Rheumatoid arthritis (RA) is believed to be caused by a combination of genetic susceptibility and environmental factors. In many cases, presenting individuals will have a number of these factors that are all likely to contribute to the development of the disease.
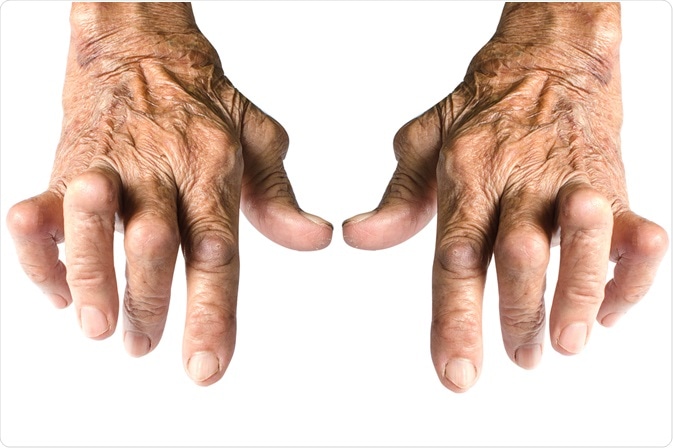
Image Credit: Chaowalit Seeneha / Shutterstock
Inherited Genetic Susceptibility
Initially, it was observed that patients with a family history of rheumatoid arthritis were more likely to be affected by the condition, suggesting a familial link.
Since the introduction of more advanced technology, several genes have been identified that are thought to be associated with an increased risk of developing rheumatoid arthritis. In fact, it is believed that several genetic markers often contribute to each case of the condition.
The HLA-DRB1 gene is the most predominant genetic risk factor for the development of rheumatoid arthritis. There are many variants of the gene and several of these are linked to an increased risk of the disease. Additionally, the protein tyrosine phosphatase 22 (PTPN22) gene is also linked to a higher risk of developing rheumatoid arthritis, although it is unclear how this occurs.
However, it is believed that there are many more genetic markers that have not yet been identified that, with further research, could lead to a more complete understanding of the disease and initiate targeted treatment and prevention strategies.
Hormonal Factors
Rheumatoid arthritis is more common in women than in men, and the disease tends to go into remission during pregnancy, suggesting that hormonal factors may play a role in the presentation and regulation of the disease. One hormone that may be involved in causing rheumatoid arthritis includes prolactin, which is responsible for the production of milk and enhances inflammation.
Additionally, the incidence of rheumatoid arthritis in young women who have taken the oral contraceptive pill is approximately half that of those who have never taken the pill.
Health Conditions
It was long believed that some infection was likely to cause rheumatoid arthritis but after much unfruitful research it appears to be clear that there is no single infection or agent that causes the disease. However, many presenting cases have recently had an infection of some sort and it is believed that the immune response to several different types of infection may result in arthritis symptoms.
In rare cases, immunization can trigger rheumatoid arthritis, which is thought to result from the controlled infection administered via the vaccination.
Rheumatoid arthritis is also more common in people who are already affected by an autoimmune disease, which is likely due to the similarity in the pathology of the conditions.
Smoking
A history of smoking is a considerable risk factor for the development of rheumatoid arthritis, and it can also affect the course or progression of the disease.
Many smokers with rheumatoid arthritis find it difficult to stop as it can help to reduce related symptoms, such as joint tenderness and pain. However, patients that continue to smoke are at risk of extra-articular disease where also the nodules, lungs or blood vessels may be affected.
Diet
There is also some evidence that certain foods or diets can impact the likelihood of being affected by the disease. For example, people with diets that have a high proportion of red meat and low vitamin C and vitamin A content are at an increased risk of developing rheumatoid arthritis.
References
Further Reading
Last Updated: Mar 11, 2023