Tetanus is a potentially life-threatening infectious disease that is usually transmitted through environmental exposure. It can also sometimes be referred to as lockjaw due to its characteristic symptom of muscular contractions, which usually present initially in the jaw.
Without treatment, 25% of people with the infection are likely to die and it is, therefore, imperative that treatment is sought as soon as possible. There is also a tetanus vaccination available, which allows the prevention of the infection, even if an immunized individual is exposed to the infection.
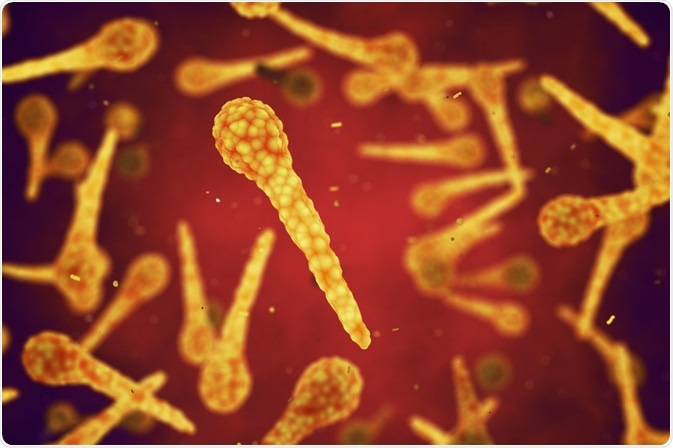
Image Credit: nobeastsofierce / Shutterstock
Causes and Pathophysiology
Tetanus is caused by the bacteria Clostridium tetani, which is anaerobic, Gram-positive and is commonly found in soil, dust and manure as a spore but can exist anywhere in the environment.
The infection may occur when a wound, such as a cut or deep puncture, is exposed to the Clostridium tetani bacteria around the individual. The soft tissue of the host with low levels of oxygen is the perfect breeding ground for the anaerobic bacteria, which proliferate and create spores that evolve into vegetative bacilli. These spores then excrete a neurotoxin called tetanospasmin that affects the central nervous system (CNS) and causes uncontrollable muscular contractions.
Symptoms
It usually takes about 3-10 days for symptoms to become evident after exposure to the bacteria, although the incubation period may be as long as three weeks. In most cases, faster onset of symptoms correlates to more severe symptoms and a greater probability that the disease will be fatal.
Signs of tetanus may include:
- Stiffness of muscles in the jaw
- Neck stiffness
- Difficulty swallowing
- Stomach muscle stiffness
- Spasms of muscles
- Sweating
- Fever
- Bloody stools and/or diarrhea
- Tachycardia
It is also possible for bone fractures, particularly of the spine, to occur as a result of the tetanus infection and muscular contractions.
Treatment
Any case of suspected tetanus is a medical emergency and patients should be treated as quickly as possible.
Immediately after the occurrence of the wound and possible exposure to the bacteria – before the infection becomes symptomatic – it is important to clean the wound adequately.
The individual should then receive a tetanus immunoglobulin injection, regardless of previous vaccination history. When administered early in the lifespan of the infection, these antibodies are able to kill the Clostridium tetani bacteria and prevent the disease from progressing. Antibiotics may also be used in some cases to aid in the prevention of bacterial spread.
For symptomatic patients, anticonvulsants such as diazepam and phenobarbital are usually required to control muscular spasms. Additionally, muscle relaxant drugs like baclofen are also used to address symptoms of muscle stiffness.
In some cases, a ventilator may be required to assist patients who are having difficulty breathing and the medical practitioner may opt to surgically remove the area surrounding the original wound to eradicate of a large proportion of the bacteria.
Immunization
Tetanus is preventable as a result of the tetanus vaccination that protects against the infection.
In most developed countries, infants are immunized against tetanus along with several other standard vaccinations. This consists of three separate injections at the age of approximately two, three and four months. A booster shot is given at around four years of age and a final injection is administered between the ages of 13 and 18.
In total, these five vaccines provide adequate protection against tetanus for a lifetime. However, even if an individual has been immunized against tetanus, it is advisable for them to seek medical attention if they suspect they may be exposed to the bacteria. A post-exposure vaccination of antibodies against tetanus ensures that the infection will not take hold and cause symptoms for the individual.
References
Last Updated: Nov 8, 2022