Noonan syndrome is a condition notable both for its frequent occurrence and phenotypic variability. It is one of the most common non-chromosomal disorders in children with congenital heart disease, with an estimated prevalence worldwide of 1 in 1000-2500. The average age at diagnosis is nine years, and life expectancy is likely normal if serious cardiac defects are absent.
With total penetrance but variable expressivity, the phenotype of this autosomal dominant disorder ranges from mild cases (often unrecognized and undiagnosed) to severe ones when diagnosis is already possible at birth. The principal features of Noonan syndrome are short stature, characteristic facial appearance that changes with age, congenital heart defects, webbed or broad neck, pectus deformity and mild intellectual handicap in some instances.
 Image Credit: nito / Shutterstock.com
Image Credit: nito / Shutterstock.com
Characteristic facial features
Facial appearance in Noonan syndrome alters with age. Newborns have a broad and high forehead, wide-spaced and downward slanting palpebral fissures, ptosis, epicanthal folds, a depressed nasal root with upturned nasal tip, higharched palate, micrognathia, low posterior hairline and the short and/or webbed neck.
During infancy the head is relatively large when compared to the face, with a prominent and tall forehead. Ptosis, hypertelorism and thick hooded eyelids remain characteristic, while the nose is short and wide with a depressed root. In later childhood years, the face sometimes appears coarse or even myopathic, with prominent eyes and thick lips.
In the adolescent and young adult years, the eyes become less prominent and the neck appears less short with a prominent trapezius. In older adults, nasolabial folds are exaggerated and the skin appears transparent and thin. They can also present with thick hooded eyelids, wrinkled skin and a high anterior hair line, albeit all aforementioned facial features can be subtle.
Cardiovascular anomalies
Cardiac abnormalities can be found in over 80% of patients with Noonan syndrome, and pulmonary valve stenosis with dysplastic leaflets is the most frequently observed cardiac lesion. The pulmonary valve is often only mildly dysplastic with no significant obstruction, thus the long-term prognosis for these patients is excellent. Certain individuals with Noonan syndrome that experience a rapid progression of valvular obstruction require surgery.
Hypertrophic obstructive cardiomyopathy with asymmetrical septum hypertrophy occurs in approximately 20% of patients. The finding is poorly understood with notable variability in course and prognosis, but is significantly associated with mortality in infancy. Akin to non-syndromic familial hypertrophic cardiomyopathy, this type of cardiomyopathy exhibits myocardial disarray and thick-walled coronary arteries in the intramural space.
Other common structural cardiac anomalies include atrial or ventricular septal defects and tetralogy of Fallot. Persistent ductus arteriosus can also occur in 3% of cases. With the exception of transposition of the great arteries, virtually every type of heart disease has been described in Noonan syndrome. Cerebrovascular anomalies (such as AV-malformations and aneurysms) have also been associated with this syndrome.
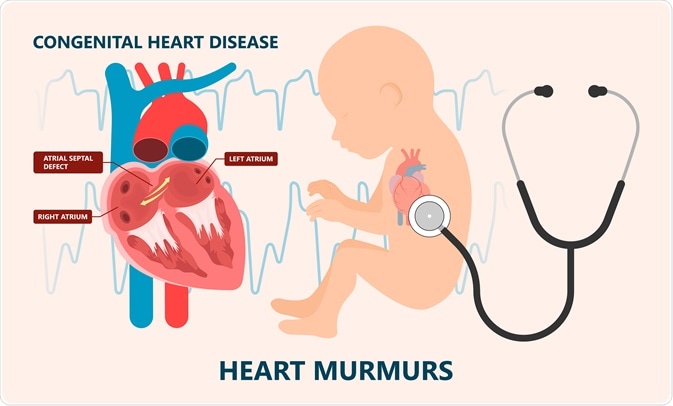 Atrial or ventricular septal defects are common structural cardiac anomalies in Noonan syndrome. Image Credit: ruamray / Shutterstock.com
Atrial or ventricular septal defects are common structural cardiac anomalies in Noonan syndrome. Image Credit: ruamray / Shutterstock.com
Other findings
More than 90% of patients with Noonan syndrome have pectus excavatum or pectus carinatum with subsequent shield-like chest deformity. Kyphosis (hunchbank), scoliosis (abnormal spinal curvature) or clubfoot is present in 10–15% of patients. Many affected individuals have hyperextensible joints and muscular hypotonia, albeit the latter generally improves with time.
Ocular anomalies are among the most common findings in Noonan syndrome, and patients most often present with strabismus, refractive errors and amblyopia. Nystagmus and anterior segment changes (prominent corneal nerves, cataracts, panuveitis) are also frequently found, whereas coloboma, retinitis pigmentosa, fibrosis of extraocular muscles and corneal rupture are rare.
Infants with Noonan syndrome generally exhibit a delay in early developmental milestones; the average age of sitting is at 10 months of age, while walking and talking occur closer to 2 and 2.5 years of age, respectively. Most infants have feeding difficulties that can lead to failure to thrive. Mild mental retardation can occur in up to 35% of affected individuals; however, IQ can range from 64 to 127.
Hearing loss due to otitis media is commonly observed. Abnormalities of pigmentation in Noonan syndrome include multiple pigmented nevi, cafe-au-lait spots, as well as lentigines. Up to 80% of boys diagnosed with Noonan syndrome have unilateral or bilateral cryptorchidism. Lymphatic vessel dysplasia, hypoplasia or aplasia can lead to lymphedema and lymphangiectasia.
As mentioned before, short stature represents one of the cardinal features of Noonan syndrome, although adult height is not always adversely affected. Despite a normal appearance at birth – with height and weight within the normal range – after merely a few months height growth evidently slows down. That results in a significant short stature (i.e. falling below the third percentile of height) for over 70% of individuals with Noonan syndrome.
References
Further Reading
Last Updated: Feb 9, 2021