Cracked heels refers to a condition produced by the occurrence of fissures in abnormally hard, dry skin over the heels of the feet. If left untreated, they may cause complications and discomfort.
In this condition, the skin around the heels is unusually thick and dry, and is known as the callus. When weight is put on the heel, the normal fat pad underlying the skin flattens out sideways to distribute the pressure more equally. However, this causes the skin to crack if it is too dry and thick.
If the fissures run very deep, standing can be painful. It may also develop into cellulitis, a spreading infection of the skin.
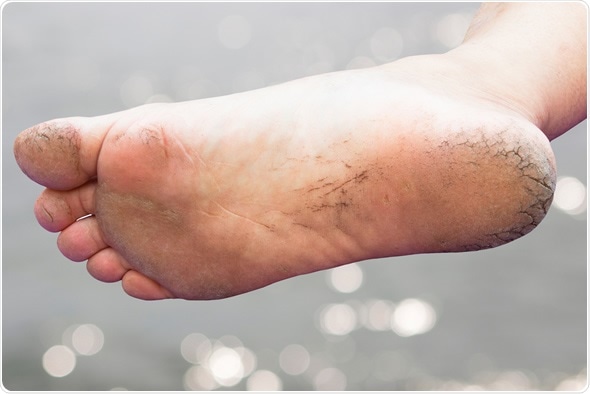
Cracked Heels - Copyright: Kriengsuk Prasroetsung / Shutterstock
Causes of cracked heels
Some patients have skin that tends towards dryness while other people may encourage the appearance of cracked heels by their style of walking. Some other triggering factors are described below.
Prolonged standing
When a person often stands for a very long time on a hard floor, it may contribute to the development of cracked heels.
This risk may be minimized by the use of footwear which is properly padded in the heel and sole areas to provide extra support.
Conversely, thin-soled shoes may make the problem worse. Also, being overweight may encourage the symptoms as increased body weight increases the pressure on the normal fat cushion under the heel of the foot.
Eczema or atopic dermatitis
This itchy skin condition can increase skin dryness and make the heels more susceptible to cracks.
Treatment includes using moisturisers on the skin, as well as the use of steroids and antibiotics if indicated, under the supervision of your healthcare provider.
Psoriasis
This disease is characterized by dry scaly and flaking skin, and can develop in different places on the body, including the feet. If you notice that your skin is peeling or scaling, ask your healthcare provider to advise you on how to treat it.
Palmoplantar keratoderma
This disease causes thickening of the skin on the palms of the hands and soles of the feet and predisposes to fissure formation.
Juvenile plantar dermatosis
Children with this condition experience high levels of moisture on the skin over their feet, followed by quick drying. Repeated wet-dry cycles lead to cracks developing on the soles of the feet.
Systemic conditions
Some systemic conditions may precipitate or aggravate cracked heels. Diabetes patients have to be mindful of the risk of foot ulcers developing from the cracks in the skin.
Autonomic neuropathy is another complication of diabetes which can affect sweating and lead to increased dryness of the skin. Hypothyroidism, or the presence of an underactive thyroid, may also contribute to dry skin.
Inappropriate footwear
Shoes without a proper back, and open sandals, as well as similar types of footwear, can cause or worsen cracked heels as there is little to keep the fatty pad in the heel of the foot in place when pressure is exerted on it.
This leads to increased lateral bulging of the fatty tissue and enhances the pressure on the dry thickened skin at the sides of the heel.
Treatment
A person who has dry skin over the heels should regularly buff the area using a pumice stone or something similar, to exfoliate dead skin and thus reduce the thickness of the cornified epithelium.
The next step is to moisturize daily with oil-based moisturizers. Moisturizers may contain keratolytics to remove dead skin, or water-retaining substances such as urea, to restore moisture to the skin.
Such patients should avoid the regular or prolonged use of thin-soled shoes or footwear that does not provide proper support to the heel fat pad.
Any complications such as cellulitis must be promptly treated with antibiotics, debridement of any necrotic tissue, and keeping the affected foot raised to encourage proper circulation and healing.
Diabetics should take care to acquire shoes or other footwear which are comfortable, adjustable to one’s individual measurements, allow free passage of air through the material, and which allow for enough space.
References:
Further Reading
Last Updated: Feb 26, 2019