Impetigo is a bacterial skin infection. It initially presents as blisters on the skin near the nose and mouth of the baby, before spreading to other body parts. The size of the blisters varies depending on the type of Impetigo the baby has contracted. Smaller blisters burst quickly to form sores, while larger ones burst after a few days.
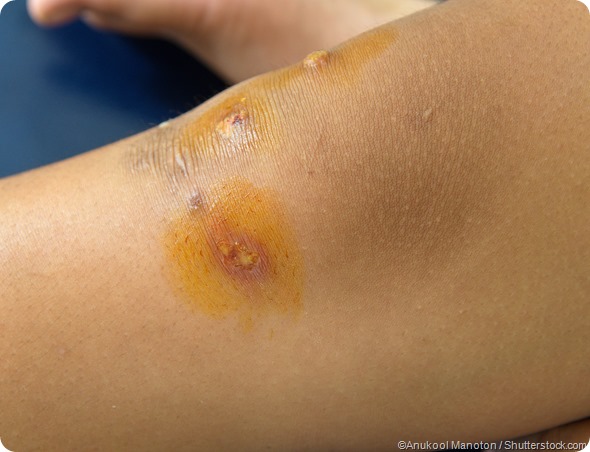
Impetigo is extremely contagious and spreads quickly between children, earning the name ‘school sores’ for this very reason. Coin-shaped sores are left on the skin after the blisters burst. These get covered by a yellowish-brown scab, which take a while to heal, but normally do not leave a scar behind.
Cause of impetigo
The skin disease is caused by Staphylococcus or Streptococcus bacteria, both of which are commonly found bacterial species that spread quickly in warm climates. They are often present on the skin, throat or nose of the baby without causing any issues.
It is rare for healthy skin to develop the bacterial infection. However if the skin has a scratch, cut, bite or disease like eczema or chicken pox, the bacteria may flare up and cause the Impetigo infection. The incubation period for the infection is 4-10 days after exposure to the bacteria.
Types of impetigo
The two types of Impetigo are bullous and non-bullous. Both are caused by a bacterial infection, but each manifests on the body differently.
Symptoms of non-bullous impetigo
Blisters usually start close to the mouth or nose before they spread to limbs and other body parts.
Blisters burst, leaving a red, wet patch of skin called a sore.
The skin of the sore oozes fluid for a while before a soft and yellowish brown crust develops.
The crust will form a scab and heal in roughly three days. Some peeling of the scab may take place at the edges during healing.
Once the sore is healed, there is no scar left behind as long as the baby has not been allowed to scratch the sore.
Symptoms of bullous impetigo
The bullae (fluid-filled blisters) are almost 2cm in size, larger than those in a non-bullous impetigo infection.
The blisters appear on the torso of the baby first, usually between the neck and the waist before eventually spreading to the limbs and rest of the body. The blisters may be painful and take a longer time to burst than is usual. The skin around the blisters tends to itch so the baby must be prevented from scratching them.
Fever and swollen lymph glands in the neck are more likely to occur in Bullous Impetigo. In addition, the scabs take longer to heal.
Treating impetigo in babies
The baby’s skin will need an antibiotic ointment applied to it daily. It is equally important to maintain basic hygiene by using warm water and gentle cleansers every day. If the infection is severe, an oral course of antibiotics may also be prescribed by the doctor.
Mild cases may clear up in 2-3 weeks without medication. However it is better to medicate the baby as the duration of the illness reduces to 7-10 days and considerably eases their suffering if appropriate ointments are used.
Importantly, if the infection is left untreated, it may result in complications such as a worse skin disease called cellulitis. Rarely, in some cases, it could develop into psoriasis, septicaemia, scarlet fever and even a kidney disorder known as glomerulonephritis. These complications are very rare.
Preventing the spread of impetigo
Precautions which may curb the spread of this bacterial skin infection include the following:
- Don’t allow the baby to scratch the sores as this will spread the infection to other parts of the skin.
- The blister is infectious as long as fluid is oozing out of it. Minimize skin contact with the fluid and infected skin.
- Hands of the baby and caregiver should frequently be washed with warm water and soap.
- Cover the oozing sores with a dressing and bandage to prevent bacterial spread.
- Use an antibiotic soap for bathing the baby and pat all the blisters dry with a disposable paper napkin.
- Change and disinfect the bed linen, towels and clothes of the baby daily while the infection lasts.
- Wash the toys the baby plays with in a disinfecting solution.
- Minimise contact between the baby and other children in the house to ensure the infection is not contracted by those unaffected.
References
- http://www.nhs.uk/conditions/impetigo/pages/introduction.aspx
- http://www.babycentre.co.uk/a548384/impetigo
- https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/impetigo-school-sores
- http://www.rch.org.au/kidsinfo/fact_sheets/impetigo_school_sores/
- https://www.seattlechildrens.org/
Further Reading
Last Updated: Jan 1, 2023