Leprosy is an infectious disease caused by a rod-shaped, microaerophilic bacillus Mycobacterium leprae. While it is relatively uncommon, it has been dreaded since ancient times because of its disfiguring and disabling nature. Even today it is the cause of much discrimination and poverty, as the deformities caused by this bacterium are permanent without reconstructive treatment.
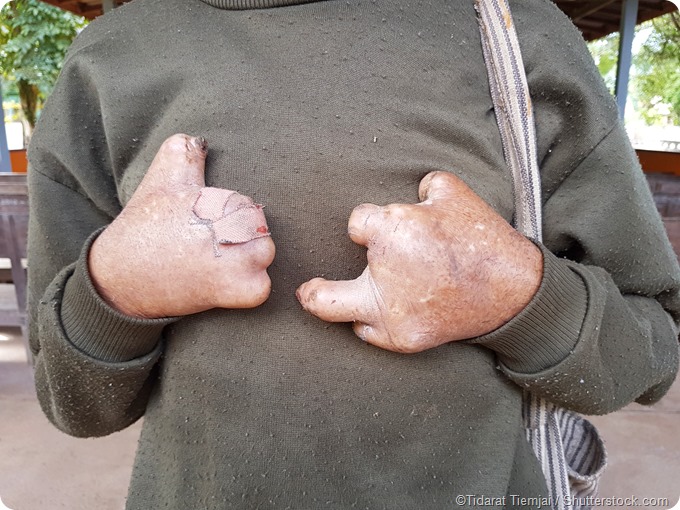
Need for leprosy research
It is no wonder that the questions are asked why so much research devoted to leprosy. Some of the reasons include:
- Leprosy is a completely curable disease in the majority of new cases
- Its deformities and disabilities are completely preventable by simply diagnosing and treating it early, as in most instances they arise from injuries secondary to neuropathy and not because of the bacillary infection itself
- The stigma of leprosy is almost unbearable and all-encompassing, denying the affected person human dignity
Areas of research
The International Federation of Anti-Leprosy Associations (ILEP) is developing a strategy which focuses on reducing leprosy transmission by research in five areas:
- Current management of index cases and contacts
- Diagnostic tests employing sensitive and specific biomarkers for detecting leprosy early, using polymerase chain reaction (PCR) technology and skin test antigens for field work
- The feasibility of chemoprophylaxis utilization in field settings
- Leprosy vaccine development other than BCG
- Strain typing to find out how present programs are affecting transmission
Breaking transmission
This resulted in new approaches to break the chain of transmission and thus reduce the future burden of disease, such as the viability and usefulness of administering chemoprophylaxis to healthy household contacts. For instance, when a single dose of rifampicin was given to contacts, the incidence of leprosy in contacts went down by over half.
The exact mode of transmission of leprosy is not yet conclusively proven, though the risk of infection has been shown to be highest among household contacts, and lowest among those who had no known contact with a leprous individual. Strain typing is being done in different regions of the world to identify the existence of an animal reservoir, such as the nine-banded armadillo in the US. This may help to detect patterns of transmission in endemic areas.
Research is also required to assess how HIV infection affects leprosy and its transmission, manifestations, leprosy reactions, and reaction to drug treatment. Some findings suggest that there is a higher frequency of immune-mediated responses that complicate leprosy in co-infected patients.
LSU researchers look into transmission of leprosy
Vaccine development
Since the primary epidemiologic indicator of current transmission is new cases in children, vaccines to prevent infection (immunoprophylaxis) are being developed and studied, as well as ways to increase the efficacy of existing vaccines.
For example, new strains of mycobacteria (such as Mycobacterium habana, Mycobacterium indicus pranii, Mycobacterium vaccae) and the addition of killed mycobacteria to BCG are all being tested to find protection rates, as well as potential side effects. The Mycobacterium indicus pranii vaccine developed in India is being released for use, while one developed by the Infectious Diseases Research Institute is being tested.
Treatment and chronic disability management
It is important to study the use and effectiveness of existing and newer drugs in leprosy, such as rifampicin, ofloxacin, minocycline, and clarithromycin. Some may be effective as single-dose supervised regimens in some types of paucibacillary leprosy.
Intermittent fully supervised regimens, in contrast to self-administered daily regiments, may make a huge difference in the cure rate, the development of secondary disabilities, and the emergence of drug-resistant strains. It is also important to identify the occurrence of post-treatment relapses and the development of resistance.
Innovative ways of community intervention, education, and motivation to garner support for socioeconomic rehabilitation of leprosy patients are being studied to help achieve early diagnosis and treatment, which will help prevent disability.
References
- http://trstmh.oxfordjournals.org/content/107/9/533.full
- http://www.who.int
- https://www.niaid.nih.gov/diseases-conditions/leprosy-hansens-disease
- https://www.ncbi.nlm.nih.gov/pubmed/16728321
Further Reading
Last Updated: Dec 29, 2022