Prolapse is a common medical condition that occurs when the structures designed to keep organs in place weaken or stretch, causing them to literally “fall out of place.” The term can be used to describe the misalignment of the valves of the heart (mitral valve prolapse), protrusion of the rectum (rectal prolapse), or even spinal disc herniation (lumbar disk prolapse).
Pelvic organ prolapse is a medical condition that arises when the normal support of the vagina is lost, resulting in the descent of one or more pelvic structures including the bladder, urethra, cervix, or vagina. The cause is multi-factorial, though primarily due to a loss of the support maintained by a complex interaction among the pelvic musculature, the vagina, and the connective tissue.
Mitral valve prolapse
Mitral valve prolapse can be defined as an abnormal bulging of the mitral valve leaflets into the left atrium during ventricular systole. The overall prognosis of patients with this condition is excellent, albeit a small subset can develop complications such as serious mitral regurgitation, arrhythmia, endocarditis, congestive heart failure, and cerebrovascular ischemic events.
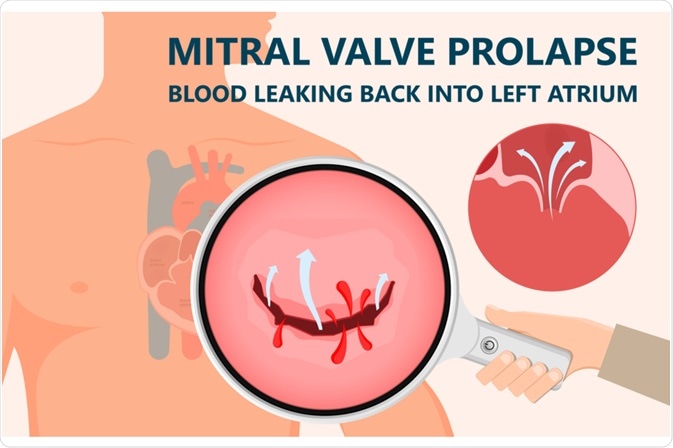
Image Credit: rumruay / Shutterstock.com
Myxomatous degeneration with genetic background is the most common cause of mitral prolapse. Echocardiography represents the method of choice for diagnosing mitral valve prolapse. Both clinical and echocardiographic features can predict which patients with prolapse are at the highest risk for developing complications.
Although the symptoms associated with this type of prolapse are often alleviated with beta-adrenergic blocking agents, there is no medication to correct or prevent the progression of valve prolapse. Therefore, surgical mitral valve repair using a variety of techniques is often the treatment of choice for symptomatic prolapse.
Rectal prolapse
Rectal prolapse (or procidentia) can be described as full-thickness protrusion of all layers of the rectum through the anal canal into the external environment. It is most commonly found in young children and elderly people and can be classified according to its severity. To this end, rectal prolapse can be classified as complete, mucosal, or internal (often termed occult) rectal prolapse.
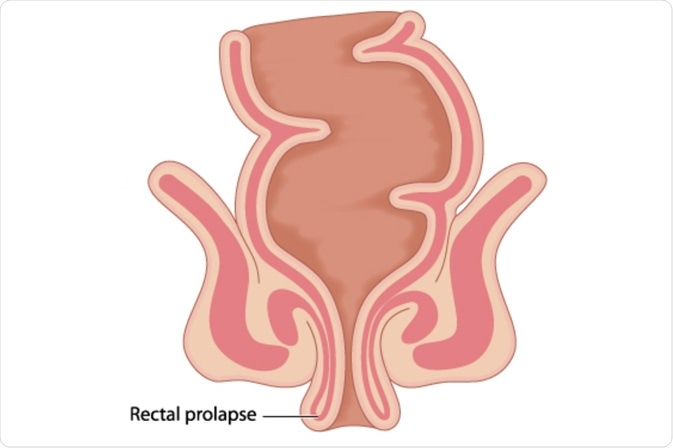
Image Credit: Blamb / Shutterstock.com
The precipitating factors in the development of this condition are not completely understood; however, they include often include poor bowel habits, sliding herniation of a deep pouch of Douglas, relaxation of the rectal suspensory ligaments, and rectal wall intussusception.
Patients with rectal prolapse frequently complain of bleeding, mucous drainage, incontinence, and sometimes even pain. The purpose of treatment for rectal prolapse is the correction of the prolapsed rectum and prevention of the postoperative defecation dysfunction, most often with a surgical approach. Notably, the surgical treatment for rectal prolapse is typically only contraindicated in cases of severe comorbidities.
Lumbar disk prolapse
Lumbar disc prolapse, which is also known as a slipped disc, accounts for less than 5% of all lower back problems but represents the most common cause of nerve root pain or sciatica. Pressure on one or several nerves that contribute to the sciatic nerve can result in lower back pain, as well as tingling, numbness, a “pins and needles” feeling, and muscle weakness in the lower body.
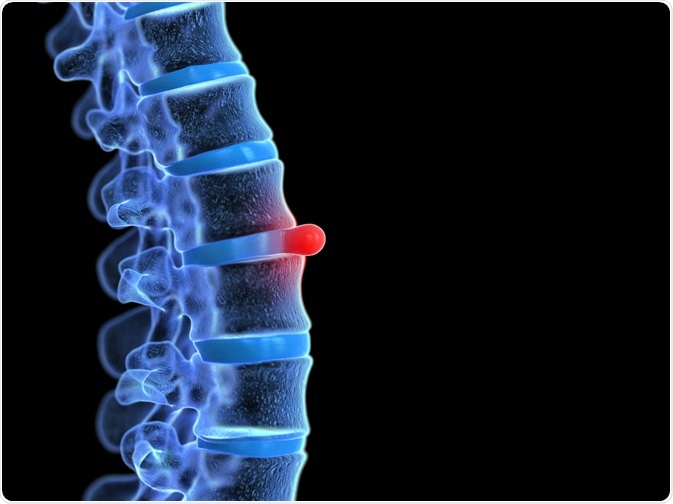
Image Credit: Sciepro / Shutterstock.com
Disc herniation occurs when the annulus fibrous breaks open or cracks, allowing the nucleus pulposus to escape. The intervertebral discs between relatively flexible lumbar vertebrae are particularly vulnerable to prolapse, as this region of the spine bears much of the body’s weight and supports a fairly wide range of motion.
In most instances, prolapsed disc symptoms can be managed through conservative or non-surgical treatments, such as pain medications, physical therapy, exercise, or rest. Surgery is pursued in order to provide more rapid relief of pain and disability in the minority of patients whose recovery is unacceptably slow.
References
Further Reading
Last Updated: Feb 16, 2023