In the early stages of the therapy for lymphedema, it is common for patients to require daily treatment to induce lymph fluid drainage and reduce the volume of the affected area. This intensive phase may take several weeks, depending on the severity of the condition.
The maintenance phase of therapy follows this and is strongly driven by the individual patient, involving several techniques to help prevent worsening of the condition. The aim of this phase is to sustain the reduced swelling that has been achieved in the intensive phase.
Adequate patient education is required to allow individuals to manage the condition with self-massage techniques and the use of compression garments to stimulate the flow of lymph fluid. Movement exercises are also recommended to improve lymph drainage and reduce the risk of fluid accumulation. It is important to continue to provide support to the patient and conduct regular reviews to ensure the treatment progresses as well as can be expected.
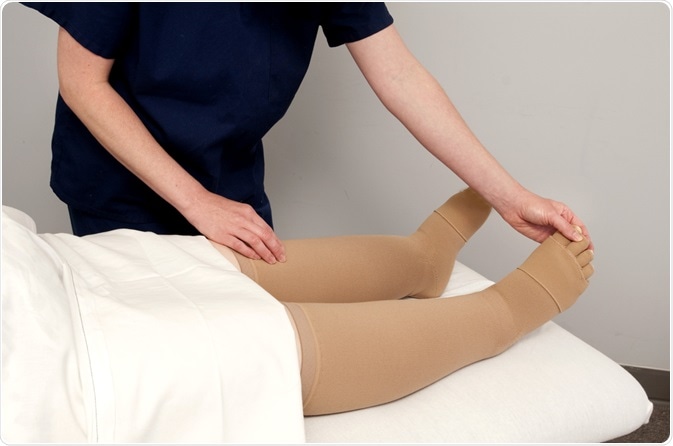 Physiotherapist treating a patient who has lymphedema with pressure stockings. Image Credit: futurewalk / Shutterstock.com
Physiotherapist treating a patient who has lymphedema with pressure stockings. Image Credit: futurewalk / Shutterstock.com
Decongestive lymphatic therapy (DLT)
Decongestive lymphatic therapy is the first-line treatment for lymphedema and is very useful in the control of symptoms, although it is not able to cure the condition. There are four main components of DLT, which include:
- Compression bandages to remove excess fluid from the affected limb and reduce future accumulation.
- Adequate skincare to reduce the risk of infection.
- Movement exercises to improve drainage of the lymph fluid from the affected area.
- Manual lymphatic drainage (MLD) and massage techniques to stimulate lymph fluid flow and reduce swelling.
The lymphatic system relies on the movement of the surrounding muscles in the body to move the lymph fluid around the body. Compression bandages or garments, such as sleeves, gloves, stockings or tights, can be fitted around body parts affected by lymphedema to support the muscles and promote the movement of fluid away from the area. It is often beneficial to apply the compression bandages to the affected limb following an MLD session to reduce the return of fluid.
Eventually, the patient should be able to apply the bandages by themselves correctly, to continue with the maintenance of their therapy independently. Velcro wraps are useful in this respect as they increase the ease of self-application.
Appropriate care for the skin is essential for an individual that suffers from lymphedema to reduce the risk of infection. Infections such as cellulitis are more common among these patients and care should be taken to protect skin from cuts and other trauma.
Movement exercises designed to stimulate the muscles that promote lymph drainage are important in the prevention of swelling related to lymphedema. This usually involves a combination of targeted muscle exercises with whole body activities such as swimming, cycling or walking.
MLD plays a central role early in therapy to move the fluid away from swollen areas to where it can be drained out of the body and is usually conducted by a specialized massage therapist. Simple lymphatic drainage (SLD) are massage techniques can also be taught and carried on by the individual or a carer during the maintenance phase to prevent recurrence of swelling.
Treating And Managing Lymphoedema - Macmillan Cancer Support
Other treatments
In rare cases, surgery may be required in the treatment of lymphedema. This may involve the removal of excess skin, tissue or fat from the affected limb or the restoration of fluid flow in the lymphatic system. Surgery is reserved for severe cases when the size of affected limbs significantly inhibits the individual's quality of life.
Liposuction involves the insertion of a thin tube via a small incision in the skin that is used to remove the fat from the area A compression garment should be worn following this procedure to reduce swelling, usually for at least a year.
References
Further Reading
Last Updated: Nov 26, 2022