Paraplegia can be caused by a range of both local and cerebral causes.
Paraplegic Definition, Explained, Causes, Recovery, Prognosis | Paraplegia | Spinal Cord Injury
Trauma to the spinal cord or brain
Most commonly, paraplegia is the result of accidents, which often occur in the young adult male population, between the ages of 15 and 35, that cause traumatic injury to the spinal cord. This accounts for more than 75% of all spinal injury cases.
Some of the different accidents that may cause paraplegia can include vehicle accidents, sports accidents, gunshot or stab wounds, or suicide attempts. Comparatively, workplace and household injuries are most commonly due to falls, diving accidents, electrocution, or blast injuries.
Other accidents resulting in paraplegia include:
- Spinal injections of toxins that damage the nerves
- Inflammation of the membranes surrounding the spinal nerves (arachnoiditis)
- Pathologic spinal fractures, such as those that occur in degenerative bone diseases
- Surgical accidents.
Types of spinal injuries
There are several different types of spinal injuries, which include hyperflexion, hyperflexion-rotation, vertical compression, hyperextension, extension-rotation, and lateral flexion spinal injuries.
Hyperflexion spinal injuries are typically caused by trauma to the back of the head or forceful decelerations. Comparatively hyperflexion-rotation spinal injuries are caused by disruption to the posterior spinous ligament.
Vertical compression spinal injuries, which can also be referred to as axial loading, arise when the vertebral body is compressed, resulting in a range of conditions from a reduction in the patient's height to complete fragmentation.
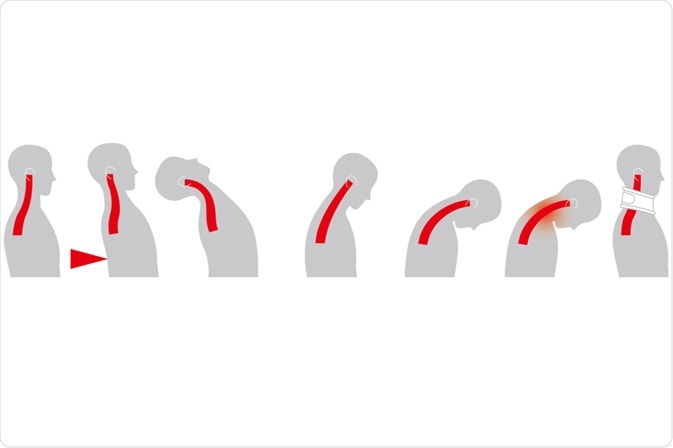
Image Credit: alphabe / Shutterstock.com
Hyperextension spinal injuries are often due to trauma to the front of the head or whiplash injury. Comparatively, extension-rotation spinal injuries occur when both the anterior and posterior spinal columns are disrupted, which can typically arise in diving injuries. The final type of spinal injury is described as lateral flexion and is often seen along with flexion or extension injuries.
In addition to spinal injuries, the different types of cerebral injuries that can lead to paraplegia include depressed skull fractures or subdural hematomas.
Medical
Infections in and around the spinal cord, such as abscesses, tuberculous abscesses, Pott’s disease, and parasitic infestations, such as schistosomiasis or bilharziasis, can also lead to paraplegia. In addition, vascular lesions, including spinal cord infarction, extradural hematomas of the spine, arteriovenous malformations, or aortic aneurysms have also been found to cause paraplegia.
Tumors, due to primary or secondary growths of the spine, including myeloma, neurofibromatosis, and neurilemmomas, as well as anesthetic accidents leading to spinal cord hypoxia, are all additional medical causes in which paraplegia is a potential complication.
Image Credit: Mortortion Films / Shutterstock.com
Another useful classification of the causes of paraplegia is as focal and systemic.
- Focal lesions
- Focal compressive lesions
- Vertebral compression
- Fracture or fracture-dislocation of vertebrae
- Pott’s disease
- Disc herniation
- Kyphoscoliosis
- Tumors
- Meningeal compression
- Intradural tumors, such as neurofibroma
- Extradural tumor deposits, as in leukemia
- Dural tumors, like meningiomas
- Cord compression, as in syringomyelia
- Focal inflammatory lesions, such as transverse myelitis.
- Vascular lesions, such as hematomas, infarcts, or hemangiomas of the spinal cord.
- Systemic lesions
- Hereditary
- Hereditary spastic paraplegia
- Hereditary ataxias, such as Friedrich’s ataxia
- Non-hereditary or nutritional
- Pellagra
- Subacute combined degeneration of the cord
- Idiopathic
- Motor neuron disease
- Disseminated disease, such as disseminated sclerosis
- Cerebral causes
- Affecting the cerebrum, in the parasagittal region, which regulates the voluntary movements of the lower limbs.
- Traumatic, as in subdural hematomas
- Inflammatory (i.e., meningoencephalitis)
- Vascular, as superior sagittal sinus thrombosis
- Tumors of the parasagittal region
- Degenerative, as in cerebral palsy
- Conditions affecting the brainstem
- Midline tumors
- Syringomyelia
Pathophysiology of acute spinal cord injury
Traumatic injury results from compression of the spinal cord against the neighboring bone-ligamentary complex. This leads to vascular injury, mainly of the tiny vessels inside the medulla of the bones, which produces hemorrhagic injury to the grey matter of the cord, as well as infarction due to spasm of the vessels.
The resulting fall in blood circulation inside the cord sets off the inflammatory cascade that leads to secondary injury by swelling, infarction, and permanent loss of function of the cord. In addition to the release of pro-inflammatory mediators, other mechanisms that lead to the loss of blood flow include failure of autoregulation, hypotension, thrombosis, and impaired energy production by the damaged and shocked cells, and vasospasm.
The eventual result of this chain of events includes loss of nerve conduction through the cord, membrane disruption, and the loss of structural integrity of the spinal cord.
References
Further Reading
Last Updated: May 16, 2021