Regular pregnancy tests work a little bit like a simple light switch that you have on your wall. It’s either on or off. When it’s on, that means the test is positive; if it’s off, obviously, it’s negative.
What determines whether the light switch -or the test- is on or off, is a threshold level, or a minimal level, of the hormone of pregnancy, which is called human chorionic gonadotropin, or hCG.
Most of the pregnancy tests that are currently available either at the chemist or the drugstore or at your doctor’s office have a very low threshold (which means it’s very sensitive) for determining the presence of hCG. And once you’ve exceeded that threshold, the test is positive.
It doesn’t give you any relative information about how today’s test compares to yesterday, or a week ago, or how it will compare to a test you might do next week. It’s just on or off, positive or negative.
The ones that you buy in the store that are generally available are very sensitive, so even with a very small amount of hCG which may be present five or six days after conception, the test will turn positive.
What is a semi-quantitative pregnancy test (SQPT) and how does it differ from a standard pregnancy test?
A semi-quantitative test is more like a light switch with a dimmer. So, instead of just on or off, you can see relative brightness of the light bulb.
The way that we have arranged the semi-quantitative test to work like this dimmer is to arrange five separate little brackets. So, it’s not like a continuous dimmer, but it’s a dimmer with five different settings.
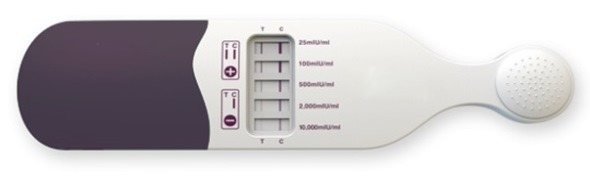
An image of the test similar to the one used in a variety of studies. The purple “cover” slips off and shows the “paddle” part of the test, which is then dipped into the cup of collected urine. The “brackets” (like the settings on the dimmer switch) in the “windows”, represent the different levels of hCG being tested.
So now, using this test, you have the baseline setting, which would be the same as the ordinary pregnancy test that you buy on the street or in your doctor’s office, but you also now have these other settings which are increasingly less sensitive, which means you need more hCG in the system in order to make them turn positive.
For example, let’s say we do the test today, and I’ve just conceived maybe five days ago. I would expect that the very lowest (most sensitive) level of the test would be positive; but the other brackets, the other settings of this dimmer, would probably still be negative.
Thus, I might have a positive test for a very, very early pregnancy, but I don’t know how well it’s progressing.
But now, especially if I was concerned about the progress of my pregnancy, I might repeat the test in a couple or three days, or maybe four days, and now the next level bracket, or even two brackets up, might be positive. This means that there is an increasing level of hCG in my system.
By being able to make relative assessments, or serial assessments, of how one day compares to another, or maybe every few days, we might be able to get a handle on whether a pregnancy is progressing or regressing. In other words whether the hCG is going up or down.
Right now, the use to which they’re being put, even as we speak, is in the realm of medical abortion.
Is medical abortion the reason SQPTs were developed?
Like most things, necessity is the mother of invention.
In the setting of medical abortion women take pills to basically induce a miscarriage, to induce an abortion.
In many countries of the world (this is not necessarily the state of the art in the UK right now, but in the US and in many other countries it is), women essentially take these pills at home and have the miscarriage, or the abortion, at home. And I just want to note here, that this approach has been shown to be highly safe and effective.
The effectiveness rates, and what we mean by effectiveness is that the woman safely and effectively has the abortion process or the miscarriage process at home with no need for any surgical intervention, are about 95% to 98% , depending on the actual gestational age.
Now, that being the case, you can understand for the vast majority of women, they really don’t need to come in to the office for a follow-up, which in the UK and in many other places is currently done wither with ultra sound, which is both expensive and somewhat invasive, or with a blood test, which is also expensive and somewhat invasive.
If there was a way that we could help the woman even at home, or even if she did come to the doctor’s office, avoid the need for the more expensive technology and use a simple, cheap test that would have a result for us in a few minutes, that would be a valuable tool. That is, if there was some way that we could determine who really would benefit from some follow-up and who really doesn’t need it that would be great.
How were these tests developed and how long did the development process take?
Well, you’d be surprised how long it actually took to get where we are now. But, basically, I started to have this idea in the mid to late 1990s.
When we first started to have our national experience with medical abortion in the US, ultrasounds were expensive and blood tests were expensive. What I realized was you could take the patient’s urine and dilute it.
The pregnancy tests we had at the time were the ones that I described at the very beginning of this discussion - they’re very sensitive so they always turn positive. And so even though the abortion might be over, the HCG stays in the system for a few weeks.
So, a very sensitive pregnancy test would be positive, but, if I diluted the urine in my office and instead of just using one drop of urine on the pregnancy test I took one drop of urine and diluted it with ten drops of water, and then repeated the pregnancy test, I might find that now the pregnancy test was negative.
The initial test was positive, which I means that I might have, say, twenty-five units of hCG, but if I diluted it by a factor of ten, with ten drops of water and now the test is negative, that tells me that I have less that 250 units of hCG.
This gets to be a little laborious in the office, the constant putting of drops of water into a drop of urine and so I decided that it would be a lot easier if I could pre-dilute the urine by making a pregnancy test that already had the dilutions built into the test. And that’s how the semi-quantitative test evolved.
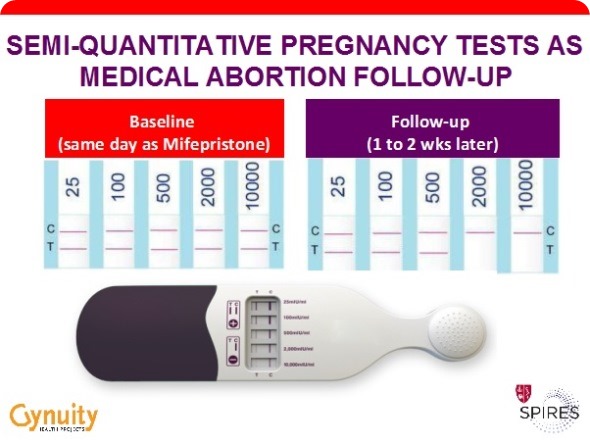
This shows the test at baseline (> 10,000 mIU of hCG) and perhaps 10 days after taking the abortion medications, where the test now shows the hCG level is below 2,000, which means that the abortion process is highly likely to have completed successfully.
Instead of having to put drops of water into the urine, we created the test paper which actually is less sensitive, which means it needs more hCG to turn the switch on.
Now, in the setting of medical abortion, if a woman takes the test at the beginning of the process - so the day she takes the first pill, for example - on average, the test will generally show that the hCG level is over 10,000. This is very common after about six weeks of pregnancy.
But if she then repeats the test after 7-10 days, let’s say, she’ll find - if the process is going well - that now the test is negative at 10,000. It might even be negative at 2,000. This tells us that the hCG level has definitely gone down, which means the process is evolving successfully, and there is no ongoing (or continuing) pregnancy.
We have now done several kinds of studies with this test to show that if you use this test in a real clinical setting that it does pick up on the people that we want to identify most and those are the people for whom the medical abortion process has failed. In other words, their pregnancy is just continuing as if nothing had happened.
So those are the people we want to identify most critically. And this test has shown us that it identifies them just about 100% of the time. Those are the people who really do need follow-up.
Can SQPTs be used at home?
Yes. We think they absolutely can be used at home. In the US the company that is getting the license for distribution of this test will be applying for having it available for what we call over-the-counter use.
We have already done several studies to show that women can use these tests at home and then just call the clinic for minimal follow-up. Thus they do not have to come into the clinic at all.
Are SQPTs used in the same way as standard pregnancy tests?
You pee into a little cup, and then - because of the five brackets it’s more like a little paddle - you dip the paddle into the cup of urine.
Then you wait, in this case about fifteen minutes, and you get the answer for these five different brackets.
What impact do you think SQPTs will have?
I think first of all, just in the realm of medical abortion, it could greatly simplify the process both for providers and for women. Right now there’s a lot of time that providers spend either making appointments for, or actually seeing, women that don’t need to be seen. Both the providers and the patients have better things to do with their time than make unnecessary appointments!
Likewise, there are many women who are given appointments, or who feel they should be followed up, when - if they were to use this pregnancy test - they probably don’t need to be followed up. In fact, if the test tells them what we’re looking for, then we at least know that they don’t have an on-going, or continuing, pregnancy.
One of the interesting things that we’ve found is that right now, especially in the US and I think the same is true in the UK, the actual follow-up rates for medical abortion care for women who actually come to the clinic, is actually very low.
This is because more often than not the women actually feel okay and maybe they did have the cramping and bleeding which is part and parcel of the abortion process, but in some cases they think everything has gone well, but in actual fact it has not.
In the studies that we’ve done so far, by just asking the women to call the clinic instead of showing up at the clinic, we actually get a higher follow-up rate with the pregnancy test because it’s much easier for them to use the pregnancy test at home and make a call than it is for them to find the time and the transport and so forth to get to the clinic.
We actually learn more about how these patients are doing by use of the pregnancy test, in some cases, than when we require, or have requested, an actual follow-up in person.
So these tests will probably greatly simplify and make medical abortion less expensive. But they have other impacts as well.
One thing that we’re actually exploring right now is their use in assisted reproductive technologies - whether it’s intrauterine insemination, or IVF, in vitro fertilization.
For example, a woman who has intrauterine insemination, or any kind of insemination, or even just attempting to get pregnant the old fashioned way, can actually follow the very early progress of the pregnancy and watch the hCG go up every few days, so that when it gets to a certain level on the test, for example 2,000 or 10,000, that’s when we know that if we were to do an ultrasound for that woman, we should expect to see something in the uterus.
This is very reassuring, especially for women who have had a lot of assistance with reproduction. They’re very, very anxious to know what’s going on. For those women, instead of having to come to the office for a blood test, or perhaps for an ultrasound which may even provoke more anxiety as we don’t see anything in the uterus just yet.
By doing this test at home, we might be able to both provide reassurance that things are going in the right direction and give them a threshold point at which we say, “Okay, when the test hits 2,000, now make an appointment for the clinic because we should see something.”
There are other uses as well. For example, the possibility of following the progress of a tubal pregnancy, which has been managed with medication as opposed to surgery.
We could even use this to triage the status of a patient who presents to casualty with a possible ectopic pregnancy. It will tell us, in the course of a few minutes, whether we should expect to see something in the uterus in ultrasound, or not; whereas right now, the patient might have to have a blood test done, which takes several hours if not a day to get the results back and so forth.
This is especially important in developing countries where blood tests are more difficult to find, and are even more expensive than they are in some developed countries and where ultrasound is either less accessible and perhaps even less reliable.
Where are SQPTs currently available?
They’re currently available in the US and they can be ordered from a manufacturer in the US.
However, right now if you were to order the test you would be getting an older version of the test, which we think doesn’t work as well as the version that we’ve currently been testing and getting ready for commercialization.
We will need to wait for the new, improved version of the test to be approved by the FDA etc.
We are also looking at making the test available in other countries. For example, with our partner, Gynuity Health Projects, the countries where we’ve been currently exploring the value of the test include places like Vietnam, the United States, Mexico, Moldova, Georgia, and Tunisia - a variety of countries that have different levels of sophistication in their health care systems.
How do you think the future of pregnancy tests will develop?
I think they’ll probably develop along two tracks. Right now this test, partly in order to keep costs down, is what we call semi-quantitative. In that there are several pre-defined brackets. For simplicity’s sake we can continue to refine this kind of semi-quantitative test.
But it might be possible to, in the future, develop a pregnancy-dipstick type test which is truly quantitative. In other words, it will actually tell you the level. Instead of it just telling you how one bracket compares to another, you might actually be able to pee on a device, or in a cup, and then dip the device into the cup, and then, let’s say, plug it into your iPhone and it will give you the answer - it’ll give you the number.
So, that’s one way things could develop. That’s what I perceive as the next leap in these kinds of tests.
Is it true that women in ancient Egypt used to urinate on seeds to determine whether they were pregnant?
I’m not sure; however, it makes sense that they could have done because hCG makes things grow. So it certainly might be possible. Here’s a link to more information about that: http://mentalfloss.com/article/48655/9-historical-methods-detecting-pregnancy. By the way, if you put birth control pills in your tomato plants, they’ll grow like crazy.
How was this work on SQPTs funded?
The work on this test has been a collaboration between Stanford University and Gynuity Health Projects and it’s been funded through an anonymous donor.
Where can readers find more information?
Can at-home semi-quantitative pregnancy tests serve as a replacement for clinical follow-up of medical abortion? A US study. Blum J, Shochet T, Lynd K, Lichtenberg ES, Fischer D, Arnesen M, Winikoff B, Blumenthal PD.
Simplified medical abortion using a semi-quantitative pregnancy test for home-based follow-up. Lynd K, Blum J, Nguyen Thi NN, Shochet T, Blumenthal PD, Winikoff B
About Dr. Paul Blumenthal
 Paul D. Blumenthal, MD, MPH is Professor of Obstetrics and Gynecology at Stanford University School of Medicine.
Paul D. Blumenthal, MD, MPH is Professor of Obstetrics and Gynecology at Stanford University School of Medicine.
He directs the Stanford Gynecology Service and the Division of Family Planning Services and Research at Stanford. He also directs SPIRES, the Stanford Program for International Reproductive Education and Services, an initiative providing technical assistance and training to family planning programs in a wide variety of countries across Africa, Asia, and Central America.
Dr. Blumenthal received his medical degree from The University of Health Sciences/The Chicago Medical School in 1977 completed a residency in obstetrics and gynecology at Michael Reese Hospital and Medical Center in Chicago, followed by a Fellowship in Family Planning at UCLA in 1982.
For over 25 years, Dr. Blumenthal has been an advisor to multiple international agencies such as Gynuity Health Projects, Ipas, Pathfinder, Family Health International, Path, JHPIEGO Corporation, and the World Health Organization and served as the Special Advisor to Minister of Health and Family Planning of the Republic of Madagascar.
He currently serves as the Global Medical Director for Population Services International, and has served as Medical Director for both the Planned Parenthoods of Chicago and Maryland in the past.
Among other things, Dr. Blumenthal is currently involved in studies of community-based distribution of injectable contraceptives, Post Partum IUD insertion, and “single visit” approaches to the prevention of cervical cancer and simplification of both medical abortion regimens and contraceptive delivery systems.
He is an author of over 115 peer-reviewed publications involving collaborations from over 20 countries. Dr. Blumenthal is committed to the development and implementation of innovative approaches to reproductive health issues in both the domestic and international arenas.