A new study has shown that some of the sub-strains of the bacteria that commonly live on our skin have become resistant to common infections – or in other words turned into superbugs. Infections with these strains thus could become untreatable with the antibiotics available and may turn life-threatening, warn researchers.
According to a recent UK government report, emergence of the superbugs that are resistant to the commonly used antibiotics could push humans back into the “dark ages of medicine” where specific antibiotics were not available for all infections. This report says that if prompt action is not taken now, up to 10 million people could die of infections by these superbugs by 2050.
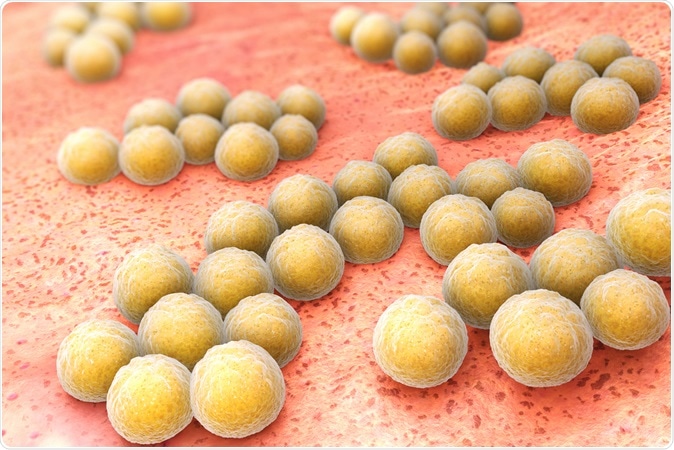
Methicillin-resistant Staphylococcus aureus (MRSA) is a bacterium responsible for several difficult-to-treat infections in humans. Image Credit: Tatiana Shepeleva / Shutterstock
In this latest study the team has looked at sub strains on the commonly present human pathogen called Staphylococcus aureus or staph. Staph has long since developed resistance to the bacteria Methicillin and has emerged as MRSA or Methicillin Resistant Staph aureus which has been notoriously difficult to treat. One of Staph’s sub-styrains commonly lives on the skin surface. This is called Staphylococcus epidermidis (S. epidermidis). Staph epidermidis is fast emerging as a cause for hospital-acquired infections. It needs to be treated with an antibiotic called vancomycin. Vancomycin is commonly combined with another antibiotic called Rifampicin for the treatment of Staph epidermidis infections.
In 2012 however a patient was admitted for a simple procedure and he acquired Staph epidermidis infection which necessitated a three month hospital stay. Dr. Jean Lee from the University of Melbourne's Department of Microbiology and her colleagues and team including her PhD supervisor Professor Ben Howden started investigating this particular case of drug resistance. The team spent the next six years trying sequence the genetic code of this stain of the bacteria. They noted that Staph epidermidis has three distinct genetic lineages. These mutations were compared globally with other strains. One in 10 countries in the UK, America and Europe showed emergence of the same mutations that could lead to these superbugs that resisted the antibiotics. For this study the team collected hundreds of Staphylococcus epidermidis isolates from 78 different medical institutions situated in 10 different countries worldwide.
According to Lee, all of these three strains of the Staph epidermidis have spread worldwide and are resistant to the commonly used antibiotics. The 2012 case was not a one-off case, she adds. In fact some of the samples of the bacteria have shown that they are resistant to the strongest “last-ditch” antibiotics as well. This renders their infection potentially untreatable she explains. She added that this bacteria commonly is present over the skin and can enter into the body via the medical devices that are introduced within the body such as feeding tubes, catheters, intravenous lines etc.
As of now the degree of prevalence of these strains around the world and their degree of severity of infection among patients is not explored in details, the authors explain. There is an emergence of a handful of reports that speak of Staph epidermidis resistance to antibiotics. Since these infections are commonly acquired within the intensive care when the patient’s immunity is low, the situation is more worrying. Professor Howden says, “Catheters and other implanted devices are frequently impregnated with antibiotics as a strategy to prevent infection, however this approach may be promoting the development of resistance. Also, these infections are most prevalent in intensive care, where patients are sickest and strong antibiotics are liberally prescribed, promoting the development of additional resistance.”
At present a deeper understanding of the method of spread of this superbug and prevention of the same is being sought. Professor Howden says that there needs to be an “international monitoring system” that would provide data on prevalence of S. epidermidis and its impact. The system would also help measure antibiotic resistance and the infections caused by this strain he said.
The research was published in the latest issue of the journal Nature Microbiology.
Citation: Global spread of three multidrug-resistant lineages of Staphylococcus epidermidis, Jean Y. H. Lee, Ian R. Monk, Anders Gonçalves da Silva, Torsten Seemann, Kyra Y. L. Chua, Angela Kearns, Robert Hill, Neil Woodford, Mette D. Bartels, Birgit Strommenger, Frederic Laurent, Magali Dodémont, Ariane Deplano, Robin Patel, Anders R. Larsen, Tony M. Korman, Timothy P. Stinear & Benjamin P. Howden | Nature Microbiology (2018) https://www.nature.com/articles/s41564-018-0230-7