Testicular cancer or germ cell cancer is a rare type of cancer affecting approximately 6 in 100,000 men each year. It can be cured completely by surgically removing the affected testicle.
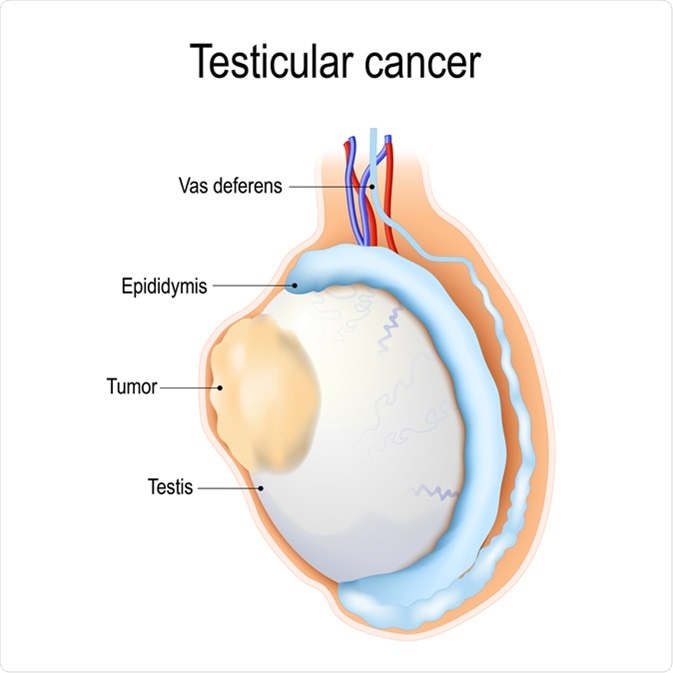
Testicular cancer. Tumor develops in the testicles. Image Credit: Designua / Shutterstock
How testicular cancer affects the psychology of a person?
After being diagnosed with testicular cancer, men usually develop a sense of fear and undergo stress, anxiety, anger, and depression. These emotional changes subsequently reduce the sexual performance and fertility. Moreover, cancer-related hormonal changes also cause a temporary infertility. Such condition can bring a sense of guilt and uncertainty to the affected person.
The changes in life that occur due to intense and long-term treatment regimen also bring a feeling of overwhelmed. New compromises that an affected person has to make are often very difficult to deal with.
How to discuss cancer-related issues with your partner?
There is no better alternative than a healthy communication between couples to overcome the problems and concerns related to testicular cancer. Being the partner of a cancer survivor, you can be the most valuable support for your partner’s physical and emotional well-being.
If you are the primary caregiver, you may also undergo strong emotional changes. In such situations, the most important thing to remember is that your stress can be the cause of primary distress of your partner who is already going through the tough phases of cancer. Thus, a good communication is always necessary for both of you to improve the quality of life.
Before beginning a conversation with your partner, your primary responsibility is to educate yourself about the physiology of testicular cancer and its treatments. If your partner is concerned about treatment-related reduction in sperm count and infertility, suggest him about preserving sperms in a sperm bank before starting the treatment. He can also opt for radiation shielding to reduce the risk of radiation-induced sperm DNA damage, although this is not possible in all cases. In this process, a lead shield is used to cover and protect the unaffected testicle from the radiation.
If there is a temporary loss of fertility due to surgical removal of one testicle, assure your partner that his fertility will resume within 2 years after the completion of chemotherapy or radiotherapy. In case both testicles are removed, testosterone replacement therapy can be helpful for maintaining the sexual performance. Encourage your partner to discuss with his healthcare provider about the best possible form of hormone therapy.
Encourage your partner to adopt a healthy lifestyle, such as quit smoking, avoid alcohol, and perform physical activity regularly. These changes will help your partner better cope with cancer- and treatment-related changes in the body.
In most of the cases, men usually detect the presence of lumps in the testicle by themselves. The fear of having cancer often prevents the men from consulting a doctor. In such cases, your primary duty is to explain to him that testicular cancer is highly curable if diagnosed and treated promptly.
Testicular ultrasound is generally performed to detect the position and nature of lumps (solid or fluid-filled). In some cases, blood tests are also done to determine the level of tumor biomarkers. Once diagnosed, doctors recommend removing the affected testicle and analyzing the lump to determine the type and stage of the cancer. This is particularly important for determining the type of treatment you need and the prognosis.
About Testicular Cancer Symptoms & Treatment
In most of the cases, testicular cancer is cured completely after successful completion of the treatment. However, a cancer survivor is always worried about possible cancer relapse. In this regard, regular follow-up checkups are very important for proper management of the cancer. During follow-ups, regular lab tests and imaging tests are done to check the presence of cancer-related symptoms and treatment side-effects. Explain to your partner that follow-up checkups are essential to keep an eye on cancer progression. This is particularly needed for early detection of cancer recurrence and timely initiation of appropriate treatment.
Further Reading
Last Updated: May 7, 2019