Introduction
The role of twin and family-based studies
Genome-wide association studies (GWAS)
The relationship between age, genetics, and hypertension
Genetic base of hypertension
The future of genetic investigations in the context of hypertension
References
Further reading
Hypertension is a major modifiable risk factor for renal, cerebrovascular, and cardiovascular disease. The pathophysiology of hypertension, also known as high blood pressure, is complex, whereby both genetic and environmental factors interact with several physiological pathways and mechanisms to produce an observable phenotype.
 Image Credit: Chompoo Suriyo/Shutterstock
Image Credit: Chompoo Suriyo/Shutterstock
Epidemiological studies have improved our understanding of the environmental factors that influence hypertension, particularly the role of diet and exercise; however, the role of genetics in the context of hypertension has been a challenge to determine.
Studies of blood pressure data systematically acquired across three generations of the Framingham Heart Study (the first and long-term, ongoing cardiovascular cohort study of residents of the city of Framingham, Massachusetts) have revealed that higher blood pressure in both grandparents and parents is associated with the risk of the same condition appearing in the third generation.
This is particularly true when a family history of hypertension is documented to have been developed before the age of 55; this represents the strongest risk factor via potential in the subsequent generation. This effect occurs independently of a range of measured environmental factors known to influence the risk of hypertension – including sodium intake, alcohol intake, and level of physical activity.
The role of twin and family-based studies
Twin and family-based studies have shown that blood pressure is a heritable characteristic; between 30 and 50% of the variance in this parameter has been linked to heritability. Rare disorders outside of hypertension have also demonstrated a demonstrable role of Mendelian genetics.
However, when observing the distribution of blood pressure, a Gaussian distribution can be seen, which suggests that the mutations are unlikely to play a major role and that the multiple genetic effects (which are quantifiably small) either contribute to or enhance an individual susceptibility to hypertension.
Following advances in genomics, a more widespread opinion is that hypertension is a complex trait with a polygenic (controlled or influenced by several genes) basis. Moreover, environmental influences are also likely to influence epigenetic changes, which can be transmitted across generations.
 Image Credit: chayanuphol/Shutterstock
Image Credit: chayanuphol/Shutterstock
Genome-wide association studies (GWAS)
GWAS have been used to determine common genetic variants. The Wellcome Trust Case Control Consortium (WTCCC) was one of the first to embark upon this. bringing together over 50 research groups from the UK to explore complex human diseases of major public health importance— hypertension being amongst coronary artery disease, Crohn's disease, rheumatoid arthritis, types I and II diabetes, and bipolar disorder. Since then, more recent studies have been conducted, bringing the total number of variants associated with the risk of hypertension to 280. Moreover, these variants are associated with other diseases, such as coronary artery disease, a disease causally associated with the risk of high blood pressure.
The relationship between age, genetics, and hypertension
The premature onset of a condition is considered a genetically driven outcome rather than a result of environmental and lifestyle factors. Studies have shown that early-onset hypertension, occurring before the age of 55 years, is a great predictor of the risk of hypertension in subsequent generations. After the age of 55, systolic blood pressure is typically known to increase. In contrast, diastolic blood pressure is decreased - however, once over 55, this process is generally due to vascular aging, which is caused by stiffening of the arteries.
While family history does not provide information on this specific role of environmental or genetic effects that affect the risk of developing hypertension, to determine this, a more thorough investigation of the genome, as well as environmental exposure, is needed to identify the pathophysiological factors affecting the risk and their size.
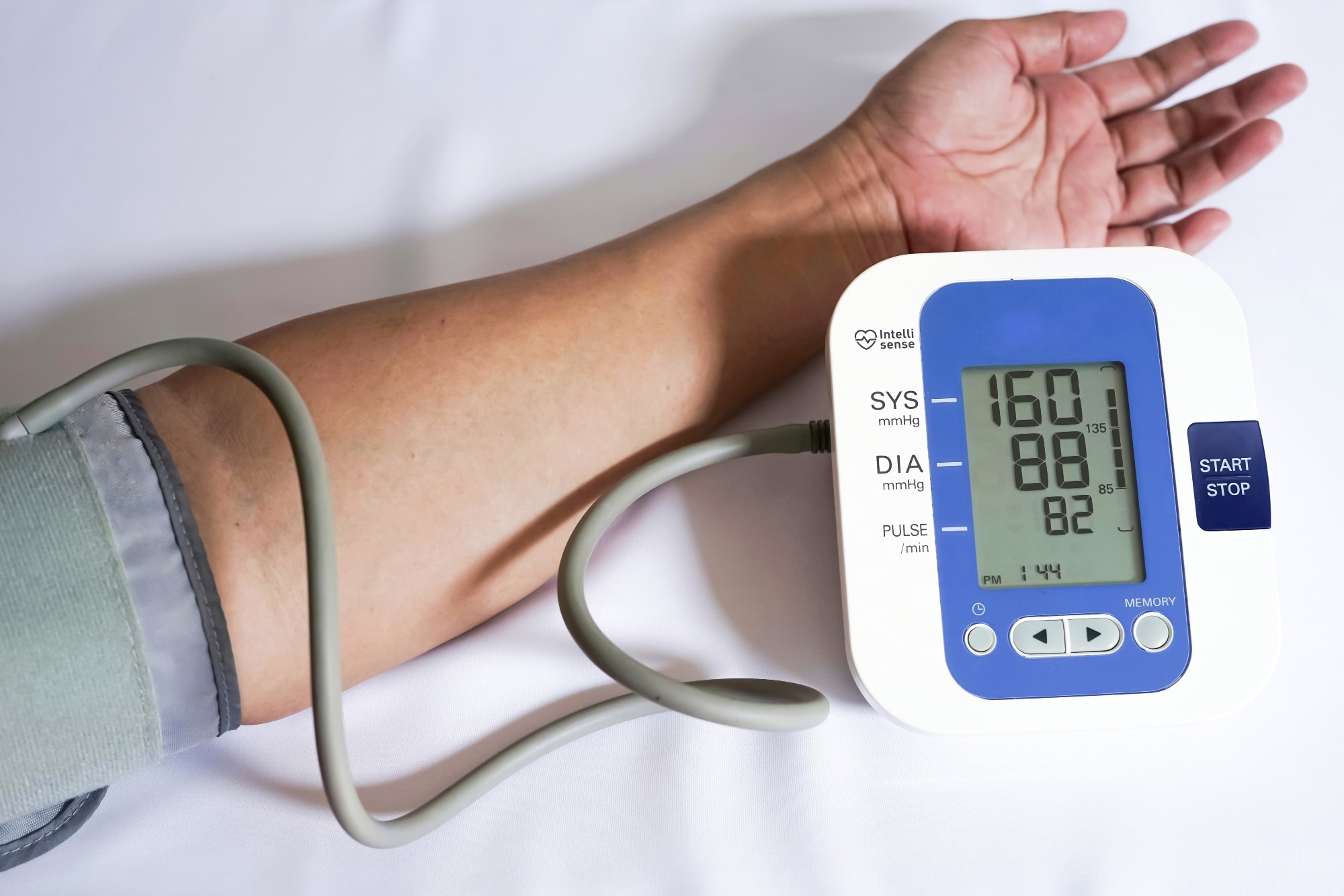 Image Credit: Adheamir/Shutterstock
Image Credit: Adheamir/Shutterstock
Genetic base of hypertension
By determining the known variants associated with an increased risk of hypertension and quantifying this using a genetic risk score, information related to individual susceptibility can be determined. Moreover, this could inform understanding of the pathways responsible for hypertension.
By understanding this, more effective prevention of hypertension and associated cardiovascular disease could occur based on the following:
- The identification of at-risk subjects before developing hypertension
- Implementing targeted and aggressive lifestyle interventions
- Providing more rational and targeted selections of drugs that are likely to be both safe and effective for an individual patient
These principles are associated with precision medicine, an approach based on identifying high-risk patients before symptoms show, with distinct mechanisms of disease, as well as an understanding of their likelihood of responding to particular treatments.
Both hypertension and heart disease are prevalent and have a sizable impact on life expectancy; if precision medicine initiatives are applied to them, this may lead to marked improvements in public health outcomes.
The future of genetic investigations in the context of hypertension
As precision medicine becomes popularised, early identification of patients at risk of hypertension in the preclinical phases of the disease could be possible. In addition, modifying the factors likely involved in the development of hypertension promises to determine both non-responders and toxic responders among patients before prescribing the medication. This way, only patients who are responders and not predisposed to toxicity are prescribed the appropriate medication.
References
- Mahmood SS, Levy D, Vasan RS, et al. (2014) The Framingham Heart Study and the epidemiology of cardiovascular disease: a historical perspective. Lancet. doi:10.1016/S0140-6736(13)61752-3.
- Patel RS, Masi S, Taddei S. (2017) Understanding the role of genetics in hypertension. Eur Heart J. doi:10.1093/eurheartj/ehx273.
- Magavern EF, Warren HR, Ng FL, et al. (2021) An Academic Clinician's Road Map to Hypertension Genomics: Recent Advances and Future Directions MMXX. Hypertension. doi:10.1161/HYPERTENSIONAHA.120.14535.
- Eales JM, Jiang X, Xu X, et al. (2021) Uncovering genetic mechanisms of hypertension through multi-omic analysis of the kidney. Nat Genet. doi:10.1038/s41588-021-00835-w.
Further Reading
Last Updated: Jan 16, 2023