The initial diagnosis of onychomycosis is usually done by inspection of the affected area and questioning the patient about their history of the symptoms. Discussing the family history of the condition may be warranted, as there is a possible hereditary link. Laboratory tests are often needed to confirm the diagnosis, as some differences cannot be confirmed upon visual inspection.
Onychomycosis - What is it and how is it treated?
Distinguishing onychomycosis
When performing the diagnosis of nail infection, it is important to distinguish symptoms of onychomycosis from several similar conditions, as they can be easily confused. In fact, in approximately half of all cases where nail fungus is suspected, another form of nail deformity is responsible.
Other conditions that may be mistaken for onychomycosis include:
- Nail psoriasis
- Lichen planus
- Contact dermatitis
- Nail bed tumors (e.g., melanoma)
- Trauma
- Yellow nail syndrome
- Chronic paronychia
- Normal nail aging
It is important that the correct diagnosis is made, as treatment is usually specific to each condition and misdiagnosis may lead to inadequate treatment, allowing the infection to worsen with extended time. Additionally, this can lead to unnecessary exposure to medications and an increased risk of side effects.
Diagnosis
Laboratory confirmation is often needed to accurately determine the condition that is responsible for the symptoms. Nail scrapings or clippings are usually used as the culture for microscopic examination. There are three main tests used in the laboratory, which include a potassium hydroxide smear, culture, and histology. For optimal sensitivity in diagnosis, recent results show that direct smear and histological examination performed together to yield the best results.
In order to identify non-dermatophyte molds accurately, it may be necessary to collect several samples for laboratory testing.
Types of onychomycosis
There are four main types of onychomycosis, which should be differentiated during the diagnosis process. These types include distal subungual, white superficial, proximal subungual, and candidal onychomycosis. The particular differences between each of these types are outlined below.
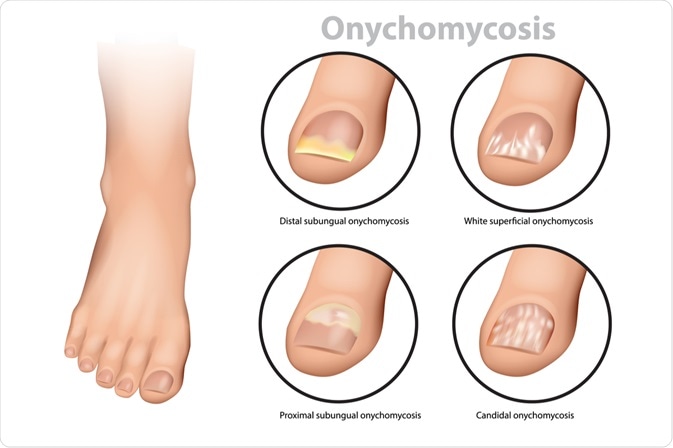
Image Credit: Sakurra / Shutterstock.com
Distal subungual onychomycosis
Distal subungual onychomycosis is the most common form of onychomycosis. Thichophyton rubrum is frequently the cause of this type of infection, which affects the nail bed and underneath the nail.
This form of onychomycosis involves the characteristic discoloration and weakening of the nail, which is not associated with pain in the majority of mild to moderate cases.
White superficial onychomycosis
When the outside layers of the nail plate are predominantly affected by the invasion of fungus, “white islands” can be formed on the plate, which is characteristic of white superficial onychomycosis. This form of onychomycosis is less common than the distal subungual type and accounts for approximately 10% of all presenting cases.
It is common for white superficial onychomycosis to be a misdiagnosis of a condition with similar symptoms called keratin granulation. Keratin granulation is not caused by a fungal infection but is rather a reaction to nail polish that results in nails that appear chalky white. Both conditions usually present with white discoloration of the nail; therefore, the differential diagnosis should be made by taking a history of nail polish use and with the confirmation of a laboratory test.
Proximal subungual onychomycosis
Proximal subungual onychomycosis is an infection that involves fungal penetration through the proximal nail fold into the new nail formation. This type is the least common form of onychomycosis in the general population, although people who are immunocompromised are significantly more susceptible to this type of infection.
Candidal onychomycosis
Candidal onychomycosis infection occurs when Candida albicans invades the fingernails. This type of onychomycosis is much more common in individuals who often immerse their hands or feet in the water, such as swimmers. Most cases involve previous damage to the nail plate by either an infection or trauma, which was then exposed to the infective fungus.
An accurate diagnosis offers the benefit of more effective treatment and usually results in better outcomes for patients. It is important that the examination and appropriate tests are undertaken to avoid misdiagnosis.
Further Reading
Last Updated: May 5, 2021