A new study has shown that people who have a psychiatric condition called intermittent explosive disorder (IED) are twice as likely to have been exposed to toxoplasma gondii, the parasite found in cat feces and undercooked meat.
Individuals with IED have violent outbursts of extreme anger in response to seemingly trivial irritations.
“The kind of triggers are usually social provocations,”
“In the workplace it could be some kind of interpersonal frustration, on the road it could be getting cut up.”
Royce Lee, University of Chicago, one author of the study.
As reported in the Journal of Clinical Psychiatry, Emil Coccaro (University of Chicago) and colleagues recruited 358 adults and assessed whether their aggression levels were associated with toxoplasmosis infection.
The participants were categorized into three groups: around one third had no psychiatric problems, one third had IED and the remainder had a psychiatric problem other than IED such as depression. The researchers then examined blood samples taken from the participants to check whether they had been exposed to the parasite.
The findings showed that those who had been exposed scored significantly higher on the aggression tests than those who tested negative for exposure to the parasite. Furthermore, patients with IED were more than twice as likely to have been infected with the parasite than those with no psychiatric disorder.
Almost 22% of people who had IED tested positive for exposure to the parasite, compared with 9% of those with no psychiatric disorder and 16.7% of those with another psychiatric condition.
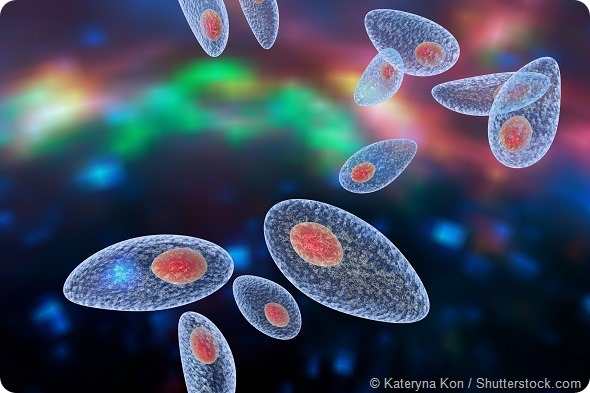
Toxoplasmosis is an extremely common parasitic infection thought to affect up to 16 million Americans. It is transmitted through contact with infected cat feces, contaminated water and undercooked meat.
It is usually latent and harmless among healthy people, but it is known to reside in brain tissue and has previously been linked to conditions such as schizophrenia and depression.
"We don't yet understand the mechanisms involved,” says Lee. “It could be an increased inflammatory response, direct brain modulation by the parasite, or even reverse causation where aggressive individuals tend to have more cats or eat more undercooked meat.”
The researchers are now carrying out further studies to examine the link between toxoplasmosis, aggression and IED and inform new strategies about diagnosing or treating IED.
"If we can learn more, it could provide rational to treat IED in toxoplasmosis-positive patients by first treating the latent infection," concludes Coccaro.