The herpes simplex virus (HSV) is a common virus that causes episodes of small, fluid-filled blisters on the mouth, lips, skin, eyes, and/or genitals.
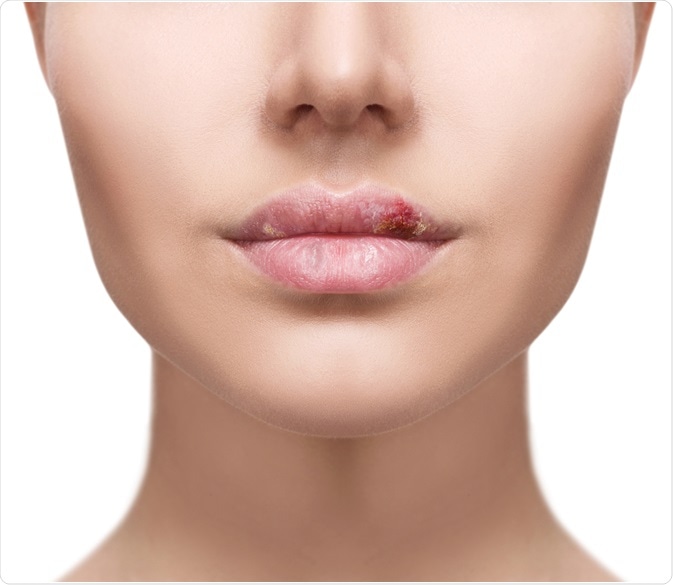
Image Credit: Kotin / Shutterstock.com
How is HSV spread?
HSV is a very contagious infection that can be spread through skin-to-skin or sexual contact with an individual who is infected with the virus. HSV can also be spread through direct contact with the blister, which allows the virus to access the body, or through contact with the affected area, even when no blisters are present. Genital herpes is primarily spread through sexual contact.
It is less likely that sharing towels, utensils, and cutlery carries a risk of transmission, as the virus dies quickly once it is outside of the body. However, avoiding contact with such items is advised if a person is known to be having an outbreak of symptoms.
After the initial infection, HSV lies dormant in the body and may be reactivated later, sometimes several times a year. HSV cannot be cured; however, the use of certain antiviral drugs can ease symptoms and help reduce the risk of infection to others.
HSV types
There are two types of HSV, including:
- HSV-1: This form of HSV usually causes cold sores on the lips, which is referred to as herpes labialis, as well as blisters on the cornea of the eye, which is referred to as herpes simplex keratitis. HSV-1 can also be spread to the genital area through oral sex.
- HSV-2: This form of HSV usually causes genital herpes and is spread through both skin-to-skin contact and sexual contact. HSV-2 is highly contagious whether sores are present or not. Recurrence is much more common with HSV-2 as compared with HSV-1.
The lesion often seen in both types of HSV contains a clear fluid in which the infective viral particles are present. The body develops antibodies to the HSV within weeks after acquiring the infection, and these antibodies can be detected on laboratory investigations. In a person who has transmitted oral HSV-1 infection, antibodies may take around 6 weeks to develop.
Pathophysiology
Both HSV-1 and HSV-2 typically access the body through the genital or oral mucosa. From here, the virus then replicatse in the stratified squamous epithelium, where it is then taken up by ramifying unmyelinated sensory nerve fibers.
Next, HSV undergoes retrograde microtubule-associated transport to the neuronal cell bodies in the dorsal root ganglia (DRG) near the spinal cord, where acute infection is followed by lifelong latent infection. The virus remains in a dormant state within this collection of nerve cells. Periodically, the virus becomes reactivated and travels through anterograde microtubule-associated transport back into the stratified squamous epithelium of skin or mucosa, where replication occurs and the virus is shed into genital or oral secretions.
Herpes (oral & genital) - causes, symptoms, diagnosis, treatment, pathology
The cycle of HSV infection is controlled by the immune system on several levels. Upon entering the body, innate and adaptive immune processes regulate the degree of replication that takes place in the mucosa. This determines how much of the virus accesses the DRG, becomes latent and then becomes reactivated.
At the DRG level, latency and reactivation is subject to immune control. After the virus has been transported to the axon terminals, the level of replication is determined by an adaptive immune mechanism at the interface with epithelial cells in the mucosa. This also determines whether clinical disease or asymptomatic shedding takes place.
Reactivation and recurrence can occur many times and can be triggered by various factors including fever, stress, menstruation, and/or immune suppression. Physical trauma such as excess exposure of the lips to the sun or a dental procedure can also trigger the development of cold sores. However, in most cases, the trigger is not known.
In nearly half of individuals infected with HSV who do not exhibit symptoms, shedding of the virus can occur more than a week before or after symptoms present. In addition, if other infections are present, the risk of transmission in the absence of overt symptoms remains higher.
References
Further Reading
Last Updated: Sep 27, 2025