Sleeve gastrectomy is a surgical procedure that is used to remove around 90% of the stomach, so that the capacity of the stomach decreases to around 100 to 200mL. This reduces the amount of food a person can eat in one sitting, thereby ensuring they feel full after consuming just a small portion of food. In addition, cells in the stomach produce the appetite-stimulating hormone ghrelin and removing a large portion of the stomach results in less of this hormone being made.
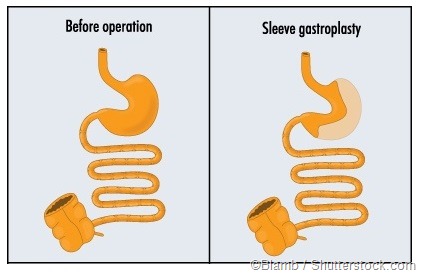
The complications associated with sleeve gastrectomy are rare; however, when they do occur they are more serious than those associated with other weight loss strategies such as gastric banding. If a leak develops, for example, resolving the problem can take months. Another disadvantage is that sleeve gastrectomy is a relatively new procedure and there is a paucity of long-term data on how successful weight loss via this procedure is over time.
As is the case with any operation, sleeve gastrectomy is associated with a number of risks and, although rare, the following describes some of the complications that can occur.
Bleeding
If post-operative bleeding occurs, which happens in approximately 0.5% of cases, a blood transfusion may be required.
Infection
Infection may occur, in which case antibiotics and sometimes repeated surgery are needed. Wound infection is more common in people with a higher body mass index.
Leaks at the staple line
This happens in about 1% of cases and can be life threatening. A leak can require repeated surgery and a persistent leak can lead to a fistula forming or recurring infection within the abdomen. A leak can result in a patient having to stay in hospital for weeks or even months after surgery.
Inability to tolerate food intake
This is extremely rare, but since sleeve gastrectomy affects digestive function, some individuals find they are unable to tolerate an adequate food intake. This can mean they need nutrients administered intravenously on a long-term basis.
Organ damage
Accidental injury to organs near to the operation site is always a risk in keyhole surgery and if it occurs, further surgery may be required to correct any damage to organs.
Deep Vein Thrombosis
Blood clots in the veins or lungs are also a potential risk.
Long-term complications
Any intra-abdominal surgery involving the gastrointestinal tract may be complicated by the formation of scar tissue in the gut or a hernia forming as a result of wound sealing, both of which could mean further surgery is needed.
There is also a risk of gastroesophageal reflux disease developing post-operatively, which may mean patients need to take antacids. Sleeve gastrectomy is not performed when patients have presented with serious symptoms of this condition.
Occasionally, patients have problems absorbing nutrients after the surgery and, in such cases, supplements and blood test monitoring are required.
Post-Operative Problems Associated With The Gastric Sleeve
Further Reading
Last Updated: Feb 27, 2019