Oral thrush, which is also referred to as oral candidiasis, is a fungal infection caused by the yeast Candida albicans. This fungus exists naturally in the mouth and is one of the “beneficial floras” residing in the oral cavity. However, oral thrush occurs when the fungus overgrows and starts to cause symptoms.
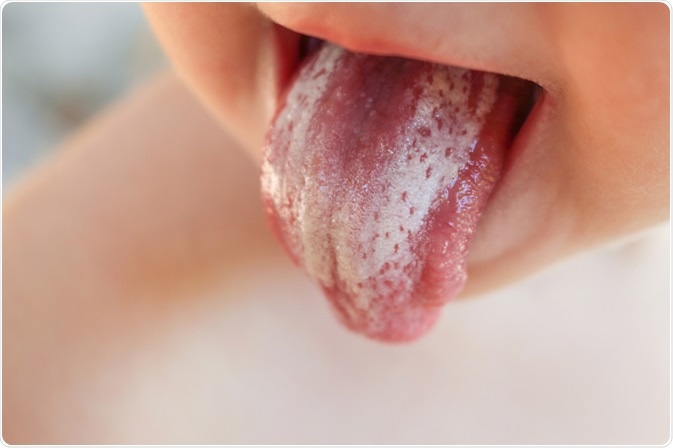 Image Credit: Victoria 1 / Shutterstock
Image Credit: Victoria 1 / Shutterstock
Oral thrush can affect any individual at any age, but it is most commonly seen in babies. Adults are more likely to develop oral thrush if they are elderly, have a compromised immune system, are taking certain medications, or have certain health conditions. For healthy people, the presence of Candida albicans does not cause any serious problems; however, for people with weakened immunity, it can be more serious and difficult to manage.
What are the symptoms of oral thrush?
The symptoms of oral thrush may develop quickly or slowly, depending on the cause of the problem and the immune status of the patient. Symptoms may persist for any period from a few days to months.
There are various signs and symptoms associated with oral thrush. These include:
- White lesions (plaques) on the tongue, on the inside of the cheeks, and sometimes the roof of the mouth. The lesions are difficult to wipe away and may leave red areas that slightly bleed. The white patches may also develop on the gums and tonsils.
- Some lesions may appear slightly elevated and may resemble cottage cheese
- Soreness and redness inside the mouth
- Loss of taste
- Cracks and redness at mouth corners
- Burning or pain in the mouth
In acute conditions like cancer or HIV/AIDS, the lesions can spread down the esophagus. This condition is known as Candida esophagitis, which can make swallowing difficult and cause the sensation of food becoming stuck.
What are the various risk factors of oral thrush?
Oral thrush can infect any individual; however, there are certain situations under which an individual becomes more prone to oral thrush infection, including:
- Certain medical conditions like cancer and HIV/AIDS affect the immunity of a person, thereby making the affected individual more prone to candida infection.
- Uncontrolled diabetes may harbor candida infection in the oral cavity, which occurs due to increased levels of sugar in the mouth.
- Individuals suffering from vaginal yeast infections become more prone to an oral thrush infection.
- Consuming certain medications like corticosteroids or antibiotics can disturb the oral microflora and cause oral thrush infection.
- People wearing dentures also become highly susceptible to oral thrush infection
What are the causes of oral thrush?
Typically, the body’s natural immune system functions well enough to maintain a balance between harmful and beneficial microorganisms in order to prevent the overgrowth of harmful microorganisms. However, in the event that the body’s natural immunity fails to protect against the increasing growth of candida fungus, the candida infection known as oral thrush can arise.
CANDIDIASIS, Causes, Signs and Symptoms, Diagnosis and Treatment.
How is oral thrush diagnosed?
Oral thrush can usually be diagnosed by a doctor based on an examination of the mouth or by examining a sample of a mouth lesion under a microscope. In some cases, certain blood tests are also carried out to check for the presence of any underlying health problems
If oral thrush has spread to the esophagus, the physician may perform any of the following tests:
- Biopsy - A biopsy for oral thrush will involve taking a swab from the back of the throat to obtain a sample that will be sent for culture in a microbiology lab. This test will allow the clinician to determine which bacteria or fungi are responsible for an underlying condition.
- Endoscopic Examination - An endoscopy may also be performed, which involves the use of a flexible tube with a camera at the tip (endoscope) that is passed down the esophagus while the patient is anesthetized to assess the esophagus, stomach and duodenum.
- Physical Examination - Specific physical or blood tests may be ordered by the treating clinician to determine any underlying condition that might be the cause of oral thrush in the esophagus.
How is oral thrush treated?
The primary aim of treating oral thrush is to limit the spread of the fungus; however, the best treatment modality may depend on age, overall health status, and the reason for candida infection. If the primary cause of the infection has been eliminated, the infection can be controlled.
In healthy adults, the physician usually recommends antifungal drugs, which may be prescribed in the form of lozenges, tablets, or in a liquid form for swishing followed by swallowing. Initially, topical medications are advised; however, if the condition does not go away, the treating clinician may recommend oral antifungal drugs. In adults with immunocompromised conditions, the physician will typically recommend antifungal drugs.
References
Further Reading
Last Updated: Mar 9, 2021