The intestine is an amazing organ in multiple ways, not least of which is its capacity to heal itself even when it is injured or damaged. Finally, a study by researchers at Dana-Farber Cancer Institute, published in the journal Cell Stem Cell shows how intestinal stem cells keep their number constant to renew the intestinal lining as and when it is required.
Intestinal cell turnover
The intestine is among three body tissues with a constant cell turnover – cells are dying, and freshly generated cells are taking their place. These tissues have the common property of being brought in contact with the environment most often, which puts them at risk of harm from potential toxins. The fast turnover is an escape route for these tissues to avoid the accumulation of multiple harmful effects that could be passed on to future generations of cells.
Intestinal stem cells
Intestinal stem cells (ISCs) are found deep in the finger-like 'inpouchings' of the intestinal lining called the intestinal crypts. These stem cells give rise to a large pool of billions of daughter cells that change over time into the type that builds and rebuilds the intestinal lining. And even if the stem cells themselves undergo damage, they are replaced from a self-renewing pool within a week.
However, ISCs are very radiosensitive, and exposure to high levels of radiation can knock out most of them for a time. Thus, individuals who have been exposed to nuclear fallout often suffer severe damage to the intestinal tissues because there are too few ISCs to make good the loss of intestinal lining cells.
On the other hand, ISCs also bounce back from such damage very fast. Thus, if the severely ill patients with intestinal damage from radiation can be kept alive for a week, the ISC count comes back to normal.
Some scientists thought that there might be a reserve of ISCs within the intestine, like a backup for the backup. This would mean that there was also a fresh supply of cells to replenish those that were lost from the area of trauma.
Other researchers postulate a more involved mechanism, where the ISCs generate not just more stem cells but the intestinal lining cells. On the other hand, if the ISC' mother cells' are themselves damaged, the specialized daughter cells enter a de-differentiation pathway. These then again become immature-appearing stem cells capable of regenerating whatever cells are needed and replacing the lost ISCs.
Intestinal stem cells. Image Credit: Sam Ogden
De-differentiation of daughter cells
The recent study lends support to the latter hypothesis for ISC self-renewal. The scientists found that both the ISCs and the daughter cells they produce have a markedly responsive association. When the ISCs are healthy, they differentiate into daughter cells. if the ISCs are being lost, the daughter cells turn back in their lifecycle to become ISCs again.
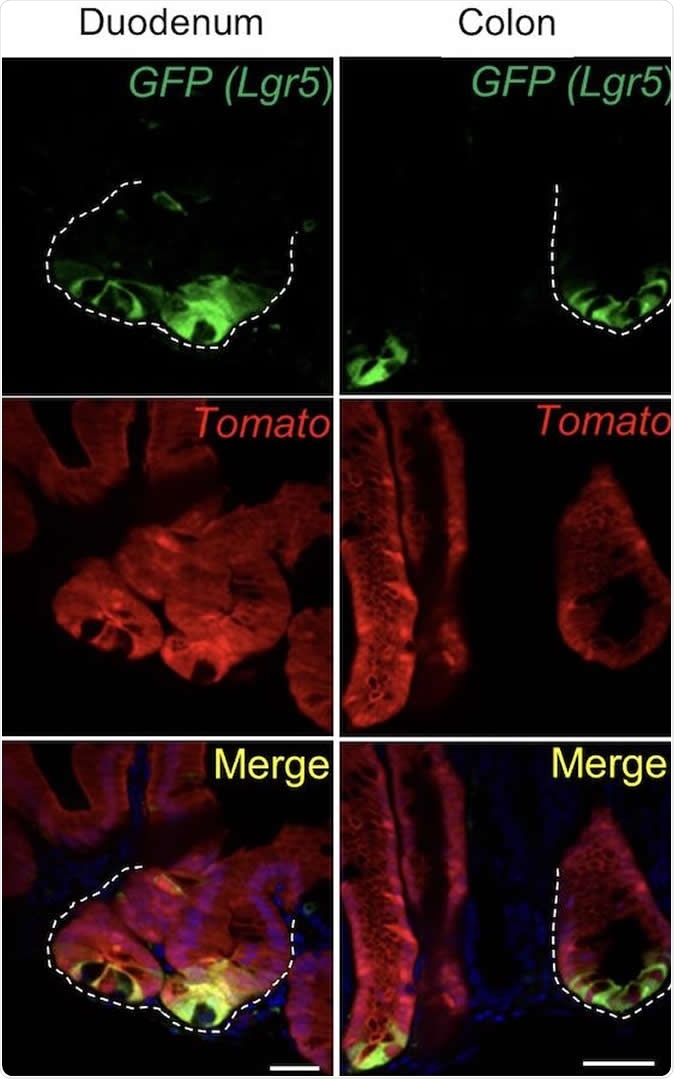
The researchers were able to prove that this happens. They treated a set of ISCs with the drug tamoxifen, which induced fluorescence in them as well as in any daughter cells they produced. After incubating the drug for 48 hours, to allow the drug to have its full effect, they then killed the ISCs so that any fluorescent ISCs picked up after that would be the de-differentiated daughter cells produced from this initial ISC collection. They succeeded in finding fluorescent ISCs.
The mechanism of ISC replenishment
This is not the first time that de-differentiation of mature cells has been observed: it has been seen to occur in many kinds of mature differentiated cells using laboratory techniques. However, the importance of this finding is that it proves this capability is not just a chance property, but the very key to stem cell restoration and renewal after damage.
In other words, according to senior author Ramesh Shivdasani, "Our findings suggest that the restoration of intestinal stem cells occurs entirely by the process of de-differentiation. We showed there's no need for a reserve set of ISCs."
The current experiment was able to show this happening in real-time. This is because cells that are beginning to de-differentiate switch on a particular gene, which is the key to permitting laboratory isolation and collection of these cells. This allowed the scientists to pick out cells that are losing their mature characteristics, from along the continuous path.
Scientists will now look into whether this property is common to mature cells in other organs and tissues. Another area open for research is how the crypt senses the death of ISC cells so that they need to be replaced, and how the daughter cells get the signal to de-differentiate. The investigators now plan to examine this question.
Journal reference:
Ascl2-Dependent Cell Dedifferentiation Drives Regeneration of Ablated Intestinal Stem Cells Murata, Kazutaka et al. Cell Stem Cell, https://www.cell.com/cell-stem-cell/fulltext/S1934-5909(19)30569-7