Phantom pregnancy or pseudocyesis is rare in developed countries such as the US, but much more common in developing countries. This is because such contexts put a very high value on fertility with respect to the status given to a woman.
Since the primary female functions are thought to be childbearing and field work, which is true inmany cultures, this aspect of womanhood takes on a disproportionate importance in the eyes of the women who grow up in such an environment. Infertile women may be subjected to increased domestic abuse in such cultures.
Cultural considerations before treating false pregnancy
When sons are highly esteemed as superior to daughters, even women who have borne a number of children (but no or very few sons) may aspire to bear one. This longing is intensified as a woman reaches the end of her childbearing years, or faces the loss of a valued relationship, or is presented with the end of attempts to treat her presumed infertility.
Security, the desire to have a man marry her for love or to emerge from poverty-stricken circumstances, or the need to establish a marital or other relationship on a firm footing, are other factors which may lead to the occurrence of a phantom pregnancy.
This preamble will help us understand how best to treat this phenomenon, which is not purely medical in nature. Instead, sociocultural norms are pre-eminent in its genesis, and will be important in its treatment. The most prominent of these appear to be a low socioeconomic status, which results in insecurity and dependency, as well as low self-esteem and powerlessness.
Revealing the truth
Treatment is concerned with alleviating the impact of these factors. The patient needs to be told about the falsity of her assumption that she is pregnant, with such evidence as can be garnered. This may include imaging of the uterus showing that it is empty.
In addition, she should be reassured that this does not mean she was faking a pregnancy, but actual neuroendocrine changes did occur within her body, leading to signs and symptoms originating from the reproductive organs.
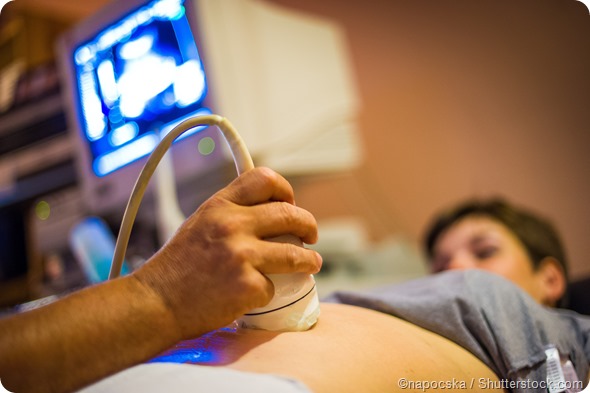
Supporting the patient
Some families may be concerned that the woman has a mental disorder because she had a false idea that she was pregnant. They need to be assured that this is not the case, but she is emotionally and mentally stable.
It is vital to support the patient with adequate counseling because she may develop depressive symptoms following the realization that she is not pregnant. Family therapy is ideal to avoid recurrence of the condition.
Likewise, psychodynamic and supportive psychotherapy often plays a crucial role in the proper management of pseudocyesis. Finally, it is quite important to consider potential related psychotic features that might be observed in women with this condition.
Further Reading
Last Updated: Feb 27, 2019