosis.
Differential diagnosis
Nearly all infants, approximately ninety-five percent, who present with a grave intracranial injury are victims of being violently shaken. The remaining five percent may suffer injury as a result of accidents like motor vehicle crashes.
Rarely, birth injury may be the cause of an infant having chronic subdural hemorrhage. Medical problems that should be considered include arteriovenous malformations, infectious effusion, and connective tissue as well as bleeding disorders.
Chronic subdural hemorrhage may also be seen in very rare conditions, which cause subdural bleeding. For example, in glutaric aciduria type 1, there is an enlargement of the subdural spaces with corresponding stretching of bridging veins. These stretched vessels easily tear in response to even minimal trauma. Glutaric aciduria can be ruled out with the help of biochemical screening tests.
Assessment
It is not an easy task to detect or diagnose victims with SBS. However, SBS should be considered in any child or infant who collapses without an obvious cause. In order to avoid under-recognizing the condition, the threshold for suspicion must be held very low. It is imperative that healthcare workers take an extensive medical as well as social history from the caregivers of the infant. Follow-up investigations include imaging as well as laboratory and physical tests.
Investigations
Neuroimaging is a key technique in terms of diagnosing SBS. Intracranial pathologies such as cerebral edema and subdural and subarachnoid hemorrhage may be identified with the help of CT scans. These scans are usually the tool of choice in emergency situations.
In contrast, MRI scans may be performed a few days later to ascertain the extent of the neurological impairment. In very young children, ultrasound may also be used to detect intracranial hemorrhage.
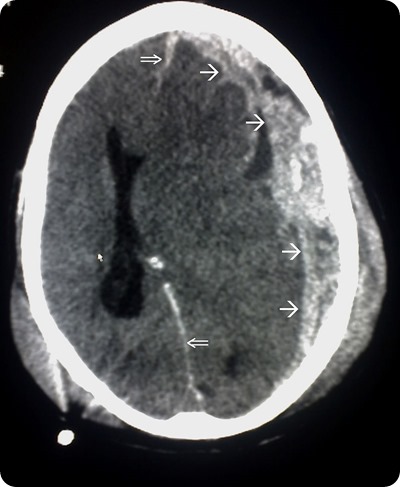
CT scan flowing head trauma, the single arrows mark the spread of the subdural haematoma and the double arrows mark the midline shift. Source: commons.wikimedia.org
Approximately 9 in every 10 infants with SBS will have retinal hemorrhages that are diffuse, bilateral, and multilayered. A further ocular pathology that may be seen includes papilledema.
Thus, ophthalmological examination is required to support a definitive diagnosis. Other laboratory tests such as a complete blood count, biochemical panels, cerebrospinal fluid examination, and urine cultures are all supportive when diagnosing SBS. Skeletal assessment must also be conducted in cases of suspected abuse.
References
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1757926/pdf/v078p00732.pdf
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3210040/
- http://www.uptodate.com/contents/child-abuse-eye-findings-in-children-with-abusive-head-trauma-aht
- http://www.uptodate.com/contents/child-abuse-evaluation-and-diagnosis-of-abusive-head-trauma-in-infants-and-children
Further Reading
Last Updated: Feb 27, 2019