Human babesiosis is an emerging tick-transmitted infection caused by protozoal hematotropic parasites that belong to the genus Babesia. Although this condition is rare, fatal outcomes have been described. For this reason, timely detection, adequate treatment, and prevention efforts are essential tools to control babesiosis.
The selection of treatment strategies largely depends on the species responsible for the infection, severity of the disease, as well as the underlying immune status of the affected individual. Individuals without any symptoms usually do not necessitate any treatment. Although there is no vaccine available to prevent human babesiosis, several other preventive measures are successfully used.
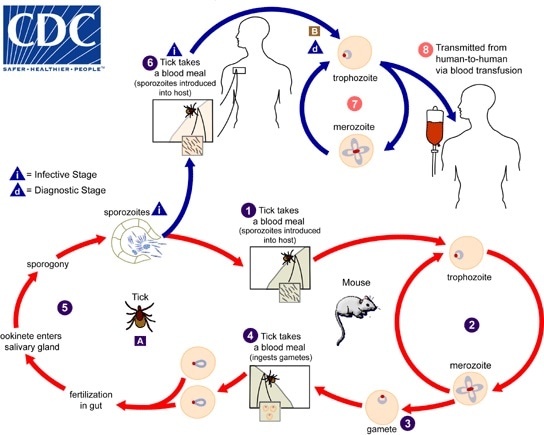
The Babesia microti life cycle involves - image and information courtesy of DPDx / CDC
Therapeutic Modalities
After the diagnosis of babesiosis is confirmed by the examination of thin blood smears under the microscope or by polymerase chain reaction (PCR), patients who exhibit symptomatic babesiosis are candidates for a course of antimicrobial treatment. Two commonly employed antimicrobial regimens show high effectiveness: the combination of atovaquone with azithromycin, and the combination of clindamycin with quinine.
Atovaquone and azithromycin are used for the treatment of immunocompetent patients facing mild to moderate babesiosis, while clindamycin and quinine are reserved for more severe infections. Significantly fewer adverse effects are seen in those treated with the combination of atovaquone and azithromycin when compared to those treated with clindamycin and quinine.
Adverse drug reactions can be seen in three-fourths of patients on clindamycin-quinine combination, with a third of them forced to decrease the dose or to end the treatment prematurely. Some adverse effects that are seen include decreased hearing, tinnitus, gastrointestinal symptoms, visual disturbances, headache, vertigo, and rash. On the other hand, only fifteen percent of patients treated with atovaquone and azithromycin experienced symptoms that were congruous with an adverse drug reaction.
Individuals with babesiosis should be strictly monitored during therapy. In a majority of cases, improvement occurs within a day or two after the treatment is instituted. Still, it must be noted that certain patients may have persistent low-grade parasitemia for several months after infection, and if the symptoms do not improve, the possibility of co-infection with Lyme disease or human granulocytic anaplasmosis should be suspected.
Whole blood or red cell exchange transfusion can produce a swift and a notable fall in parasitemia, thus its use as an adjunct treatment to chemotherapy should be considered in gravely ill patients with high parasitemia counts. Exchange transfusion can also rapidly correct anemia and remove toxic byproducts of babesia parasites.
Prevention Efforts
Preventive measures for tackling babesiosis vary, from avoiding exposure to ticks to the modification of habitat. Simple measures involve using tick-repellent chemicals on the skin before visiting a region known to be infested by ticks; minimization or complete avoidance of such areas; and meticulous skin examination after exposure.
Diverse public health policies have come into use to reduce the density of tick population in infested areas. This includes the spraying of acaricidal formulations, which is the most commonly employed method. It has been shown that applying such pesticides on the fur of animal reservoir hosts helps to break the cycle of transmission of Babesia parasites successfully.
In conclusion, the recognition of human infection with Babesia parasites will probably improve, as physicians (as well as the public) become more cognizant of this condition. The number of known cases is likely to go up as people recreate and live in rural tick-infested regions, and as the number of immunocompromised patients continues to increase.
Further Reading
Last Updated: Feb 26, 2019