SIDS is the sudden and unexpected death of a baby, which usually occurs during sleep. The great majority of the babies are aged between about two weeks and seven or eight months.
Despite very thorough investigation after the death, including a detailed post-mortem and investigation of the circumstances, no adequate cause is found.
The death has a natural cause and seems to be something related to the developmental stage of the baby, but there's no simple explanation for it and it remains unexplained after all investigations.
Most years in the UK, somewhere between 200 and 250 babies die from SIDS.

© Shutterstock.com / Monkey Business Images
Can SIDS occur in babies older than 8 months?
Technically, the international definition of an infant is a baby under the age of one year. Children can die suddenly and unexpectedly beyond that but typically the term SIDS is only applied to children under the age of one year because that's what the definition of an infant is.
A very similar circumstance occurs in children of 13 or 14 months, but that is very rare. Of all the young infants and young children who die suddenly and unexpectedly, 90% of them are under the age of seven months and about 98% are under the age of one year.
Please can you outline the study being launched to investigate the potential to identify babies at greater risk of SIDS?
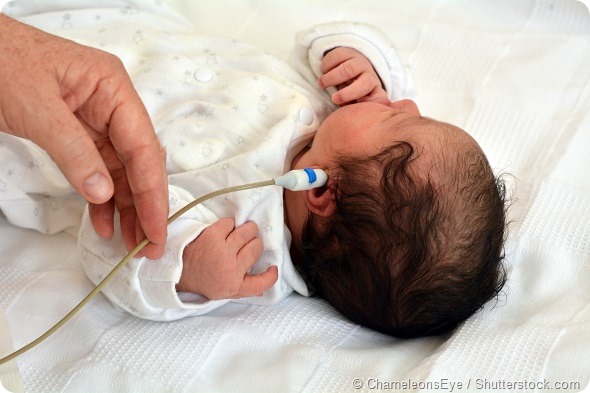
Work that we did a few years ago, and our collaboration with a group in the US that has done similar work, have shown that the routine hearing test that all babies in the UK have now is a direct measure of the function of the back part of the brain, which is where hearing is dealt with.
There are also some very important other functions in the back part of the brain, including the control of temperature, breathing, blood pressure and heart rate. We think those are all really important in terms of the things that can go wrong and cause babies to die suddenly.
The question that arose was whether we could look at those routine recordings for all infants and identify any aspect of them that was different in the babies who subsequently died suddenly and unexpectedly?
The answer was that yes, we could. In a small study from Rhode Island, we found that there were some very subtle differences in the recordings between babies who survived and babies who subsequently died. It's not that the babies who died failed their hearing test; they all passed it. It's much more subtle than that and involved a complex mathematical analyses of the wave forms.
The question then was whether we could confirm that and take it to a much larger scale, because if we can identify the babies who are at risk of dying suddenly, clearly we're then in a position to start making some very focused, individual-level attempts to prevent the deaths happening.
We've done a lot over the years to reduce the risk across the population, but for the individual baby who is particularly at risk, we've not been able to do much because we've not had a reliable way of identifying the baby who is at significant risk.
We can tell you that babies of parents who smoke are at an increased risk, as well as babies with other features, but those increases are still relatively small. More than 99% of the babies with those features still survive.
What we're trying to do is to look at whether using a combination of what we know currently about risk factors such as parental smoking, low birth weight and pre-term delivery, combined with some features of the routine new-born hearing screening, will enable us to identify a group of babies who are at a significantly increased risk. Then, we might be able to start some interventions that will look at the effectiveness of trying to prevent those deaths.
ChameleonsEye / Shutterstock.com
How much evidence is there to suggest that differences in new-born hearing test results could be indicative of a baby’s risk of SIDS?
There are several studies now and we've now got quite a lot of additional work. In work that I did 30 or so years ago, when we were measuring the transmission of signals across the baby's brain stem using some special electrodes that allowed us to test hearing in a slightly different way, we found that abnormalities of breathing control were associated with particular features of that.
Subsequently, a study from Italy that was done last year showed that among babies who had SIDS, using very careful and special testing of the area of the brain involved in hearing, it was possible to identify specific features that would fit in with what we'd already observed.
Thirdly, a group in Boston led by Professor Hannah Kinney who is the head of pathology at Boston Children's Hospital, have made some very similar observations. They found specific abnormalities in a part of the brain stem in babies who had SIDS.
Now, we want to see if we can establish a marker while the baby is alive and apparently quite healthy that would identify those babies who are at a real risk, so that we can start to try and do something about it.
What is thought to be the underlying mechanism of this association?
In terms of the final event or trigger event that may cause the baby to get into trouble and die suddenly and unexpectedly, there are probably a lot of different factors involved.
However, the final sequence of events seems to be that something goes wrong with the baby's ability to coordinate and maintain their breathing and blood pressure control. Those two factors are really tightly connected because you've got to be able to get the blood and oxygen to the organs that need it.
Breathing and blood pressure control are very tightly linked in babies and also in adults. If something goes wrong with that, then the baby will deteriorate and die quite quickly.
The final event is that, whereas normally, when something starts to go wrong, the baby would wake up, in these babies, something has gone wrong with the link from that area to the front of the brain which is the area that would tell you to wake up.
The mechanism seems to be that something either within the appreciation of a problem arising with breathing and blood pressure or something that tells the front part of the brain to wake up, has gone wrong. All of that is concentrated in this very tiny area of the brain stem, through which these hearing pathways go.
If a baby is found to be at a higher risk of SIDS, are there processes that can be followed to reduce the risk of the baby dying? Why are these processes not followed for all babies?
We know a lot about how to reduce the risk of SIDS in babies. In the 1980s in the UK, about 2,000 babies died this way. In the late 1980s, myself and my research group as well as a few other research groups around the world started to identify features of how the babies had been looked after that increased the risk.
For example, babies who were put down to sleep on their tummy, babies who got too warm (particularly at the time of infection), babies who had their heads covered or were exposed to tobacco smoke.
By taking away those factors, we've already reduced the occurrence of SIDS by about 90%. The number of babies dying now is a little over 10% of what it was 25 years ago. We've had a huge impact already, but those factors are generic and they apply to all infants. We're now trying to find out how to stop the deaths of individual babies who are, if you like, intrinsically at an increased risk.
There's no validated technique that has been shown to reduce the risk of dying in those babies. In the US, during the 1980s and early 1990s, a lot of attention was paid to the idea that if we monitored breathing very carefully in these babies, we might be able to protect them.
That's never been shown to work and it doesn't work. They stop breathing and can't be resuscitated. That was a simplistic approach that everybody thought was going to be an answer, but it wasn’t.
We've known now for 25 years that that doesn't work on a population basis. However, there are now some much more sophisticated, more expensive and much more complicated ways of monitoring babies' ability to deliver oxygen to the right tissues and so on. We still don't know whether they work, but we think they've got a better chance of working than the old, simple breathing monitors.
If we tried to apply that and see if it works on a population basis, where one in two thousand babies has SIDS, we would need to monitor about half a million babies. The cost of the monitoring equipment is several thousand pounds each, so the cost of doing that when we don't even know whether it will work would be astronomical and inappropriate.
If, on the other hand, we can identify a group of babies where the risk of dying is not one in two thousand, but perhaps one in ten, then starting to look at using more sophisticated technology to help those babies starts to become more of a realistic possibility. We have to be able to apply something to the group who are going to benefit rather than across the board. That's when this starts to become valuable.
In addition, there are a number of potential routes that involve using certain types of medication that might affect these particular pathways. Again, we have evidence from animal studies that this might be the case, but obviously you don't go giving medications for long periods to babies unless you're absolutely confident you've got it right. Without being able to identify the babies for whom it would be appropriate to try some of these techniques, we can't tell whether they work.
This current study is the first phase. If we can confirm that this does work and can identify babies by doing these other complicated analyses, we can eventually identify a group of babies where as many as one in ten of them might die if they are not helped. Then, we can start focusing on that group and really trying to work specifically for them and with them to try and help them.
What implications could a screening tool for SIDS have?
Well, I think the first and most simple point is that if we can identify a group of babies who are at very high risk, then we can actually work with families and make absolutely sure that those babies are never put in a position where their risk is increased by having their heads covered, being positioned on their tummies, being exposed to tobacco smoke, getting too hot or being in the wrong place, for example.
The evidence we have suggests that if we can work with families on a one-to-one basis and use those very simple techniques to take away all the risk factors that we can identify, we may well be able to prevent quite a few deaths. However, we can’t do that level of one-to-one investigation and care when we're dealing with 700,000 new-borns a year, which is what we have in the UK.
How does your study aim to learn more about unexpected death in older children?
SIDS is very rare in children aged as old as 3 or 4 years, but there are some who die suddenly and unexpectedly. Because that is so uncommon, relatively little is known about the deaths of those children. I've been collaborating with a group in the US for about 15 years now trying to learn as much as we possibly can about those children and what contributes to their deaths.
Many of the features are rather similar to those of babies who die at a younger age. We really have very limited information about those individuals because most of the studies of SIDS have been from limited populations, in a part of the country and over a part of a period of time.
What we now want to do is to collect information about any of those babies across the whole of the UK who have died in the last few years, so that we can learn as much as we possibly can about the characteristics that contribute to their deaths and, by implication, how we might be able to prevent them.
How is this research being funded?
The funding comes from the Lullaby Trust, which is the organization in the UK that leads the way in terms of the investigation and understanding of SIDS in infants and children. The Lullaby Trust, which used to be called the Foundation for the Study of Infant Death, is the main agency that is coordinating and providing the funding for this and, indeed, will be helping us to recruit the families whose babies have died.
They have acquired the money through a number of routes. We have very generous donations from families in Australia we have donations from two family organizations in the US.
We also have parents whose baby died a couple of years ago in the UK, who have been very generous and raised a lot of support funding for the Lullaby Trust to support this project. Very much of the money has come from families who have been affected by the tragic loss of a child.
When will recruitment for participants begin and how can people get involved in the study?
We're recruiting two groups of babies. The first is through the families of babies or young children who have died suddenly and unexpectedly at any time in the last six years… anytime from 2010 onwards.
We’re asking that any family who has had a baby or young child die suddenly and unexpectedly makes contact with the Lullaby Trust. We’ll tell them about the project and if they agree to take part, then we will interview them and collect all the information about their baby and what happened.
Most importantly, we’ll also be able to go to the repository and actually pull out the hearing test for their baby. We have arranged that every hearing test on every baby in England that's been done since the beginning of 2010 is now stored on a single computer in London, in a way that will be accessible if we have parents’ permission. We can't access it without their permission, but if they give us that permission we'll be able to access their recording and use that to investigate.
The other groups we're looking at are babies born in Bristol and babies born in Birmingham. Those are normal, healthy babies because obviously we need to know what the difference is between healthy babies and babies who die.
We started the recruitment in Bristol in June and we’re starting in Birmingham on 1st September. We'll be talking to each family, asking them to allow access their baby's hearing recording and collecting some information about the baby and their family.
The reason we're doing this in these two different cities is that Bristol and Birmingham are very different cities, with a very different ethnic and cultural mix. Also, there are two systems that are used to record the hearing screening in the UK. One of those systems is used in Bristol and one is used in Birmingham.
They give a similar recording, but you can only compare directly things that are made on the same system, so we're recruiting half the control babies in Bristol and half in Birmingham.
How many babies are you looking to recruit?
We're hoping to collect information from about 160 families whose babies have died suddenly and unexpectedly, from the beginning of 2010 to the end of this year. Over that six year period, we anticipate there probably being around 1,500 babies who have died suddenly and unexpectedly. We want to recruit about 160, so just over 10% of them.
For the controls, we're going to recruit 100 in Bristol and 100 in Birmingham, so that we'll be able to make very detailed comparisons.
If anyone who is reading this knows of a family who has lost a child or baby in the last few years, please put them in touch with the Lullaby Trust. I've now personally interviewed and met almost a thousand families who have lost a child in this way and one thing that is so important to almost all of them is that everything that has happened to them, they don't want to happen to anyone else and they're so willing to share their information so that we can make that progress.
All of the progress that we have made to date has depended on families who have gone through that awful tragedy being willing to share their experience and to tell us what happened so that we can try and stop it happening in the future.
Where can readers find more information?
http://www.lullabytrust.org.uk/
About Professor Peter Fleming, CBE, FRSA, PhD, MB ChB, FRCP (London), FRCP (Canada), FRCPCH
After undergraduate training in Bristol and postgraduate training in pediatrics at the Hospital for Sick Children, Great Ormond Street, London, and the Hospital for Sick Children, Toronto, I returned to Bristol.
From 1978 - 2012 I worked in the Neonatal Intensive Care Unit at St Michaels Hospital and the Children’s Sleep and Developmental Physiology Laboratory at Bristol Children’s Hospital, and also led the service for children on long term ventilatory support for the Southwest of England.
Since January 2013 I have worked primarily in research and teaching.
In 1983, I established the Avon Infant Mortality Study and since that time have continued to provide care and support to families bereaved by perinatal and infant deaths particularly the sudden or unexpected death of an infant or child within the Avon area (population 1million).
My research has included extensive studies of normal physiological development of infants and children, both in the laboratory and community setting and over the past 35 years I have led several large-scale epidemiological studies of factors contributing to unexpected deaths in infants and children.
Our studies in Avon were amongst the first to identify the importance of infant’s sleeping position, heavy wrapping, exposure to tobacco smoke and other features of the sleep environment as contributory factors to unexpected death in infancy.
I was the lead clinician in the UK “Black to Sleep” Campaign in 1991, which led to a dramatic fall in the numbers of infants dying suddenly and unexpectedly. I have been involved as a collaborator and advisor to several similar campaigns in other countries. This work is estimated to have led to the saving of over 15,000 infants’ lives in the UK, and over 100,000 worldwide.
I continue to conduct detailed research on epidemiological and physiological factors contributing to unexpected deaths in infancy and have co-authored more than 360 scientific publications.
The approach to the care and investigations of families bereaved by the sudden expected death of their child that we pioneered in the Avon area has since 2008 been adopted nationally in England under The Children Act 2004.
Since 2010 I have led a project in Neonatal Units in the Southwest of England developing approaches to better inform parents of preterm infants about their needs and care, before and after discharge from hospital. The “Train to home” that we have developed improves parents’ knowledge and confidence, and has led to reduced use of out of hours services after babies are discharged home.
We applied the techniques and knowledge derived from the studies of childhood deaths in the largest study yet conducted into factors contributing to premature deaths of people with learning disabilities.
Publication of the results of this study in the Lancet in 2014 led to government pledges to respond to the deficiencies and service failures identified. In May 2015 we were awarded a £2.3 million 3-year Grant by NHS England and are now establishing a National monitoring system for deaths of people with Learning Disabilities, modeled on the Child Death Review Programme.
In May 2016, with funding from the Lullaby Trust, we commenced a new national study investigating the possible links between subtle features of the routinely collected new-born hearing screening test and the risk of Sudden Infant Death. This study aims to identify infants at increased risk of unexpected death in infancy or early childhood, in order to facilitate targeted interventions that may reduce the risk to these infants.