Research into the mechanisms of early brain development, especially that of the cortex, is important in aiding our understanding of how the brain develops so that we can also understand how neurodevelopmental and neuropsychiatric disorders occur.
Studying human brain development in vivo is incredibly difficult, as is studying the development of most mammalian organisms. Therefore, newer techniques are required to study aspects of the developing cortex using human cell models. Here, only mechanistic insights into the developing cortex will be discussed.
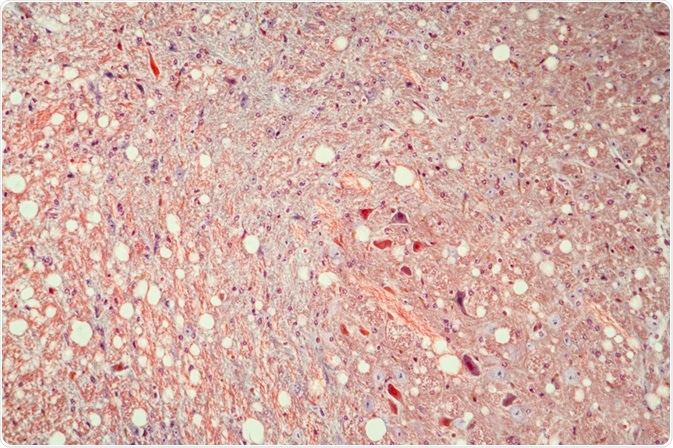 Image Credit: Dr. Norbert Lange / Shutterstock.com
Image Credit: Dr. Norbert Lange / Shutterstock.com
The Development of the Human Cortex
The vertebrate brain starts off as a sheet of epithelial cells called the neuroepithelium, or neural plate. The neural plate begins to fold in on itself to form the neural tube, which extends across the developing embryo.
The neural tube undergoes expansions at specific sites to form the developing brain at the front, and the spinal cord towards the back. At the front, the neural tube is patterned meticulously to form the forebrain, midbrain, hindbrain, and cerebellum. It is within the forebrain that the cortex forms as well as other specialized structures. The entire process is governed by different genes interacting with one another.
The cortex is the specialized part of the evolved forebrain that makes mammals different from the rest of the animal kingdom. The cortex is the most evolved in humans compared to other non-human primates. In humans, the cortex has 5 layers.
In development, these are structured as the ventricular zone (VZ), the inner subventricular zone (ISVZ), the outer subventricular zone (OSVZ), the intermediate zone (IZ) and the cortical plate (CP) at the top.
The cortical plate is much expanded in humans and higher-order mammals and begins to fold in itself forming gyri and sulci. All neurons arise from neural stem cells called radial glia. Radial glia have long processes that span the entirety of the developing cortical length (bottom to top) and allow a structural scaffold for developing neurons to migrate upwards.
Whilst studying many aspects of neuroscience in rodent models is possible due to the similarities to humans in cell types, structure, and function, studying the developing cortex is not entirely accurate as mice have key differences in the development of the cortex and its structure. Mice and rats do not have gyri and sulci and are therefore the brain is much less expanded.
Secondly, mice do not have an OSVZ as higher-order mammals do. In humans, further neural stem cells can be found in the OSVZ called basal radial glia, which are not found in most other mammals. To study the developing human cortex, human cells are needed to define the intricacies of cortical development that is different to most other mammals.
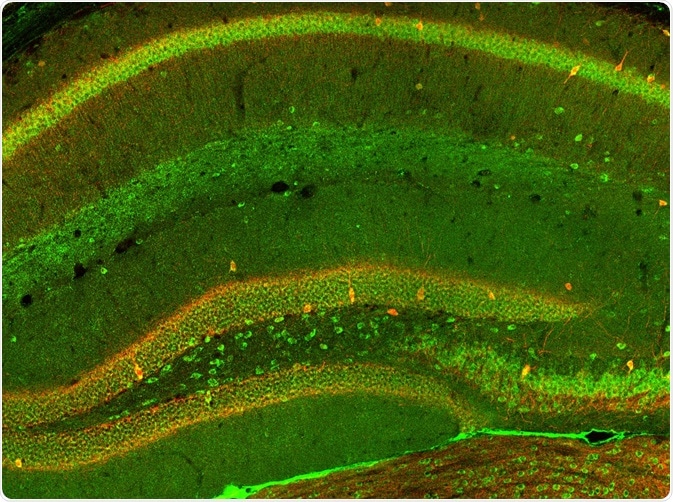 Image Credit: Alexandros A Lavdas / Shutterstock.com
Image Credit: Alexandros A Lavdas / Shutterstock.com
Human Cell Models of the Cerebral Cortex
Advances in human-derived cell model technology has greatly simplified studying specific cell types and complex structures in vitro in much less time than what was previously achievable. The simplest way of studying the developing cortex is that of cultured neural stem cells (2D).
These are extremely homogeneous but very simple. Increasing the size and complexity of cultured cells to form neural rosettes (3D structures) further increases complexity, but contains a heterogeneous diversity of cell types. Further complex structures include spheroids, forebrain spheroids, and cerebral organoids, which are the most complex and contain the most diverse population of cell types, structures, and properties.
Human derived progenitor stem cells can be made into cortical rosettes by SMAD inhibition and the addition of retinoids to drive this lineage in around 12 days. FGF2 signaling can drive the emergence of early-born deep layer glutamatergic neurons by 20 days, and between 50-100 days mature upper layer neurons and astrocytes can be found around the cortical rosette.
This 3D structure contains a diverse population of cortical neurons and astrocytes, and the time frame of development in vitro roughly matches that of in vivo development.
The increasing complexity of 3D in vitro structures can only be made possible with the addition of Matrigel (as a scaffold mimicking radial glial processes) as well as the application of a cocktail of growth factors and serum.
These inductive signals allow for patterning of developing structures, rather than a mixture of different cell types with no intrinsic patterning of structure that mimics in vivo localization. These organoids can reach up to 4mm in diameter and contain fluid-filled cavities that resemble actual ventricles, which are not seen in rosettes that only contain small tube-like lumens.
Organoids can also contain an OSVZ, not seen in in vivo models with the correct localisation and polarity (e.g. basal to apical). All of this can be achieved between 30-44 days depending on the protocol and specificity of the organoid.
For example, forebrain organoids require Nodal and Act growth factors, but TGFb and WNT inhibition. Cerebellar organoids, on the other hand, require Nodal, Act, and TGFb inhibition, but FGF2, FGF19 and SDF1 stimulation. These organoids can be made from embryonic stem cells or induced pluripotent stem cells.
3D organoids require more sophisticated tissue culture techniques and equipment. Unlike regular 2D cell cultures or rosettes, organoids require increased oxygen exchange. By culturing in a high oxygen environment of at least 40%, 3D organoids can be generated and maintained for long periods of time.
Though these models are by far the most complex, they have their own technical issues including the presence of non-neural cell types due to incomplete induction, as well as issues with reproducibility due to the self-assembly of mini-structures within each organoid.
The future looks bright for neurological organoid research
At present, we do not have a complete neurovascular organoid make up with different neural and non-neural cell types interacting with one another, as this is (for now) extremely technically challenging.
This is a big limitation of any 3D structure that does not have any vascular cells and a functional blood supply (or a fluid mimic). Tissue engineering advances have allowed synthetic vascular mimics to be effectively used as scaffolds in such cultures.
Over time, with advances in science and technology, more complex and ‘truer’ organoids could be formed to be used not only for understanding developmental processes, but also for the applications of disease modeling and drug discovery. This is certainly an exciting field of research bringing together scientists and engineers in doing what was previously impossible to achieve.
Further Reading
Last Updated: Oct 17, 2019