Virtual reality and augmented reality use similar technologies but offer slightly different experiences and usage scenarios.
We’ve developed a VR training tool that enables trainee surgeons to become immersed in another surgeon’s reality and gain their perspective of a recorded operation.
.jpg)
AR could be used to improve an operating surgeon’s experience of live procedures by displaying things like patient diagnostics, radiological images and physiological data on a headset. The opportunities are huge in both areas.
How do you think virtual and augmented reality could improve surgical education?
VR technologies have reached a stage where we can provide a highly realistic, immersive experience that helps people embed procedural techniques to memory, familiarize themselves with their working environment and develop softer skills, such as communication.
Rather than watching from a distance or an odd angle, students will be able to see our operations from the surgeon’s perspective.
The current generation of medical students have grown up in an age that encourages e-learning and they are comfortable with new technology. It seemed a natural progression to use VR to provide additional learning experiences they would be comfortable with, especially when they offer such profound improvements.
There is global shortage of surgical skills, especially in the developing world, so helping to spread surgical knowledge more efficiently and in the most impactful way is another good reason to create these tutorials.
Why do you think the way surgeons are trained hasn’t changed much over the last 200 years?
Surgery has always been learned through apprenticeship. Students must spend time in an operating theatre to get quality training from a mentor.
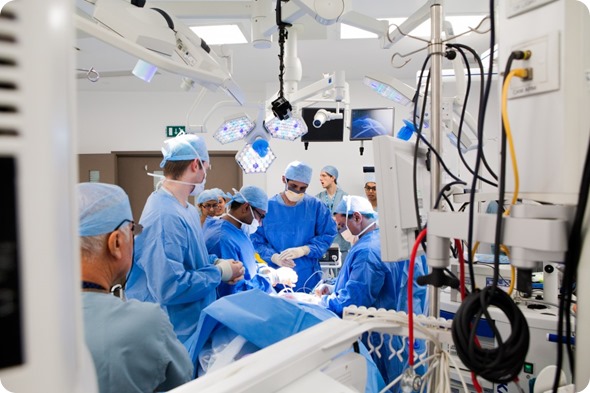
While hospitals have got bigger and surgery has improved, the theatre space around the patient is still limited and it is difficult to provide everyone with a good view.
VR lets every student learn from the best seat at the operating table.
What challenges will need to be overcome to improve surgical training?
Technically, we have pretty much everything we need. The internet allows us to stream operations and tutorials around the world and new headsets constantly improve the quality of the experience.
The only major challenge we need to navigate is fear of change. The surgical community will get used to the idea that a single operation can be used to teach more than just a couple of chosen students. If you can teach one person why not teach 1,000? It is far more efficient.
Can you please outline the 360-degree surgical training video Medical Realities published earlier this year? What were the aims behind this video?
The original video we put on YouTube demonstrated that VR could be used to improve surgical training and that there was a credible and unintrusive way of filming these procedures.
Medical Realities - Surgical Training in 360-Degree Virtual Reality
It also gave us the opportunity to develop the Virtual Surgeon product and wrap further value around the experience so that it becomes more than just a new way of watching operations.
What videos do you plan to produce next?
We are going to start by creating training tutorials for common surgical procedures including laparotomy, treatment of open fractures, hernia repair and emergency cesarean section delivery.
These tutorials will include interactive computer graphics and the ability to review patient history to provide additional insight.
How do Medical Realities plan to distribute these training tutorials? Will they be available globally?
We are going to make the tutorials available to teaching hospitals in modular format on the Oculus Rift device, and to medical students and surgical trainees of all levels via mobile apps and YouTube.
What do you think the future holds for virtual and augmented reality in surgical training?
I’d like to see a VR world in which full surgical simulation with audio, visual and tactile feedback is possible, so that every time a surgeon performs a new procedure for the first time on a person they will already have performed it using virtual surgical instruments on a virtual patient with a virtual team.
Where can readers find more information?
www.medicalrealities.com
About Dr Shafi Ahmed
Dr Ahmed is a highly experienced general and colorectal surgeon, operating at The Royal London Hospital and a co-founder of Medical Realities, an innovative medical training startup specializing in virtual reality, augmented reality and serious games.
In 2007 Shafi was appointed as a Consultant General, Colorectal and Laparoscopic Surgeon at Bart's and the London NHS trust. In 2014 he performed the world’s first live-stream of an operation using Google Glass, which was watched live by 13,000 students around the world.