The diagnosis of lymphedema can be difficult because early signs of the condition can be subtle and patients may not be aware of them worsening.
Diagnosis should be made based on a history of symptoms and medical conditions, in addition to a physical examination. There are also several diagnostic tests that are sometimes used.
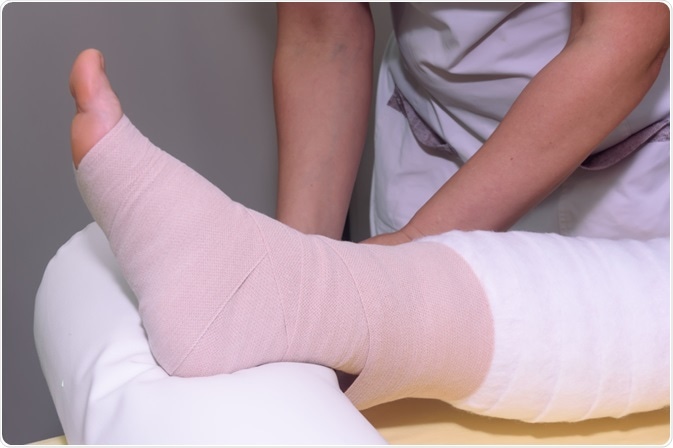 Image Credit: Petia_is / Shutterstock.com
Image Credit: Petia_is / Shutterstock.com
Symptoms and medical history
Initially, it is important to establish a thorough medical history of the individual and targeted questions about the specific symptoms of lymphedema should be addressed.
Secondary lymphedema is the most common type, which occurs as a result of identifiable damage to the lymphatic system. It is particularly common in patients that have previously undergone radiotherapy or other treatment for cancer, including surgical removal of lymph nodes.
Primary lymphedema may have a familial link due to gene mutations that affect the development of the lymphatic system. For this reason, it is important to establish if there is a family history of lymphedema.
Physical examination
A physical examination is important to establish changes to the affected body part and the involvement and severity of lymphedema.
This can be done quantitatively by measuring the size of the body part and comparing it to earlier measurements although the body part on the other side of the body.
The volume of the limb can be measured in various ways, including:
- Circumference with tape measure
- The volume of water displaced from a tank when a body part is immersed
- Perimetry outline of limb with infrared light
Diagnostic Evaluation and Medical Management of Lymphedema - Lymphedema & Wound Care
Diagnostic tests
Further diagnostic tests are not required in most cases but are occasionally used to assess the condition and monitor changes. These tests include:
- Bioimpedance testing – electrodes placed on the body deliver a mall electric charge to measure the presence of fluid in bodily tissues.
- Lymphoscintigraphy – radioactive dye infection to track movement of fluid in the lymphatic system and identify blockages.
- Magnetic resonance imaging (MRI) – scan using magnetic resonance to visualize bodily tissues and involvement of lymphatic system.
- Ultrasound – scan using high-frequency sound waves to visualize bodily tissues and involvement of lymphatic system.
- Computerized tomography (CT) – scan using X-rays and computer to depict lymph nodes in detail.
These testing methods can be used to diagnose lymphedema and monitor changes in the condition as treatment commences.
Cancer patients
Patients that have undergone cancer therapy recently or in the past have an increased risk of lymphedema and should be monitored for signs of the condition regularly.
It is important that these individuals are aware of the early signs and symptoms of lymphedema, such that they can recognize the condition earlier if it presents. Aftercare treatment programs commonly help patients to understand the individual risks they face and what they can do to help identify signs of lymphedema and other conditions.
Differential diagnosis
There are several other health conditions that may lead to swelling of the limbs and present with similar symptoms to lymphedema but require different treatments. These conditions include blood clotting and infection independent of lymph nodes.
Additionally, edema arising from venous insufficiency is commonly mistaken for lymphedema. When this condition progresses, it can lead to the involvement of the lymphatic system and require similar treatments, but in the early stages of disease, it should be viewed as a separate condition, with distinct symptoms and treatments.
References
Further Reading
Last Updated: Dec 22, 2022