Folliculitis decalvans (FD) is a condition in which there is loss of hair in a patchy fashion over the scalp, due to a chronic inflammation with scarring. The first description was by Quinquaud in the 19th century.
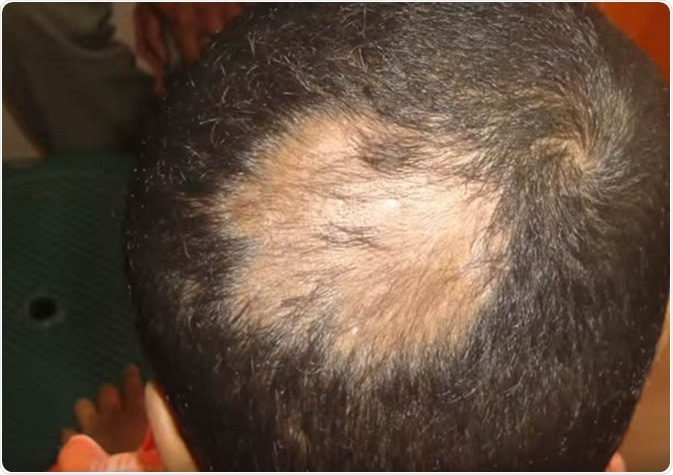
Folliculitis Decalvans. Image Credit: Ravi Clinic / Shutterstock
It is seen mostly in middle age, in both men and women, and the patches spread slowly from the vertex and back of the scalp. The affected scalp skin shows redness around the follicular openings, with pustule formation and crusting tinged with dried blood.
The pustules usually contain Staphylococcus aureus. The scarring and the pustules are characteristics of FD. Some patients may have pain and bleeding lesions, while in progressive types of FD, the skin develops small irregular scars which may be lighter than the normal skin.
Thickening and induration of the affected skin has been observed rather than atrophy. Even after the pustules subside, scarring may continue to take place.
The condition is also known as tufting folliculitis because many hairs emerge from a single follicle in this disease. It eventually leads to loss of the hair follicle and permanent baldness in that area.
Other than the scalp, the beard area, the axillary and pubic hair, the arms and the legs may be involved.
FD is the cause of about 11% of all primary scarring baldness. It is somewhat more common in African-Americans and has a slightly higher incidence in males.
Causes
S. aureus has been isolated in most patients with FD, but it is found on the skin of almost one in every three individuals in most communities, and is associated with infection in only about 0.05%.
Major histocompatibility complex (MHC) class II molecules may play a part in susceptibility to this bacterium, since S. aureus cytotoxins could bind to them and evade elimination by the host’s immune defences.
They do activate T cells, however, leading to chronic infection. A simpler explanation might be the inherent weakness of host immunity. Some cases appear to run in families, lending weight to a genetic mechanism.
Diagnosis and Management
The first step is to take a careful history, as well as a medical history in general, bout the lesions themselves, the time when they started, the earliest symptoms, the associated pain or itching, and other symptoms such as bleeding and crust formation, and symptom progression.
Any history of preceding scalp injury and a family history of similar illness should be determined.
Scalp examination with microscopy and polarized light helps exclude dermatophytic infections. All findings should be recorded for future monitoring. If FD is suspected, a skin culture and biopsy are also performed.
Management depends upon sympathetic education. The patient must understand that hair loss can be arrested but hair growth cannot be restored.
Moreover, the treatment may have to be continued lifelong. Some forms of camouflage may be required if the patient is suffering psychologically from FD. These may include scarves, caps and even hair pieces, all of which should be disinfected regularly and rotated.
The eradication of S. aureus may require oral antibiotics from the antimycobacterial, tetracycline, macrolide, penicillin, and sulfa families, and combinations of these with other powerful drugs. However, they are often required for years because of frequent relapses.
Side effects are numerous and should be promptly managed. Topical antibiotic creams and and disinfectant shampoos may be adequate if applied daily for very mild cases. In a few patients, topical steroid application and intralesional steroid injections may help to relieve inflammation, but should be combined with antibiotics to treat rapid progression.
In such cases, oral corticosteroids have been used especially in combination with vitamin A analogs and antibiotics, but caution is highly recommended due to the many and potent side effects. Photodynamic therapy has also been reported to be successful.
Surgical transplantation of hair follicles may be considered in rare cases since it may itself precipitate a flare-up or even be the initiating factor.
Further Reading
Last Updated: May 19, 2023