As the central part of the circulatory system, the heart is responsible for pumping blood, supplying oxygen and nutrients, and removing metabolic waste such as carbon dioxide from all the tissues in the body. The heart and a network of arteries and veins comprise the cardiovascular system.
The heart is a vital organ of the body; therefore, minute dysfunctions or abnormalities in the heart may have drastic consequences on human health. Typically, the heart is the size of an adult fist and is found enclosed in a pericardial sac at the chest's center, tilted to the left, and underneath the sternum in a thoracic compartment.
Image Credit: Explode / Shutterstock.com
How blood circulates in the heart
The heart consists of four chambers, four one-way valves, and a set of arteries and veins that regulate the normal flow of blood within the body.
The smooth functioning of the circulatory system is maintained by a complex network of blood vessels that circulate blood throughout the body and back to the heart. Whereas veins bring deoxygenated blood back into the heart, those that carry oxygenated blood away from the heart to other tissues in the body are known as arteries. The two exceptions to these are the pulmonary arteries and pulmonary veins, as well as the umbilical artery and vein.
The heart's two upper chambers are called the atria, with the atrial septum dividing the right and left atria. The superior and inferior vena cava are major veins that supply the right atrium with deoxygenated blood from the rest of the body.
The superior vena cava brings deoxygenated blood into the right atrium from the upper limbs and head, whereas deoxygenated blood from the lower abdomen and limbs is brought into the heart through the inferior vena cava.
The pulmonary veins supply oxygenated blood from the lungs into the left atrium and are the only veins in the body to carry oxygenated blood. However, during pregnancy, the umbilical vein carries oxygenated and nutrient-rich blood from the placenta to the fetus.
Both atria contract and release blood into the ventricles when full, a process controlled by the atrioventricular valves. The flow of deoxygenated blood from the right atrium into the right ventricle is regulated by the tricuspid valve, while the mitral valve controls the flow of oxygenated blood from the left atrium to the left ventricle.
The two lower chambers of the heart are called the ventricles. The right ventricle receives deoxygenated blood that collects in the right atrium. This process occurs by systematically opening and closing the atrioventricular and semilunar valves.
The semilunar valve connecting the right ventricle to the lungs is the pulmonary valve. This valve remains closed while the tricuspid valve opens and releases blood into the right ventricle from the right atrium.
Similarly, the left ventricle receives oxygenated blood from the left atrium through the mitral valve. During this process, the other semilunar valve, known as the aortic valve, remains closed to allow the left ventricle to fill with blood. The ventricles contract when full, subsequently causing the tricuspid and mitral valves to close and the pulmonary and aortic valves to open on the right and left sides, respectively.
When the right ventricle contracts, deoxygenated blood flows through the pulmonary valve into the lungs through the pulmonary trunk. The pulmonary trunk splits into the left and right pulmonary arteries, the only arteries in the body to carry deoxygenated blood. However, during pregnancy, the umbilical artery will also carry deoxygenated blood from the fetus to the placenta to re-oxygenate the fetal blood supply.
Oxygenated blood is pumped through the aortic valve into the aorta when the left ventricle contracts. The aortic valve splits into smaller arteries, known as common iliac arteries, which carry blood to the rest of the body through a complex network of arteries.
Structure of the heart
The heart wall is composed of three layers, including the outer epicardium (thin layer), middle myocardium (thick layer), and innermost endocardium (thin layer). The myocardium is made up of cardiac muscle fibers and is responsible for the contraction and relaxation that results in the pumping of the heart.
The two atria have a thinner myocardium layer than the ventricles, as the force required for atrial contractions is much less than that needed for ventricular contractions. The walls of the right ventricle are also thinner, as this ventricle only pumps blood a short distance to the lungs. Comparatively, the left ventricle, which has much thicker walls, must generate enough force to pump oxygenated blood throughout the rest of the body.
The myocardium requires a constant supply of oxygen and nutrients to maintain the contractions and relaxations that keep the heart pumping. This blood supply is maintained through a set of coronary arteries and veins in the myocardium.
The right and left coronary arteries, which branch off the first section of the aorta known as the ascending aorta between the left ventricle and aortic arch, supply blood to a network of capillaries in the myocardium. Deoxygenated blood from the myocardium is carried through a set of cardiac veins to the right atrium that is subsequently drained through the coronary sinus.
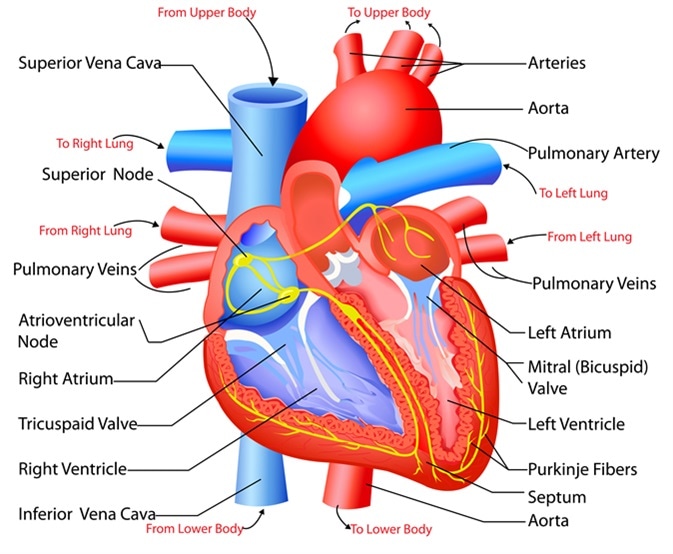
Easy to edit vector illustration of the anatomy of the heart. Image Credit: Snapgalleria / Shutterstock
What is a heartbeat?
On average, the heart beats 100,000 times a day and circulates about 5.6 liters of blood throughout the body three times a minute. The cardiac cycle, also known as the heartbeat, begins with deoxygenated blood collecting in the right atrium.
Simultaneously, the left atrium gets filled with oxygenated blood from the lungs. The sinoatrial node (SA node), located in the right atrium's superior wall, rhythmically initiates electrical impulses 70-80 times per minute to both atria. The SA node can be influenced by nerve impulses from the autoimmune nervous system and specific hormones, such as the thyroid hormone and epinephrine.
The SA node is often referred to as the heart's pacemaker, as it sets the rhythm of the heartbeat. Additional components of the heart's electrical conduction system include the atrioventricular node, bundle branches, atrioventricular bundle, and conduction myofibers known as Purkinje's fibers.
When full, the right and left atria contract together, thereby opening the atrioventricular valves and draining blood into the right and left ventricles, respectively. The electrical impulse from the SA node then proceeds through the His-Purkinje conduction system that stimulates the contraction of the ventricles.
Ventricular contraction pumps oxygenated blood from the left ventricle into the aorta and the rest of the body, whereas deoxygenated blood from the right ventricle into the lungs.
The contraction phase of the atria and ventricles is known as systole. Conversely, the relaxation phase is known as diastole. Systole and diastole constitute one cardiac cycle, which takes about 0.8 seconds at a normal heart rate.
The heart rate is the number of times the heart beats in one minute. A healthy adult's resting heart rate varies between 60 and 100 beats a minute. Children usually have higher heart rates. The heart rate is also affected by emotions, body temperature, and activity levels.
What is an arrhythmia?
An electrocardiogram (ECG) records electrical signals in the heart and is visualized in the form of several distinct waves. Cardiac disorders and cardiovascular diseases can be monitored using an ECG. Arrhythmia, or irregular heartbeat, occurs when the electrical signals that regulate the cardiac cycle are abnormal.
Ventricular tachycardia is an arrhythmia characterized by frequent, premature ventricular contractions and indicates underlying myocardial disease. This condition can lead to ventricular defibrillation, an immediately life-threatening form of arrhythmia believed to occur due to continuous and aberrant activation of the electric circuits of the ventricles.
Ventricular defibrillation is characterized by rapid and irregular activation of the ventricles that ultimately hinder effective ventricle contraction. The inability of the heart to pump blood out results in an instant drop in blood pressure, which could lead to death in the absence of immediate electrical defibrillation.
HCL Learning | Structure of the Human Heart
Cardiovascular diseases
Valve malformations and diseases result in a staggering amount of deaths each year. Stenosis, which is the obstructed outflow of blood and regurgitation or backward flow of blood due to defective closure of valves, are manifestations of valve diseases.
Heart sounds are caused by vibrations produced during the closure of valves. Abnormal heart sounds, or heart murmurs, indicate valve malfunctions.
The most common valve malformations include the bicuspid aortic valve and mitral valve prolapse. Valve disease can also occur through the degeneration of elastin, collagen, and proteoglycan layers of the extracellular matrix of the valves.
Coronary heart diseases (CHD) or ischemic heart diseases progress slowly. They are caused by atherosclerosis, or the buildup of fat, cholesterol, or calcium on the walls of the coronary arteries that supply blood to the heart. This results in a reduced supply of oxygenated blood to the heart. Pieces of these fat deposits can also break off, forming a blood clot that can block the coronary artery, cut off blood supply to the heart, and cause a heart attack.
Symptoms of CHD include chest pain, nausea, traveling pain through the limbs, and shortness of breath. High blood pressure, smoking, high cholesterol, diabetes, and obesity are risk factors for CHD.
References
Further Reading
Last Updated: Sep 4, 2022