A team of doctors have replaced the cancer affected windpipe of a patient with an organ made in a lab. This is a medical breakthrough for regenerative medicine. The patient no longer has cancer and is expected to have a normal life expectancy, doctors said.
Paolo Macchiarini, a professor of regenerative surgery who carried out the procedure at Sweden's Karolinska University Hospital said, “He was condemned to die. We now plan to discharge him [Friday].”
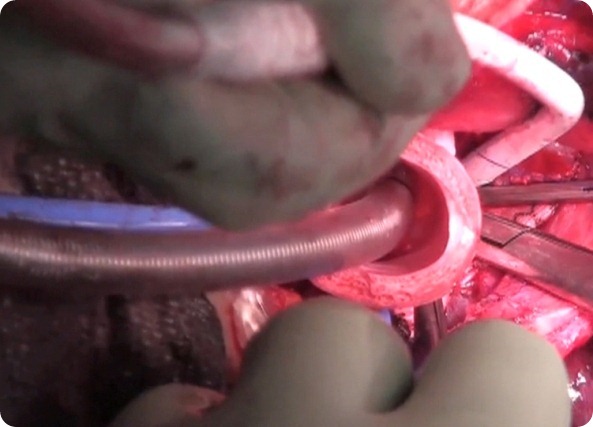 The team made an entirely synthetic and permanent windpipe in the lab on the patient on the 9th of June. The researchers haven't yet published the details in a scientific journal. The patient's speedy recovery marks another milestone in the quest to make fresh body parts for transplantation or to treat disease. More immediately, it offers a possible treatment option for thousands of patients who suffer from tracheal cancer or other dangerous conditions affecting the windpipe.
The team made an entirely synthetic and permanent windpipe in the lab on the patient on the 9th of June. The researchers haven't yet published the details in a scientific journal. The patient's speedy recovery marks another milestone in the quest to make fresh body parts for transplantation or to treat disease. More immediately, it offers a possible treatment option for thousands of patients who suffer from tracheal cancer or other dangerous conditions affecting the windpipe.
Alan Russell, director of the McGowan Institute for Regenerative Medicine in Pittsburgh, who wasn't involved in the latest operation said, “It's yet another demonstration that what was once considered hype [in the field of tissue engineering] is becoming a life-changing moment for patients.” Lab-grown bladders into children and teens with spina bifida, a birth defect were implanted successfully in 2006. And in 2008, members of a team that included Dr. Macchiarini said they had given a patient a new windpipe made partly from her own cells, and partly from “scaffolding” material taken from a cadaver. The latest experiment shows that a fully functioning windpipe can be manufactured in the lab without the need for a cadaver.
Dr. Macchiarini explained, “It makes all the difference. If the patient has a malignant tumor in the windpipe, you can't wait months for a donor to come along.” This operation was done on 36-year-old Eritrean man, identified by doctors as a father of two studying geology in Iceland. Surgery and radiation treatments failed to stem a cancerous growth in his windpipe. When the tumor reached about six centimeters in length, it almost completely blocked the trachea, or windpipe, making it hard for the patient to breathe. With no suitable donor windpipe available, the final option was to try to build one from scratch.
As a first step, a team led by Alexander Seifalian of University College London used plastic materials and nanotechnology to make an artificial version of the scaffold in the lab. It was closely modeled on the shape and size of the Eritrean man's windpipe. Prof Seifalian said, “What makes this procedure different is it's the first time that a wholly tissue-engineered synthetic windpipe has been made and successfully transplanted, making it an important milestone for regenerative medicine. We expect there to be many more exciting applications for the novel polymers we have developed.”
Meanwhile, researchers at Harvard Bioscience Inc. of Holliston, Mass., made a bioreactor. The artificial scaffold was placed on the bioreactor, and stem cells extracted from the patient's bone marrow were dripped onto the revolving scaffold for two days. Dr. Macchiarini and colleagues then added chemicals to the stem cells, persuading them to differentiate into tissue—such as bony cells—that make up the windpipe.
Dr. Russell of the McGowan Institute sounded a note of caution about using this technique to build more-complex organs. For example, while tissue engineering can help to build hollow organs such as a windpipe, it will likely prove a bigger challenge to use the technique for creating the heart, which has much thicker tissue.
Dr. Macchiarini said he planned to use the same windpipe-transplant technique on three more patients, two from the U.S. and a nine-month-old child from North Korea who was born without a trachea.