A leg ulcer can be understood as a break in the skin, typically located on the feet or the lower part of the leg.
Leg ulcers are generally diagnosed based on their appearance, though this can be challenging because the appearance of leg ulcers is highly variable. If an area of skin breaks down to reveal the underlying flesh, there is a risk of a leg ulcer developing.
The most common types of leg ulcers are venous ulcers. NHS statistics highlight that these account for approximately 80% of all leg ulcers, with the condition affecting as many as 1 in 50 older adults. These types of very painful leg ulcers typically occur slightly above the ankle.
The standard NHS treatment for venous ulcers involves a routine cleaning and dressing procedure with compression. This treatment is performed in the community, typically over an extended timeframe.
NHS referral pathways can be lengthy, with it typically taking some time before patients can access a vascular specialist.
There is often a degree of inconsistency in terms of referring patients with leg ulcers for assessment of their veins, despite the importance of rapidly addressing the underlying cause of this condition. Failure to do so can lead to healing being delayed and a high recurrence rate.
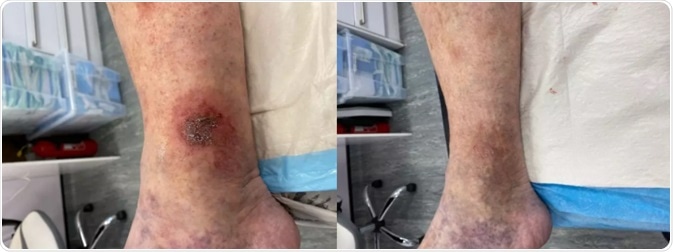
Image Credit: Veincentre
Veincentre has close to 20 years of experience in the treatment of venous leg ulcers, focusing on the application of endovenous laser ablation (EVLA) and foam sclerotherapy - methods that typically facilitate quicker healing, longer-lasting results and reduced recurrence versus traditional methods like compression bandaging alone.
Symptoms of leg ulcers
Venous leg ulcers are effectively open sores. These are generally found on the lower leg and can be slow-healing and painful.
A number of common symptoms may manifest in relation to a venous leg ulcer, including varicose eczema, varicose veins, swollen ankles, legs that feel heavy or achy or potentially even discolouration or hardening of the skin. There may also be a foul-smelling discharge from the ulcer in some instances.
These symptoms may be worse when the patient is standing or sitting. This is because the effects of venous insufficiency are more severe when the leg is below the heart.
In contrast, patients able to rest lying down or with the ulcerous leg elevated will find their symptoms lessening. This is because gravity works in line with the body to transport the patient’s blood back to their heart.
Causes of leg ulcers
Leg ulcers are caused by increased blood pressure, which often stems from poor circulation in the leg veins. As a result, the leg’s skin will become gradually damaged and fragile due to the consistently high pressure – this is known as ‘venous hypertension.’
Venous hypertension is typically the result of a valve failure such as venous incompetence, the most common cause of varicose veins. Due to this link, most patients with leg ulcers also have current or historical issues with varicose veins.
Venous hypertension may also lead to additional complications, including skin discolouration, eczema and ultimately ulceration.
It has been reported that venous ulcers account for over 75% of all leg ulcers. Arterial leg ulcers account for 15% of all cases - these tend to develop from similar problems in arteries as opposed to veins.
Venous ulcers represent the most straightforward and easy ulcers to treat and cure. An ultrasound scan will typically be deployed to ascertain the underlying cause, potentially even a mixture of venous and arterial insufficiency.
Diagnosing leg ulcers
Leg ulcers are easily identifiable due to their obvious nature as sores on the skin of the lower leg. Conventional diagnosis tends to involve an assessment of the patient’s symptoms and a cursory examination of the area of concern.
Assessment and examination may be completed while the patient is either standing or lying down. Visible varicose veins are typically easier to identify whilst standing, though it is simpler to identify and take a pulse in the ankles whilst the patient is lying down.
Veincentre’s approach involves an investigation into any underlying issues that may be causing leg ulcers and the use of a colour duplex ultrasound scan to demonstrate reflux and confirm that an ulcer is venous.
Preventing leg ulcers
While leg ulcers do present early signs, these may not always be recognisable. There may be evidence of discoloured skin on the lower leg, with the skin potentially turning into a brown patch on the inside of the area. Without proper treatment, this brown patch may darken and ultimately become ulcerated.
GPs and other medical professionals have historically recommended a combination of compression bandaging and/or compression stockings to encourage better circulation within the affected area. This helps improve blood flow from the feet to the heart.
Compression therapy remains a core element of the management of venous ulcers. It is recommended that this be augmented with the ablation of any underlying superficial venous reflux.
The most effective approach to preventing the development and recurrence of venous leg ulcers continues to be to treat the underlying cause using EVLA.
In the majority of cases, once an ulcer has been treated with EVLA and healed, it is no longer necessary to wear compression stockings. This effective treatment, therefore, means that a patient can resume their daily activities as soon as the site of the ulcer has healed.
Optimum treatment options
Veincentre’s treatment pathway for leg ulcers is much like the company’s treatment pathway for varicose veins.
Leg ulcer treatment commences with a duplex ultrasound scan - typically performed during an initial consultation - to determine the ulcer’s underlying cause and the extent of this. The results of this scan will inform the most appropriate course of treatment for that patient and their specific circumstances.
Early endovenous radiofrequency ablation (EVRA) is another effective means of treating leg ulcers, with a recent UK-based EVRA trial published in the influential New England Journal of Medicine1 supporting Veincentre’s approach of addressing this issue as early as possible.
The trial was the first of its kind to show that “early endovenous ablation of superficial venous reflux resulted in faster healing of venous leg ulcers and more time free from ulcers than deferred endovenous ablation.”
An earlier study2 highlighted that the conventional combination of surgically correcting superficial venous reflux and applying compression bandaging had no impact on ulcer healing, but this did lower the chances of ulcer recurrence at 4 years, leading to increased time without ulcers.
It is important to note that this earlier research demonstrated that surgical correction of venous insufficiency was able to reduce recurrence, but the associated lack of improvement in ulcer healing had a serious adverse impact on the overall treatment of venous leg ulcers.
Home remedies
People believed to be at risk of developing venous ulcers are advised to make a range of lifestyle changes to help avert or delay their onset. These include taking regular exercise, maintaining a healthy diet and ensuring they get enough sleep.
These changes may also lead to weight loss which can help improve blood flow in both arteries and veins.
Smokers are advised to quit smoking to reduce the strain on their cardiovascular systems, further improving circulation.
It is important to seek a medical opinion upon developing leg ulcers. If these ulcers are found to be venous in origin, then a combination of compression bandages and referral for a venous scan is necessary to address any superficial venous reflux.
Upon healing of the ulcer, it is advantageous to wear compression stockings to help limit leg swelling by assisting the blood flow to the heart.
Legs should be kept elevated while sitting, maintaining the position of the legs above the heart by popping the legs up on a cushion or pillow. This is important to encourage blood flow out of the leg and prevent pooling.
Aftercare for leg ulcer treatment
Following leg ulcer treatment via EVLA, it is advisable to continue to wear a simple dressing and compression stocking. It is then important to continue to use the dressings or bandages provided until the ulcer is fully healed.
References
- A Randomized Trial of Early Endovenous Ablation in Venous Ulceration. May 31, 2018 N Engl J Med 2018; 378:2105-2114. DOI: 10.1056/NEJMoa1801214 (https://www.nejm.org/doi/full/10.1056/nejmoa1801214)
- “Long term results of compression therapy alone versus compression plus surgery in chronic venous ulceration (ESCHAR): randomised controlled trial. BMJ. 2007 Jul 14;335(7610):83. doi: 10.1136/bmj.39216.542442.BE. Epub 2007 Jun 1.” (https://www.bmj.com/content/335/7610/83)
About Veincentre
 Veincentre are the UK’s leading varicose veins specialists using Gold Standard, minimally invasive techniques, with 15 clinics nationwide.
Veincentre are the UK’s leading varicose veins specialists using Gold Standard, minimally invasive techniques, with 15 clinics nationwide.
At Veincentre, we provide the most effective, proven treatment and the highest quality of care that is accessible to everyone. We treat the cause, not just the symptoms! All our treatments are minimally invasive – walk-in, walk-out, require no general anaesthetic, no surgery and no time off work.
The most important aspect of care for any condition is the ability and attitude of the team of doctors and nurses looking after you. We have headhunted some of the most experienced and respected vein specialists in the UK. By choosing Veincentre, you can be assured that discomfort will be minimised, outcomes will be optimised, and you will be looked after by a team who really care for you
From your initial point of contact you will be communicating with our patient advisers, who only deal with patients who suffer from varicose veins so are all highly experienced and can confidently answer all of your queries or provide any advice.
Start your journey to healthy veins and happy legs…
Sponsored Content Policy: News-Medical.net publishes articles and related content that may be derived from sources where we have existing commercial relationships, provided such content adds value to the core editorial ethos of News-Medical.Net which is to educate and inform site visitors interested in medical research, science, medical devices and treatments.