Keratoacanthoma is a slow-growing skin tumor with a characteristic type of lesion. Its appearance closely resembles that of another, a more aggressive type of skin tumor called squamous cell carcinoma or SCC, and hence it should be diagnosed accurately. A squamous cell carcinoma needs to be treated immediately to contain its malignant spread.
The epidermal growth called keratoacanthoma usually tends to occur on areas of the skin exposed to the sun. They mostly occur on the hands and faces of people. In rare cases, they may occur in a non-sun-exposed area such as the nasal vestibule. This can cause pain within the nose each time pressure is applied to the area externally. Fair-skinned people are more prone to this skin condition.
What do the Keratoacanthoma Skin Lesions Look Like?
Keratoacanthomas are epithelial neoplasms or abnormal growths of tissue found in the outer layer of the skin. They are considered benign skin tumors. These growths consist of flesh with a keratin center.
Keratin is a structural protein that protects the epithelial cells. Simply speaking, it is the tough material that makes up the outermost layer of the human skin. It is also the protein that human hair is made up of. In a keratoacanthoma, the keratin makes up the tough plug in the middle of the lesion. This portion will fall out later, even in the absence of treatment, and spontaneous healing of the skin lesion begins to occur.
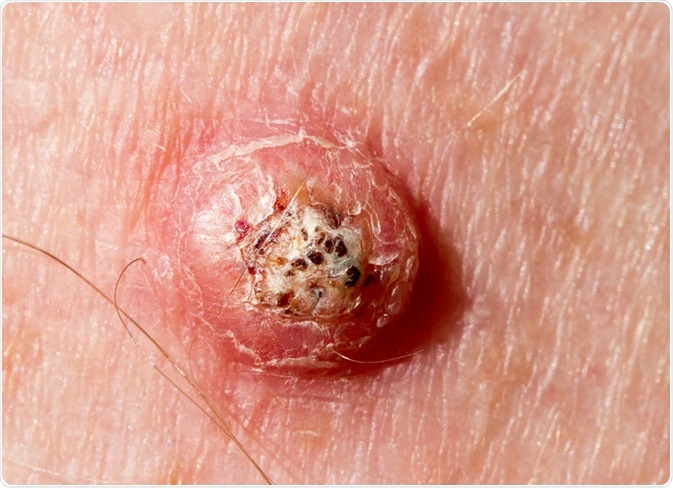
Keratoacanthoma on the leg of a 64-year-old male at six weeks development stage. Image Credit: Peter Mullineux
What Symptoms Accompany a Keratoacanthoma?
A keratoacanthoma is likely to start in the shape of a smooth dome. The initial size is about one to two mm. Over a period of a couple of weeks, it grows to a diameter of 1-3 cm. The dome will by now have a hard keratin core. At some point within this period, the lesion will stop growing.
The neoplastic nature of the keratoacanthoma then appears to have become dormant. It will not change its shape or size for nearly 6-8 weeks. Then, over the next few months, the abnormal growth will begin to regress. The skin lesion takes about 2-12 months to heal completely. The exact period may differ from person to person.
As the healing progresses, the edges of the dome-shaped growth will begin to flatten out. The core of keratin will begin to peel and eventually fall off. The shape then resembles that of a volcano with a crater. Slowly the skin will be healed, but a scar will remain at the site of the lesion.
While the lesions are on the skin, they may cause itching and mild discomfort for the individual. Sometimes the abnormal growth may be painful to touch. It is best to avoid touching them as far as possible to minimize the discomfort experienced.
Treatment and prognosis of keratoacanthoma
Since keratoacanthomas closely mimic the SCC skin tumors, it is essential to arrive at an accurate diagnosis. This is done by histopathologic examination of the lesion after its surgical removal by the dermatologist. As an SCC can progress really fast, the diagnosis should be made as early as possible. In most cases, since these tumors are sometimes indistinguishable, even on biopsy, excision or removal of the keratoacanthoma is highly recommended.
Other methods are also used if surgical excision is not possible or appropriate for any specific patient. In such cases, the keratoacanthoma can also be scraped off using a curette (a spoon-like surgical instrument). The patient will be given local anesthesia before this procedure. The raw area will be cauterized, following which stitches will be applied so that the skin can heal evenly and rapidly. Regular dressing of the wound may be needed initially.
Once the tumor is removed, the keratoacanthoma is considered cured as long as the dermatologist does not leave behind any of the core material. The neoplasm is unlikely to recur. The procedure will leave a scar on the skin. Should the lesion prove to be an SCC on biopsy, then additional treatment will be recommended by the dermatologist.
Besides curettage and cauterization, the keratoacanthoma may be removed using cryotherapy. Cryotherapy involves freezing the keratoacanthoma using liquid nitrogen or carbon dioxide snow. A cotton-tipped applicator is dipped in liquid nitrogen and applied to the affected portion of the skin. This treatment is relatively safe and reliable and not too expensive.
Another treatment option for keratoacanthoma is radiation therapy. X-rays are used to cause irreparable damage to the cells' DNA within the tumor so that the neoplastic cells are killed off. Radiotherapy is not suitable for all skin tumors, as different cells vary in their sensitivity to radiation. This method is recommended for SCC. It is not used to treat keratoacanthomas. Podophyllin, methotrexate, topical 5-fluorouracil cream and retinoid therapy are some other options for this tumor.
Keratoacanthoma: cancer or not? Squamous cell carcinoma vs Keratoacanthoma pathology histology
Further Reading
Last Updated: Dec 16, 2022