One of the main functions of protein C is to prevent blood clotting by inactivating proteins that encourage blood clotting. Deficiencies in protein C are associated with higher risks of developing blood clots known as deep vein thrombosis. A deep vein thrombosis occur in deep veins in limbs, but can move via the bloodstream and get stuck in more critical areas, such as in the lungs.
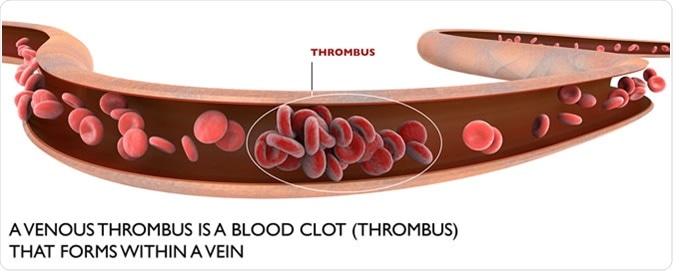
Deep vein thrombosis, a blood clot within a vein. Image Credit: Naeblys / Shutterstock
The issue
Protein C deficiency can range from mild to severe. The majority of people with mild deficiency do not progress to dangerous blood clots, but several factors can combine with the deficiency to increase the risk. These include age, medical procedures, inactivity, and pregnancy. An additional blood clotting disorder can also increase the chance of dangerous blood clotting. Symptoms of deep vein thrombosis include pain in arms or legs, swelling, bruised skin, and warmness. A deep vein thrombosis that has reached the lungs is called a pulmonary embolism, which is associated with difficulty breathing, chest pain, rapid heartbeat, and coughing up blood.
Acute cases of protein C deficiency are associated with development of a condition called purpura fulminans not long after birth. In this very dangerous condition, blood clots form in small blood vessels throughout the body, which blocks normal blood flow and can cause localized tissue destruction known as necrosis. Because the clotting absorbs all available blood clotting proteins, there can be excessive bleeding in other parts of the body. This can lead to excessive bruising.
Causes of protein C deficiency
Protein C deficiency is an inherited condition and is inherited in an autosomal dominant pattern. When only one copy of the mutated gene is present, the individual tends to have mild protein C deficiency, whereas two mutant gene copies results in severe deficiency. The gene whose mutation causes protein C deficiency is the PROC gene, which produces protein C. Most of the mutations target the amino acid sequence, resulting in a disruption in protein C’s ability to control blood clotting. Protein C deficiency can be subdivided into type I and II based on how the PROC mutations affect protein C. In type I, overall levels of protein C are decreased. In type II, protein C is produced but in an altered state which reduces activity. Both can be associated with mild or severe deficiency symptoms.
Protein C deficiency can also be caused by non-genetic factors. For example, it can be caused by deficiencies in vitamin K, which is needed to activate protein C. In such cases, levels of protein C are normal but because vitamin K cannot activate it, protein C remains in its inactivated state.
Protein C deficiency can also be acquired. Protein C is produced in the liver, so patients with liver failure may show signs of protein C deficiency. Other conditions that can cause deficiencies include use of the blood thinner warfarin, widespread metastatic tumors, severe illness (such as sepsis), and disseminated intravascular coagulation.
Treatments and other conditions
Protein C deficiency is usually treated with anticoagulants, which thin the blood. They counteract the deficiency by preventing blood clot formation and will prevent clots from growing, but the medication will not remove the clots that have already formed. Anticoagulants can be administered intravenously or orally.
Protein C deficiency is not a common condition, but the outlook is positive for most that are diagnosed because most people do not have noticeable side effects. Clotting can be relatively easily managed and prevented by maintaining a healthy diet and exercising, in addition to taking medication.
Protein C deficiencies can have serious complications for pregnancies. There is a higher risk of developing blood clots both during and after pregnancy, because pregnancy is also a risk factor for developing abnormal clots. Some research also suggests that protein C deficiencies can increase the risk of miscarriages in early and late pregnancy terms.
Further Reading
Last Updated: Apr 8, 2019