An aqueous flare is an optical phenomenon based on light scattering within the anterior chamber of the eye. This phenomenon occurs when an inflamed eye is viewed at right angles to a beam of light shined obliquely into the anterior chamber.
How does aqueous flare occur?
The human eye consists of two chambers, the anterior chamber and posterior chamber, separated by the iris and the lens. The anterior chamber contains clear fluid, located between the cornea in front and the lens behind. The iris, or colored membrane around the pupillary opening, touches the front of the lens lightly, and cuts off the anterior chamber from the posterior chamber, albeit not completely.
The fluid within the anterior chamber is called the aqueous humor. It is normally transparent akin to water, and lets through all the light from the front of the eye, so it can pass through the lens to fall on the retina.
However, when there are proteins present inside the fluid, the light may reflect in multiple directions, leading to the scattering of light. This is called the Tyndall effect, and is due to the presence of turbidity in the aqueous humor.
This means that the fluid contains more protein than it is normally present, but also (in most instances) inflammatory cells. This is an accurate sign of inflammation inside the anterior chamber, and is called an aqueous flare.
In other words, an aqueous flare means that particles floating in the aqueous humor become visible when a ray of light is shined through. Furthermore, the degree to which vision suffers depends on how strong the flare is.
As various photons present in the light beam pass through the aqueous humor, those which have a longer wavelength travel further before being scattered, while the ones which have a shorter wavelength scatter quickly, moving sideways and backwards relative to the beam.
aqueous flare and cell
What causes aqueous flare?
Aqueous flare occurs with one type of uveitis, namely, anterior uveitis or inflammation in the anterior chamber. Uveitis is a general term given to inflammation within the eye, and anterior uveitis may be caused by infections, non-infectious conditions and trauma.
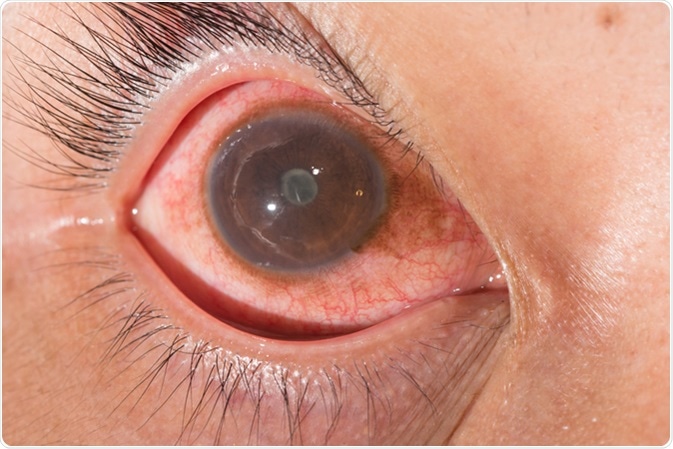
Close up of the anterior uveitis with posterior synechia during eye examination. Image Credit: ARZTSAMUI / Shutterstock
In normal eyes, the anterior chamber liquid is clear and colorless. It seeps out from the capillaries of the blood vessels that supply the eye.
There is an epithelial barrier between the blood and the aqueous humor that prevents cells and proteins from entering the latter, under normal circumstances. When this breaks down as a result of inflammation, proteins are exuded into this fluid, causing the aforementioned flare.
Other signs of anterior uveitis include:
- Keratic precipitates, which refers to the presence of solitary cells or those in clumps sticking to the inside of the cornea;
- Leaky capillaries leading to inflammatory cells in the aqueous humor, hypopyon (pus in the anterior chamber), fibrin exuded into the anterior chamber, bloody anterior chamber fluid (red and white blood cells in a mixture);
- Pigmentary dispersion, or pigment within the anterior chamber, which has been dislodged from the pigment epithelium of the posterior chamber or iris;
- Contracted pupil;
- Iris nodules;
- Adhesions or synechiae between the iris and other parts of the eye.
Granulomatous inflammation may be due to infections like syphilis, tuberculosis, herpes infections or Lyme disease, but most commonly it is associated with autoimmune disease or systemic illnesses. Thus both eyes are more commonly affected in this form.
Nongranulomatous inflammation is usually of unknown origin and occurs in an acute one-sided form, compared to the more chronic course of granulomatous uveitis.
Masquerade uveitis may also occur with conditions like lymphoma, or as a result of some drugs like bisphosphonates, rifabutin and some biologics.
How is aqueous flare measured?
Aqueous flare is graded from 0 to 4 as shown in the following table, using the Standardization of Uveitis Nomenclature (SUN) Working Group grading scheme. Grading helps to understand how severely inflamed the anterior eye chamber is, and also to assess how well the treatment is working. Thus it can be used to monitor the course of treatment and follow up the patient. However, slit lamp grading depends on subjective skill and assessment and is, therefore, rather inaccurate.
Table 1.Grading Aqueous Flare by Slit Lamp
|
Grade
|
Features
|
|
0
|
No flare
|
|
1+
|
Faint flare
|
|
2+
|
Moderate flare, but the iris and lens can be clearly visualized in detail
|
|
3+
|
Marked flare, partially obscuring iris and lens
|
|
4+
|
Intense flare, with fibrin exudate or plastic aqueous
|
Currently, laser flare photometry (LFP) is recommended as a method of flare detection and quantitation under automated conditions. Its use allows an objective assessment of the degree of inflammation within the eye, and is thus important in the management and follow-up of acute and chronic anterior uveitis. In fact, this has become the most reliable or weighty test for children with aqueous flare due to autoimmune anterior uveitis, and is also characterized by good prognostic value.
How is aqueous flare observed?
Conventionally, a slit lamp was used to observe and grade aqueous flare. For this purpose, the slit lamp is set to 16x magnification, and the beam parameters are set to 1 millimeters width and 3 millimeters length with the highest intensity. When the eye is examined the slit lamp is shined through the pupil. The beam of light passes through the anterior chamber in a slanting direction, while the viewer is positioned at right angles to the beam.
Diagnosis and management
Anterior uveitis must be evaluated thoroughly to pinpoint the affected area, as well as the duration, the type of inflammation, the underlying reason and the side of the lesion. Finally, a full medical examination with laboratory tests as required may be needed to reveal the possible cause and, consequently, to begin targeted treatment.
Further Reading
Last Updated: Dec 9, 2022