The protozoan parasitic species Trichomonas vaginalis (also commonly referred to as “trich”) and the condition it causes (known as trichomoniasis) likely represents the most abundant non-viral sexually transmitted infection worldwide.
Although previously considered more of a nuisance as a sexually transmitted disease, now it is being acknowledged as a substantial cause of reproductive morbidity, also acting as an important facilitator of the transmission of human immunodeficiency virus (HIV) – and therefore a paramount public health issue.
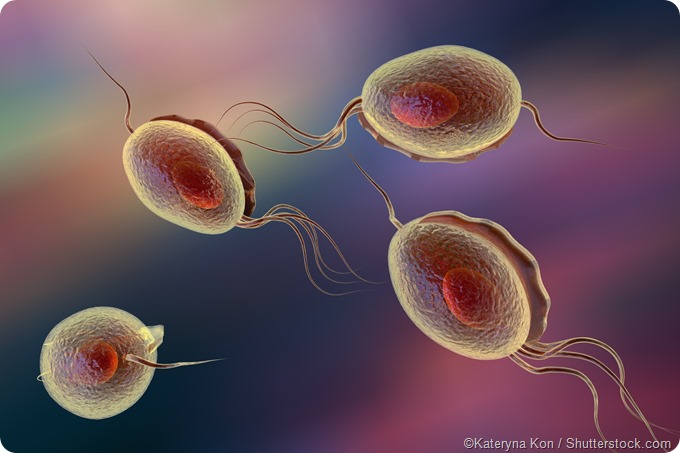
The infection is seen more commonly in women (especially elderly women) than in men, affecting the lower genital tract and urethra, respectively. The majority of infections are asymptomatic, but symptoms may and do occur, ranging from mild irritation to severe inflammatory syndromes. Trichomoniasis can also result in dyspareunia or discomfort during sexual intercourse.
Wet preparation microscopy and culture are the most commonly employed diagnostic approaches. Whilst simple to carry out, they are less sensitive than molecular techniques (currently only approved for women). Regarding the treatment, a single dose (i.e. 2 grams) of metronidazole is the preferred treatment regimen for both the primary patient and their corresponding sexual partners.
Epidemiology and risk factors for trichomoniasis
Whilst trichomoniasis is not a reportable disease, there were approximately 280 million cases of the disease in 2008 (according to the World Health Organization), with about 90 percent of them in people from resource-limited setting. That makes Trichomonas vaginalis more prevalent than a combination of gonorrhea, chlamydia and syphilis. Furthermore, those numbers may be lower than the actual figures as there are no formal surveillance systems in place and the results are drawn from microscopy studies, and not molecular techniques.
Studying 'Trich': The STD You Probably Haven't Heard of
Trichomoniasis has been found in every continent and climate without showing any significant seasonal variability. Humans are the only natural hosts for the spread of a causative parasite Trichomonas vaginalis, which is transmitted from one person to another by a sexual intercourse. This is supported by the high rate of urethra and prostate infections in male partners of infected women.
The age-specific distribution of trichomoniasis is interesting to note - it differs considerably from the distribution characteristic for chlamydial infections. It is known that chlamydia rates peak in younger women aged from 19 to 24 years; conversely, a myriad of studies have demonstrated that the prevalence of trichomoniasis is highest among those women between 40 and 49 years old.
On the whole, individuals of African descent present with higher rates of trichomoniasis – this is illustrated by higher infection rates seen in Sub-Saharan Africa and among individuals of African descent in other regions, such as the United States. In addition to increased age and individual race, other risk factors for trichomoniasis include intravenous drug use, incarceration, commercial sex work, as well as testing positive for bacterial vaginosis.
Pathogenesis of the disease
Although pathogenesis and virulence of Trichomonas vaginalis in the progression of trichomoniasis is not fully elucidated, substantial progress has been achieved in identifying products of this protozoan that can damage host tissues and cells. Two different schools of thought coexist regarding the pathogenesis of Trichomonas vaginalis – contact-dependent and contact-independent. It is very likely that both mechanisms are important in the development of infection.
In any case, the adhesion process is pivotal in the onset of trichomoniasis, as it triggers the degradation of the cell membrane skeleton and subsequent cytolysis (or disintegration of the cell). The only host-cell receptor of Trichomonas vaginalis is known as galectin-1; it is found on epithelial cells of the cervix and binds lipoglycan present on the parasite body.
Recent research endeavors suggest that Trichomonas has the ability to produce molecules that target cells and confer cytotoxicity by damaging cell plasma membrane. One such molecule can create pores in the membranes of erythrocyte membranes (which was detected by using electron microscopy), thereby exhibiting perforin-like activity.
In addition, the parasite has the propensity to adsorb host plasma proteins that have a role in its protection or nutrition or protection. The production of extracellular proteases (most notably, cysteine proteases) may represent a potential virulence factor by inactivating or altering a plethora of host proteins.
Clearly, trichomoniasis has been acknowledged in the recent decades as being more important condition than previously thought. Some important questions remain regarding the immunology of the pathogen, potential complications in pregnancy, achieving accurate diagnosis, as well as public health control of this parasite and the infection it causes.
Further Reading
Last Updated: Feb 27, 2019