Scleroderma is a health condition that involves thickening of the skin and may also affect internal organs. This condition can be difficult to diagnose due to the fact that several other health conditions have similar characteristic features; therefore, the differential diagnosis of scleroderma is essential.
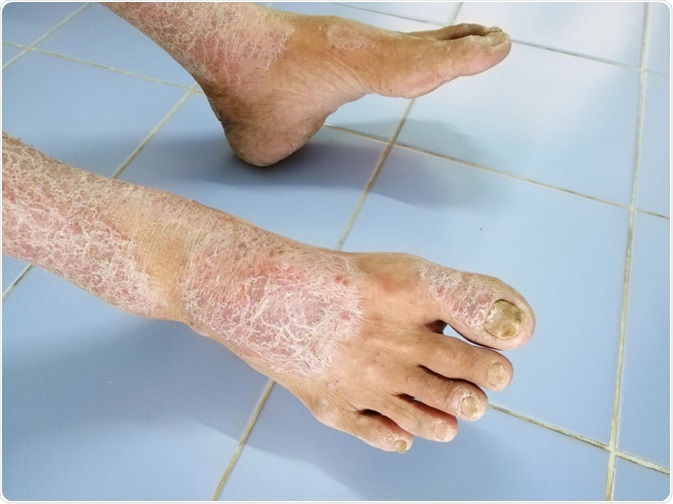
Image Credit: Numstocker / Shutterstock.com
Medical and family history
Upon initial presentation, a consultation with the patient is necessary to establish the previous medical history of the patient, indicative symptoms, and family history of the disease or other conditions.
It is important to understand the medical history of the individual to establish the risk that scleroderma may be involved. Past treatments of radiotherapy, for example, can increase the patient's risk of this condition. Additionally, there are some environmental triggers that may lead to the initiation of symptoms, such as exposure to silicon, radiation, and certain solvents.
Although there are currently no specific genes that have been identified to play a causative role in the development of scleroderma, there appears to be a genetic link, as the condition tends to run in families. For this reason, individuals with suspected scleroderma should be asked about any other family members who may have experienced similar symptoms.
Presenting signs and symptoms
The skin is the most common area of the body to be affected by scleroderma and is involved in all forms of the disease. Indicative signs of the condition include:
- Skin hardening
- Skin tightness
- Swelling or puffiness
- Sclerodactyly (skin induration)
- Hyperpigmentation or hypopigmentation changes of the skin
- Itching
- Raynaud’s phenomenon
- Nail-fold capillary changes
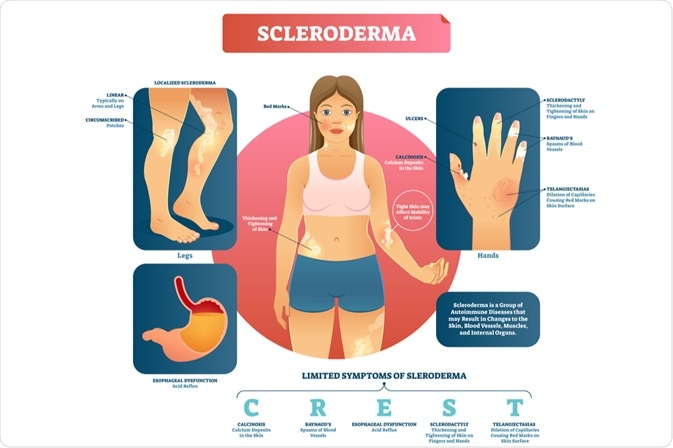
Image Credit: VectorMine / Shutterstock.com
In some cases, the involvement of other organs in the body may result in symptoms specific to the affected organs. This is known as systemic sclerosis and can lead to the following symptoms, according to which organs are involved.
- Vascular: Raynaud phenomenon, which is defined as reduced blood flow to extremities, is present in the majority of patients and may exist for several months or years before the clinical presentation of scleroderma.
- Gastrointestinal: Dyspepsia, gastroesophageal reflux disease (GERD), constipation, fecal incontinence, and malnutrition.
- Respiratory: Dyspnea (shortness of breath), chest pain, and persistent cough, all of which are usually associated with pulmonary hypertension.
- Musculoskeletal: Pain of the bones, joints, and muscles, as well as restricted joint movement and muscle weakness.
- Cardiac: Arrhythmias and congestive heart failure, which can be recognized by shortness of breath.
- Renal: Hypertension and renal insufficiency or crisis.
- Genitourinary: Erectile dysfunction, bladder fibrosis, and vaginal fibrosis.
- Eyes, ears, nose, and throat: Sicca syndrome, tooth changes, acid reflux resulting in hoarseness, and blindness.
- Neurologic/psychiatric: Pain, decreased sensation, headache, depression, and anxiety.
- Constitutional: Fatigue, loss of appetite, and weight loss.
Physical examination and tests
There is no single test for scleroderma that is able to effectively determine the involvement of the condition. Most patients present with symmetric thickening of the skin, and many are also affected by Raynaud’s phenomenon.
A skin biopsy of an affected area can be taken and tested in a laboratory setting for signs of scleroderma. These tests are able to identify anti-topoisomerase antibodies (e.g., anti-scl70) that are associated with the diffuse systemic form of the disease or anti-centromere antibodies, which are associated with the limited systemic form.
Differential diagnosis
The diagnosis of scleroderma can sometimes be confused with several other health conditions, including:
- Eosinophilia
- Eosinophilia-myalgia syndrome
- Eosinophilic fasciitis
- Graft-versus-host disease
- Mycosis fungoides
- Nephrogenic systemic fibrosis
- Primary biliary cirrhosis
- Primary pulmonary hypertension
- Complex regional pain syndrome
References
Further Reading
Last Updated: May 20, 2021