Angular cheilitis, also called perleche or angular stomatitis, is a common inflammatory condition of the angles of the mouth. It is found in elderly edentulous patients as well as those who still retain their teeth, or wear dentures. While it may occur without obvious cause, it is often more common among patients with oral appliances of any sort, very young children, and those who wear masks for much of the time.
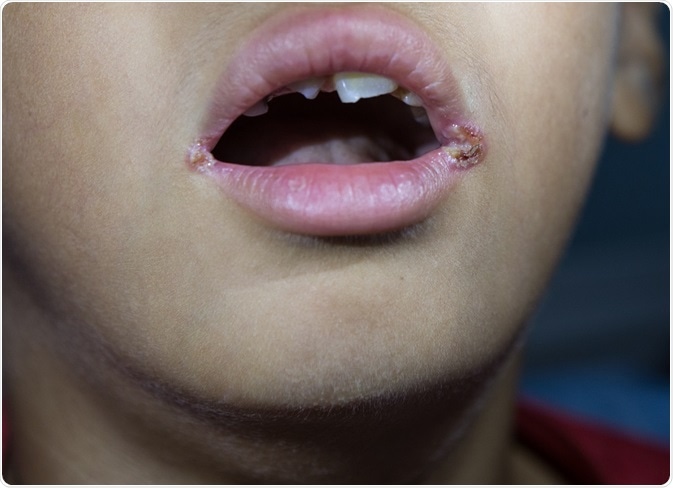
Credit: Karan Bunjean/ Shutterstock.com
Symptoms of angular cheilitis include pain, cracking of the skin around the angles of the lips, with redness and scaling, and occasionally bleeding or ulceration of the skin in this region.
Etiology
The etiology of this condition varies, with many patients showing evidence of infection with Candida albicans, Staphylococcus aureus and Streptococcal species. However, sterile cheilosis may also occur, due to overhanging upper lips, deep skin folds at the oral angles, poorly-fitting dentures, and dry skin.
Certain deficiencies in the diet, including those of iron, zinc and riboflavin, are also associated with a higher risk. Atopic children, especially those with cutaneous lesions in the form of eczema or seborrheic dermatitits, will often show perleche. Immunodeficiency due to HIV and Down syndrome are other risk factors. In short, multiple factors contribute to its incidence.
Diagnosis and management
Diagnosis of angular cheilitis is made on the basis of the history and clinical examination. The history should rule out other risk factors such as excessive flossing, badly-fitted dentures and medical causes. Some medical conditions may simulate angular cheilitis, such as herpes labialis and erosive lichen planus. Examination should be aimed at ruling out dental or gingival disorders as well, and detecting primary or secondary infection.
Staphylococcus aureus is present within the perleche lesions in many patients, and therefore swabs of the mouth as well as the anterior nares are essential. Surfaces of dentures may also be swabbed for bacterial culture.
Specific treatment is with antifungal, antibiotic and barrier creams in most cases. treatment of infection is key because of the prominent role of infectious agents in this condition. A 1% hydrocortisone cream is often combined with mupirocin in Staphylococcal infection, to counter infection and inflammation. Inhaled steroids may be used but the residual steroids should be rinsed out to prevent infection of the throat.
Systemic corticosteroids, systemic antifungals and antibiotics may be required in refractory lesions. In such patients a dermatologic consultation is often required to rule out other more serious conditions. In addition, blood testing is appropriate to rule out nutritional deficiency linked to cheilosis, including that of cobalamine, folate, iron and zinc.
Nutritional supplementation where necessary, replacement of dentures, and removing irritants within the oral cavity, such as sharp or broken teeth are other primary measures to promote healing of the lesions and to prevent recurrence. This is important as the rate of recurrence may be as high as 80%. The prolonged use of barrier ointments such as zinc oxide, and care in keeping the angles of the mouth dry, are both useful in reducing this rate.
Further Reading
Last Updated: May 27, 2019