Researchers in Scotland who have evaluated a “stratify-and shield” policy for combating coronavirus disease 2019 (COVID-19) in the UK say it is time to consider the approach as an alternative to social distancing seriously.

Glasgow / Scotland - April 04 2020: Glasgow City Centre Buchanan Street Empty During Coronavirus Covid 19 Lockdown. Image Credit: Mo and Paul / Shutterstock
The strategy would involve protecting elderly and high-risk individuals from infection while allowing exposure and immunity to grow among low-risk individuals until most of the population is protected.
“It is time to give serious consideration to a stratify-and-shield policy that could bring the COVID-19 epidemic to an end in a matter of months while restoring economic activity, avoiding overload of critical care services, and limiting mortality,” says Paul McKeigue and Helen Colhoun from the University of Edinburgh.
A pre-print version of the paper is available in MedRxiv, while the article undergoes peer review.
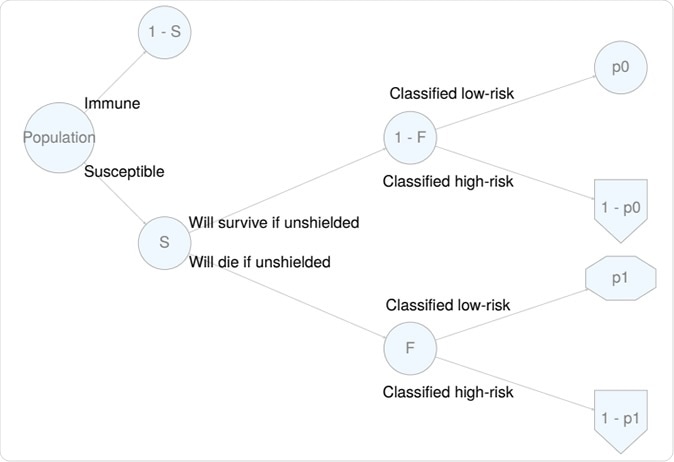
Probability tree for a stratify-and-shield policy
The different approaches
The researchers say the epidemic will only pass if the population’s immunity reached a level where the reproduction number (number of secondary infection cases arising from one original case) dropped to below 1, either as a result of natural immunity or immunization.
Although lockdown has slowed the spread of COVID-19, many experts in disease modeling agree that to keep the strain on critical care services at a manageable level, alternating periods of more and less strict social distancing measures would be needed until a vaccine has been made available.
However, an effective vaccine is not expected to be available for at least one year.
Concerns over the economic and social impact of the alternating lockdown measures taken in the meantime have led investigators to consider other approaches to managing the epidemic.
One alternative that has been suggested is imposing more intense measures on high-risk individuals while allowing low-risk individuals to be exposed to infection until the bulk of the population has developed immunity. The idea would be to protect against any second wave of SARS-CoV-2, once the epidemic has passed while relieving the strain on the NHS.
Investigating the theoretical dependencies of the policy
Now, McKeigue and Colhoun have evaluated the effectiveness of the policy at minimizing the mortality rate if social distancing rules were to be relaxed. The approach would use a classifier based on data from medical records to assign risk levels to people to determine who and who should not be shielded.
“We do not advocate a particular course of action,” writes the team… “but instead investigate the theoretical dependencies of the stratify-and-shield approach, its possible impact on mortality and workload for the health service, and discuss how to resolve some of the key uncertainties upon which the effectiveness of such an approach depends.”
The analysis found that the proportion of the population that would be shielded under the policy would be no more than 15%. However, even if a classifier based on data from medical records performed only slightly better than one based on age and gender alone, it should be possible to refer at least 80% of those who would die without shielding to the shielding group.
The importance of the population-wide fatality ratio
The average risk of infection among shielded individuals and the overall number of deaths while shielding is implemented would completely depend on the fatality ratio across the entire population.
“Although the proportion of deaths that would be prevented by effective shielding does not vary much with the infection fatality ratio, the absolute number of deaths in the unshielded varies from less than 10,000 if the infection fatality rate is 0.1% to more than 50,000 if the infection fatality rate is as high as 0.4%,” writes the team.
If the ratio were at the higher end of the values now considered viable (0.4%), even a well-performing classifier would be unable to ensure deaths would be kept to less than 30,000 or to keep the risk of death among unshielded people to lower than 1 in 2000, although this would still be manageable by expanded critical care services
However, the researchers note that the mortality risk predictions for unshielded individuals are averaged across the group and that a risk classifier “could, of course, output not simply a dichotomous classification, but a continuous risk score that would be the basis for individual choice.”
“Any shielding strategy involves issues of ethics and equity in that those in the unshielded group are asked to accept a low risk so that not just they, but those shielded from infection, can emerge from isolation sooner,” write McKeigue and Colhoun.
The team says researchers currently conducting studies that should help to answer important questions about applying the stratify-and-shield approach. Areas of uncertainty include the prevalence of immunity, the degree to which infection results in immunity, the fatality ratio, and how a classifier based on medical history performs.
“This policy option should not be dismissed”
The researchers say the time has come to seriously consider a stratify-and-shield policy that could hasten the ending of the COVID-19 epidemic.
“A stratify-and-shield policy using a classifier based on medical records has the potential to save lives, restore economic activity and end the epidemic long before a vaccine is expected to be available,” they write. “This policy option should not be dismissed but seriously evaluated as an alternative to adaptive social distancing.”
Important Notice
medRxiv publishes preliminary scientific reports that are not peer-reviewed and, therefore, not be regarded as conclusive, guide clinical practice/health-related behavior, or treated as established information.